Diabetic hand infection is a serious, debilitating illness. It can impair a person’s ability to perform daily tasks, including simple tasks such as changing clothes, cleaning their body, washing their face, and even eating.
Because hands are relatively cleaner than other body parts, infection of the hands is relatively uncommon.
In addition, infections of the hands are generally picked up earlier as they are picked up earlier because they can be easily noticed.
Here is the story of a patient who came to us with a diabetic hand infection after he had angioplasty done.
Diabetic Hand Infection After Angioplasty:
A middle-aged man underwent angioplasty for coronary artery disease. One day after the procedure, the patient developed a fever, which was very high grade, documented up to 104 F, along with chills.
The patient complained of redness and swelling in the left hand where the procedure was performed.

He consulted his cardiologist, and he was put on oral antibiotics, however, his symptoms progressed.
He developed a pus pocket at the dorsal aspect of his hand, which was drained using a small incision.
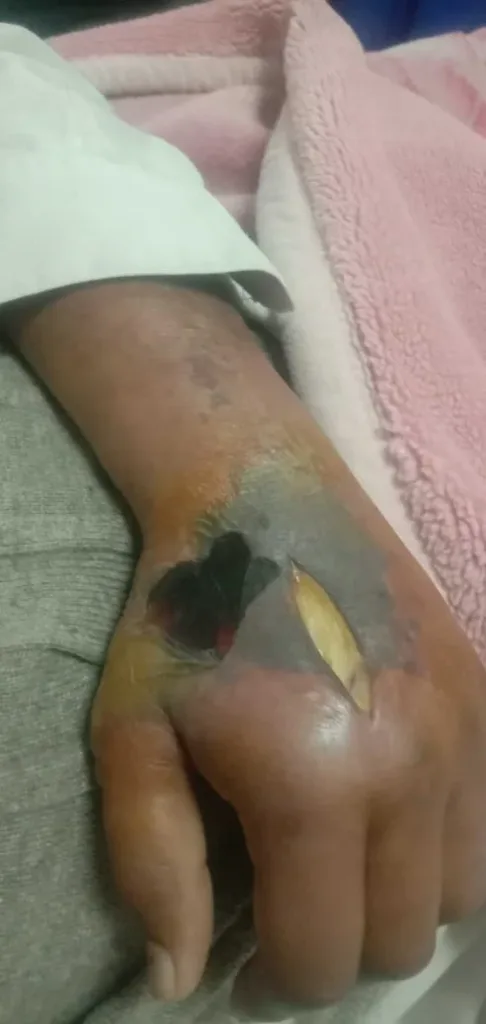
The pain slightly improved, but the infection spread to the deeper tissues. The skin of the hand sloughed off, and deeper tissues got exposed.

He was hospitalized and was given IV antibiotics. The patient also had uncontrolled type 2 diabetes for which he was taking oral anti-diabetic medications.
Despite IV antibiotics, his hand infection worsened. He visited a plastic surgeon at another hospital, where he was continued with the IV medications, and debridement was done.
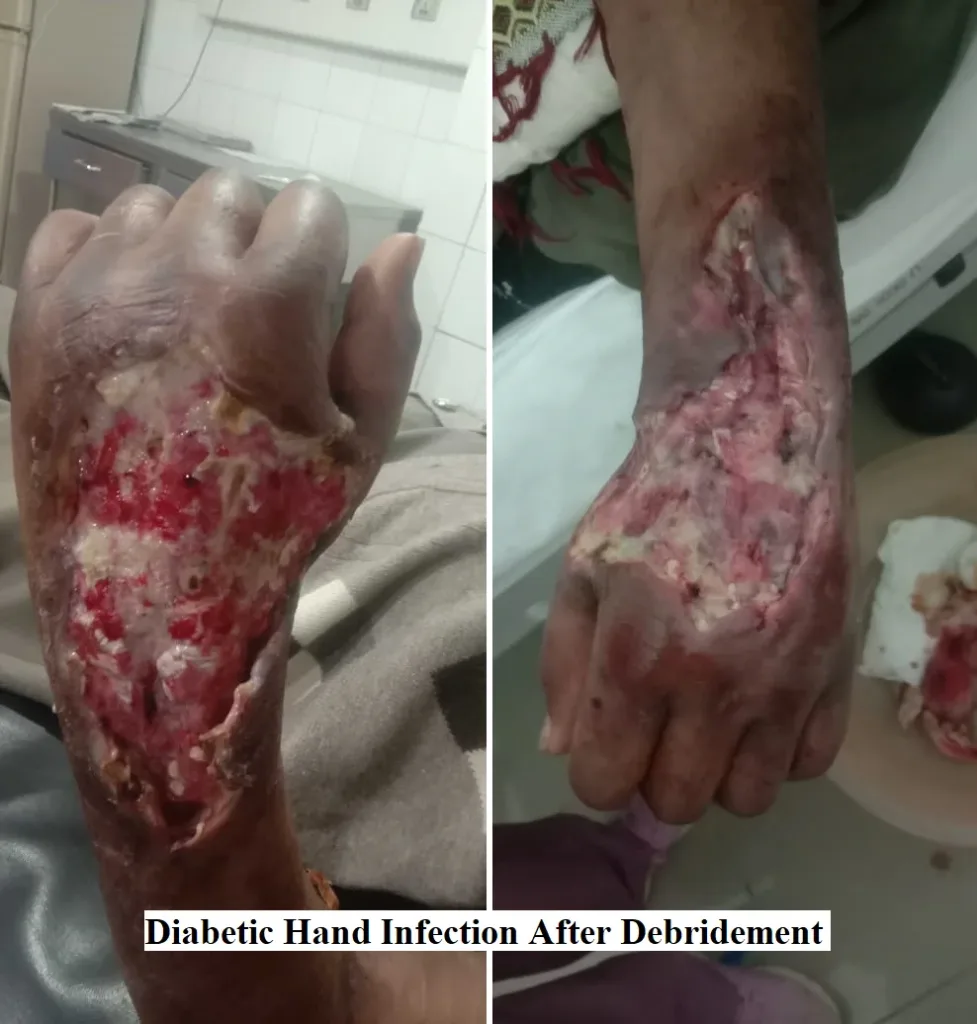
All the infected skin was removed. His fever slightly improved, but after another 2 days, he developed swelling of the whole left arm, predominantly the skin around the left elbow joint.
The plastic surgeon decided to extend the excision up to the elbow, which alarmed the patient and his relatives.
At Our Hospital …
When he visited our outpatient department, he was toxic and depressed. He was advised admission but the patient was not willing.
The patient had no prior cultures of the wound available, and we could not withhold antibiotics.
Wound debridement was done, and cultures were sent, but he was put on triple antibiotics including:
- Moxifloxacin,
- Linezolid, and
- Clindamycin.
The patient was put on basal bolus insulin, and tight glycemic control was achieved. A small nick was given to the site of maximum swelling around the elbow joint.
Continuous pus discharge was observed from the skin over the elbow. After 3 to 4 days, the fever settled, and the swelling gradually started improving. Cleaning of the wound and sterile dressings were done two times a day.
After 21 days, linezolid was discontinued. Clindamycin and moxifloxacin were continued for 3 months. Gradually, granulation tissue appeared, and the wound healed with scarring.

He was advised to undergo physiotherapy during the healing phase. After the antibiotics were stopped, the patient was referred to a plastic surgeon to deal with the scarred hand.

A Brief Discussion About Diabetic Hand Infection:
A diabetic hand infection is one of the serious complications of diabetes. It is associated with a marked functional disability if not treated timely manner.
Diabetes can affect the hands in many ways, diabetic hand infection is one of them. Here is a list of complications of diabetes in which the hands are primarily affected [Ref]:
- Dupuytren’s contracture,
- Stenosing tenosynovitis (trigger finger),
- carpal tunnel syndrome (CTS),
- Charcot neuroarthropathy,
- Reflex sympathetic dystrophy, and
- diabetic cheiroarthropathy
Diabetic hand infections can vary in severity from mild to rapidly progressive disease. It may spread rapidly to the deeper tissue and involve the whole limb.
Patients may develop fatal sepsis within days. The condition has also been termed “Tropical Diabetic Hand Syndrome” [Ref]
What is Tropical Diabetic Hand Syndrome?
Tropical diabetic hand syndrome is the term referring to a serious, rapidly progressive infection of the hand in a diabetic patient with uncontrolled diabetes.
Although it can affect any person throughout the world, cases of diabetic hand infections are commonly reported in developing countries because of obvious reasons, such as:
- Poor hygiene
- Uncontrolled diabetes
- Failure to start insulin timely manner
- Poor health and sanitation facilities
- More prevalent infections are due to the risky environment
- Old and dangerous beliefs
A diabetic hand infection is similar to a diabetic foot infection or infection anywhere in the body. However, patients with a diabetic hand infection become handicapped early in the disease process.
In addition, patients are likely to become dependent on others for simple household activities, including feeding, washing, and changing clothes.
What are the symptoms of a Diabetic Hand Infection?
The symptoms of a diabetic hand infection are similar to infection elsewhere. Patients may report pain, swelling, and redness of the hand.
A blister may develop. The infected area is usually warm. Fluid or pus discharge may be seen oozing out of the affected area.
The patient may also complain of fever and difficulty in moving the hand or performing simple daily tasks.
Signs of toxicity are common once the infection spreads and bacteremia develops. The affected hand may become black (gangrenous), necrotic, and scarred, requiring amputation.
Patients who recover may notice some functional impairment. Some patients may require a skin flap to avoid contractures and disability.
How is a diabetic hand infection diagnosed?
A diabetic hand infection is a purely clinical diagnosis. Investigations are done to evaluate for potential complications such as:
- Bone involvement (osteomyelitis),
- Nerve involvement,
- Blood vessel involvement (phlebitis),
- Muscle involvement (myositis),
- Compartment syndrome, and
- Systemic involvement
In addition, tests are done to evaluate for comorbid conditions such as diabetic control, heart disease, and kidney disease.
Blood cultures and wound cultures are essential to pinpoint the infection. Some patients may require a bone scan to rule out osteomyelitis.
Infections in diabetic hand and foot infections are frequently polymicrobial. However, tissue biopsy from the wound may result in identifying a single bacterium in up to 75% of the patients [Ref].
How is a diabetic hand infection treated?
The treatment of a diabetic hand infection includes a multi-specialty approach.
A tight glycemic control with a basal-bolus insulin regimen is preferred in most cases. A basal-bolus regimen consists of:
- Short-acting insulin (Regular insulin) or a rapid-acting insulin analog (Apidra, Novorapid, Humalog) is given three times a day before each meal
- A basal insulin (Lantus, Detemir, or Tresiba) is given once daily.
Antibiotics should be initiated before the results of wound cultures are available to stop the spread of the infection.
Broad-spectrum antibiotics covering Gram-positive, Gram-negative, and anaerobic organisms should be initiated.
Clindamycin has a good gram-positive and anaerobic cover. It can be given in combination with Moxifloxacin, which has good tissue penetration.
Vancomycin or Linezolid is frequently added in areas where MRSA (methicillin-resistant Staphylococcus aureus) is prevalent.
Wound debridement, frequent wound dressings, and limb elevation are required in almost all patients.
Amputation may be required to save the life of the patient in up to 13% of the cases [Ref].
- Premium Ingredients: Our tea blend features high-quality Berberine, aromatic Oolong, and refreshing Mint, all organicall…
- Mint Flavored: Enjoy the cool, crisp taste of mint that perfectly complements the robust flavors of Berberine and Oolong…
- Unsweetened with Zero Calories: Crafted for those who appreciate the natural flavors of tea, our blend is completely uns…
- AZO URINARY PAIN RELIEF MAX STRENGTH 24 COUNT: Fast, effective over-the-counter UTI symptom relief in 20 minutes or less
- INGREDIENTS: Contains Phenazopyridine Hydrochloride, the #1 ingredient prescribed by doctors and pharmacists targeting u…
- FAST & EFFECTIVE: Directly targets site of discomfort, so you can experience relief in as little as 20 minutes – somethi…

- POWERFUL ANTIFUNGAL CREAM: contains 1% Clotrimazole and natural ingredients to treat fungal infections while providing f…
- CLINICALLY PROVEN EFFECTIVE: Terrasil with Clotrimazole cures most fungal skin infections: athlete’s foot, bar rot, fung…
- UNIQUE PATENTED TECHNOLOGY: Only Terrasil Anti-fungal treatment cream contains Activated Minerals, backed by over 20 yea…

- USDA Organic Respiratory Health Liquid Drops: If your respiratory system is occasionally irritated by dry air or other m…
- Mullein Leaf Blend: The respiratory system is a system of great importance in our overall health. Not only does it aid i…
- Immune Support Supplement: And, did you know?? — the respiratory system also allows us to talk! This specially formulate…









