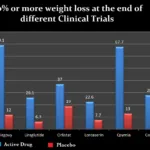
Foods to avoid with Kidney disease and diabetes include foods that have a high glycemic index, foods rich in proteins, salted foods, and foods with a high potassium and phosphorus content.
Diabetes is a disease manifesting primarily as hyperglycemia and later resulting in multiple organ diseases, kidney disease in particular.
The first principle of a diabetic diet is to reduce refined sugars and foods with lots of calories.
Once a person develops kidney disease, foods that burden our kidneys with lots of nitrogenous waste are also reduced.
So, we are left with very few choices. Our nutritionist has made it easy for you by providing a list of foods that a diabetic person with kidney disease can eat without risking the kidneys.
At the end of the article is a sample diet chart of around 1200 calories that a diabetic person with kidney disease can follow.
| Read: |
What is a Diabetic Kidney Disease or Diabetic Nephropathy?
Diabetic Kidney Disease is a complication of long-standing diabetes. It is the leading cause of ESRD (end-stage renal disease) worldwide.
DN (Diabetic Nephropathy) remains asymptomatic for years. The first two stages of diabetic nephropathy, the “stage of hyperfiltration” and the “Incipient stage” are not even detectable on regular blood tests.
The first two stages are followed by the stage of proteinuria. When the proteins from the blood get excreted in the urine in small amounts (30 to 300 mg per 24 hours) it is called “microalbuminuria” or stage III Diabetic kidney disease.
In the fourth stage, proteinuria worsens and exceeds 300 mg per 24 hours. Stage V diabetic kidney disease is characterized by rising creatinine.
Patients may notice swelling of the legs and around the eyes in the third stage and onwards. Passing frothy urine may be noticed by the patient as well.
| Read: |
How does diabetes cause kidney disease?
Kidneys perform the vital function of filtration. During the process excess amount of any substance present in the blood is excreted out in urine, with continuous high blood sugar levels in uncontrolled diabetes, the filtration ability of the kidneys gradually falls, and this causes defective membrane permeability.
As a result, the membrane becomes permeable to proteins (which must remain in the blood) and they are excreted out.
In the initial stages, the blood protein albumin is found in small quantities in urine. This condition is known as “Microalbuminuria”.
The presence of albumin in the urine is the first indicator that diabetes has started affecting the kidneys.
If this remains untreated, greater quantities of albumin are excreted out leading to “Macroalbuminuria”.
Diabetic Nephropathy progresses slowly. Following are the symptoms that appear with time, if proper measures are not taken.
Stage of Diabetic Nephropathy | Time | Characteristic Symptoms |
| Increase in size and activity of the kidney | At diagnosis |
|
| Changes to the kidney tissue | 2-5 years |
|
| Onset of nephropathy | 5-15 years |
|
| Clinical manifestations of Nephropathy | 10-25 years |
|
| Renal insufficiency | 15-30 years |
|
| Read: |
Who is at risk of developing Diabetic Kidney Disease:
It is important to know that not all diabetic patients have kidney disease but, some conditions that are potential risk factors include:
- Hyperglycemia
- High blood pressure
- Smoking
- Cardiovascular Disorders
- Uncontrolled Diabetes Mellitus
- High salt consumption
- Physical Inactivity
- Obesity
The three important factors, apart from uncontrolled diabetes, that increase the risk of developing Diabetic Kidney Disease are:
- Hypertension
- Smoking, and
- NSAIDs (non-steroidal anti-inflammatory drugs)
| Read: |
Nutritional Guidelines for Diabetic Nephropathy:
Although diabetic nephropathy cannot be completely cured, its progression can be slowed down with the help of Medical Nutrition Therapy.
Nutrition management for diabetes includes management of blood glucose levels, blood lipids, hypertension, and healthy body weight.
However, these targets are harder to achieve for patients with diabetic nephropathy.
Diet therapy is affected by individual effects of nutrients on kidney functions and renal hemodynamics.
Diabetic kidney disease requires very strict observation of dietary recommendations for carbohydrates, proteins, fats, and management of electrolytes depending on their individual kidney function.
Weight management and physical activity have also been proven to have a great role.
Furthermore, dietary recommendations may differ with different stages of diabetic kidney disease.
| Read: |
Common Foods to Avoid with Kidney Disease and Diabetes:
How much glucose is recommended in patients with kidney disease and diabetes:
A very important tool for good diabetes therapy is the maintenance of blood glucose levels below the renal threshold (250 mg/dl) so that it does not pass into the urine.
The characteristic features of patients with kidney disease are insulin resistance and glucose intolerance. For the management of glucose, the target of HbA1c should be <7 %.
Blood glucose levels in the body are affected by the amount and type of carbohydrates. For better management of blood glucose, foods with a glycemic index <55 must be consumed.
Low GI (glycemic index) foods include whole grains, cereals, carrots, broccoli, celery, cauliflower, etc.
How much dietary fiber is recommended in patients with kidney disease and diabetes:
Dietary fiber lowers blood sugar in diabetic patients. Soluble and Insoluble fiber reduces the digestion time of carbohydrates and hence aids in improving insulin sensitivity.
The FDA recommends 14g of fiber per 1000 kcal and this amount can be increased up to 35g according to the patient’s needs.
Daily Fiber Intake should range from 14 G to 35 G
Among the Foods to Avoid with Kidney Disease and Diabetes, Dietary Restriction of Proteins is very important:
Protein is the major regulatory factor in nephropathy. Reducing the amount of dietary protein intake results in reduced protein excretion and a regulated glomerular filtration rate is achieved gradually.
Many experiments done on animals and humans have shown lower protein excretion in urine when a low-protein diet is consumed, ultimately causing a delay in the progression of diabetic nephropathy.
Most of the patients do not focus on their dietary patterns and rather consume excessive quantities of carbohydrates and proteins, this excessive intake is harmful and needs to be adjusted in every diabetic patient with or without any comorbid condition.
The recommended protein-restricted diet of 0.6-0.8 g/kg protein in a day aids in improving GFR to some extent.
For Diabetic nephropathy patients with disease stage 1 or 2, 0.8 g/kg per day is generally recommended, which means, for a person with an ideal body weight of 68 kg the recommended daily percentage of protein will be 68 × 0.8 = 54 grams of protein.
For a person with diabetic nephropathy, stage 3 or above the recommended value of dietary protein is 0.6 g/kg so, with a person weighing 68 kg, the recommended protein amount will be 68 × 0.6 = 40 grams protein per day.
Although, the recommended protein amount for dialysis-dependent patients is about 1.2 g/kg (81 grams) due to dialysis-induced protein loss.
Protein cannot be completely excluded from the diet but patients with diabetic kidney disease need to carefully monitor their protein intake according to their disease stage, glycemic control, and overall nutritional status.
Patients must be given proper counseling about medical nutrition therapy. Plant-based proteins should be used instead of animal proteins.
In the case of animal protein, lean meat from fish and poultry is recommended. Some amount of protein is also present in grains and starchy vegetables so it must be carefully adjusted within the recommended amount of protein.
Recommended Protein intake is 0.6 – 0.8 gm/kg/day
Which Fruits and Vegetables can be used/ avoided in a diabetic person with Kidney Disease:
Fruits and vegetables with low potassium, phosphorus, and sodium are preferred in DKD patients.
- Some of the fruits that are not harmful and can be taken by a diabetic person with kidney disease include
- Apples,
- Red Grapes,
- Strawberries,
- Cherries,
- Pear,
- Peach,
- Plum,
- Apricots, and
- Watermelon.
- Fruits that need to be restricted include:
- Vegetables are mainly adjusted as the biochemical test results of a patient’s potassium and phosphorus concentrations in the blood.
- Vegetables good for a diabetic patient with kidney disease include:
- Cauliflower,
- Cabbage,
- Cucumber,
- Eggplant,
- Broccoli,
- Carrots, etc.
- Fruits and vegetables need to be adjusted carefully according to the patient’s blood concentration of potassium and phosphorus, Malnutrition and muscle wasting can occur if the patient does not get a proper nutrient-dense diet.
- Due to the protein restriction, carbs need to be supplied in adequate quantities to meet the extra requirements of the body.
How much fat should a person with Diabetes and Kidney disease consume per day?
The optimal amount of fats for a person with diabetes and kidney disease has not been defined yet.
The general guidelines suggest that reduced intake of saturated fat and trans-fat contributes to a reduced risk of cardiovascular diseases.
In a person with diabetes and kidney disease (diabetic kidney disease), saturated fats are limited to <7% of total calories.
In comparison to the quantity of fat, its quality has a greater effect. Polyunsaturated fatty acids (PUFA’s) and Mono-unsaturated fatty acids (MUFA’s) are known to have a beneficial impact on the control of hypertension and dyslipidemia.
In recent studies, it has been observed that higher dietary intake of PUFA’s lowers the incidence of End-Stage Renal Disease (ESRD).
What are phosphorus-containing foods that a kidney patient should not take?
Phosphorus is a mineral that is found in bones and teeth along with Calcium. With impaired renal function, the excretion rate of phosphorus is decreased which results in an increased amount of phosphorus in the blood.
Therefore, the intake of foods with high phosphorus content must be reduced.
Phosphorus intake for Diabetic kidney disease patients must be 800-1000 mg/day, to prevent hyperphosphatemia. Foods with a High protein-phosphorus ratio should be restricted.
Some of the products with high phosphorus content include:
- Milk and milk products
- Soft drinks and other beverages
- Frozen and Canned products
- Processed food items.
Vegan diet consumption must be encouraged and plant protein should be preferred because only 50% of phosphorus is absorbed from vegetable sources.
How much Salt is recommended for a diabetic person with kidney disease:
Sodium restriction in Diabetic Kidney Disease (DKD) is similar to that of Chronic Kidney Disease (CKD), a low amount of sodium has been proven to be beneficial as it affects blood pressure, the efficiency of anti-hypertensive medication, and proteinuria.
Dietary sodium intake for a person with diabetes and kidney disease is 1,500-2,000 mg/day. Sodium restriction is categorized as:
- Mild restriction (1,500-2,000 mg/day),
- Moderate (1,000-1,500 mg/day) and
- Extreme (<1,000 mg/day)
according to the patient’s blood pressure.
Similarly, calcium intake should be < 2000mg/day inclusive of supplements.
Avoid drugs that may damage your kidneys:
It is the poisonous effect of some drugs or medications on kidney function.
Patients with Diabetic Nephropathy must avoid nephrotoxic agents like Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) and Cyclooxygenase 2 (COX-2) inhibitors.
These drugs can directly damage the kidneys and reduce the glomerular filtration rate (GFR). Diabetic kidneys are especially vulnerable to NSAIDs.
Preferred pain medications include:
- Paracetamol
- Topical creams and ointments
- Pregabalin may be used for neuropathic pains, and
- Codeine and Tramadol (these drugs are addictive and may be used for short-term only).
| Read: |
Dietary Guidelines for Diabetic Kidney Disease
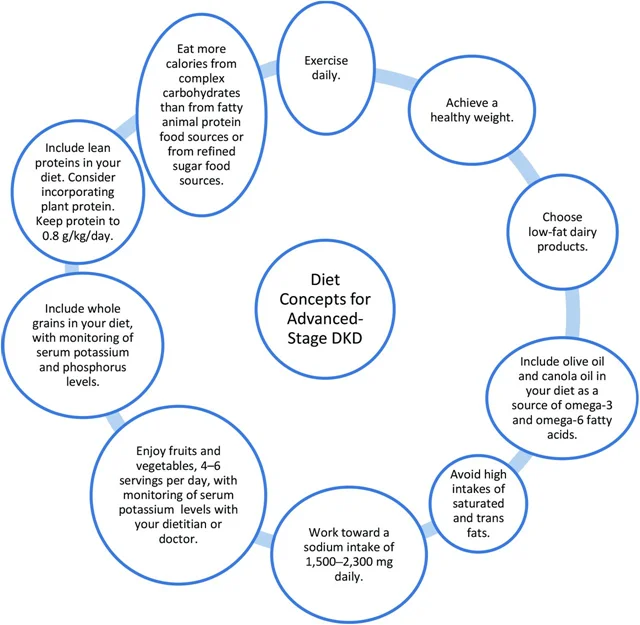
- Blood glucose control is important to prevent the progression of diabetic nephropathy.
- Hyperglycemia plays a key role in the development of diabetic nephropathy, glucose management within time can slow the progression of the disease.
- Small meals must be taken as compared to large meals to avoid increased blood sugar levels.
- Meal plans should be carefully made by a Registered Dietitian so that carbohydrates, proteins, and fats are in the right proportions.
- Carbohydrate amounts should be kept constant in all meals to avoid an increase in blood sugar levels.
- Meals and Medication must be coordinated to avoid hyperglycemia and hypoglycemia.
- The number of minerals must be carefully focused on in every meal that is planned.
| Read: |
Dietary patterns for patients with Diabetes and Kidney Disease to follow:
Diet therapy in patients with diabetic nephropathy plays a substantial role in delaying the progression of the disease.
A diabetic diet ensures the consumption of a healthy diet. Improper selection of foods may result in disease progression.
Whereas a Diabetic nephropathy diet is designed to slow down the progression of renal disease, hypertension, and hyperlipidemia, and control blood glucose levels along with careful monitoring of sodium and potassium levels.
Experiments and research suggest that focusing on diet patterns for managing chronic diseases is more beneficial than focusing on the intake of individual nutrients.
The Mediterranean diet includes an enhanced intake of complex carbohydrates, whole grains, fruits and vegetables, seeds, beans, fish, and olive oil.
Intake of trans fat products and other animal proteins along with full-fat dairy products is decreased. These dietary patterns are a new approach to the prevention of Diabetic Nephropathy.
| Read: |
A Sample Diet Plan for Diabetic Patients with Kidney Disease:
Time | Serving | Food Item | Calories |
| Breakfast 8:00 AM | 2 slices 6 oz | White Bread + Egg white Yogurt | 458 |
| Snack 11:00 AM | 4 1 | Apricots Peach | 60 60 |
| Lunch 2:00 PM | 1 small 4-5 tbsp | Barley chapatti Vegetable curry | 242 |
| Snack 5:00 PM | 1 glass | Pomegranate juice | 80 |
| Dinner 9:00 PM | 1 disc size 1 slice | Chapatti Fish | 286 |
| Bed Time 11:00 PM | 1 glass | Skim milk | 100 |
Total calories: 1286 kcal
- The above-mentioned diet chart must be followed with all foods cooked in olive oil along with a restricted amount of sodium and trans fats.
- Calorie intake is less due to weight management in diabetic patients.
- Small meals with short intervals must be beneficial for the proper management of the nutrition care process
- All patients must regularly monitor their glucose levels before and after taking the meals
- Biochemical tests must be done to assess the status of Albuminuria and Glomerular Filtration Rate (GFR)
- There are separate dietary management techniques for patients undergoing dialysis and those with End-Stage Renal Disease (ESRD)
| Read: |