Obstructive sleep apnea syndrome is the intermittent collapse of the airways resulting in reduced oxygen saturation and disturbed sleep.
As the name suggests, there is airway obstruction in sleep that results in apnea (the breathing stops transiently) or hypopnea (the breathing does not stop completely but slows down or becomes very shallow).
Buy natural drops and a device to stop snoring
Obstructive Sleep Apnea Vs Pickwickian Syndrome:
Obstructive sleep apnea and Pickwickian syndrome or Obesity hypoventilation syndrome are two different terms used synonymously. However, these are slightly different.
In obstructive sleep apnea or OSA, apnea or Hypopnea occurs usually when the patient is asleep. On the other hand, patients with Pickwickian syndrome (or obesity hypoventilation syndrome), patients have apnea and hypopnea episodes even during awake timings.
All patients who have Obesity hypoventilation syndrome (Pickwickian syndrome) are obese. Contrary to that, obstructive sleep apnea may occur even in thin and lean patients.
You may like reading:
OSA can have serious consequences:
OSA and Pickwickian syndrome can have serious consequences. It may affect the heart, and brain, and can be life-threatening if the person is driving or operating heavy machinery.
Obstructive sleep apnea is not uncommon. Apneic and hypopneas episodes occur many times per night resulting in loud breathing or snoring, heart rate variation, and changes in oxygen saturation.
Patients are prone to develop Diabetes, Hypertension, Depression, Insulin resistance, Heart diseases, Pulmonary hypertension, Venous thrombosis, and sleep-related accidents.
Children can have OSA due to enlarged tonsils. OSA is common in obese individuals, the elderly, and male patients.
Other conditions may be associated with OSA (Obstructive sleep apnea) as mentioned in the picture below:
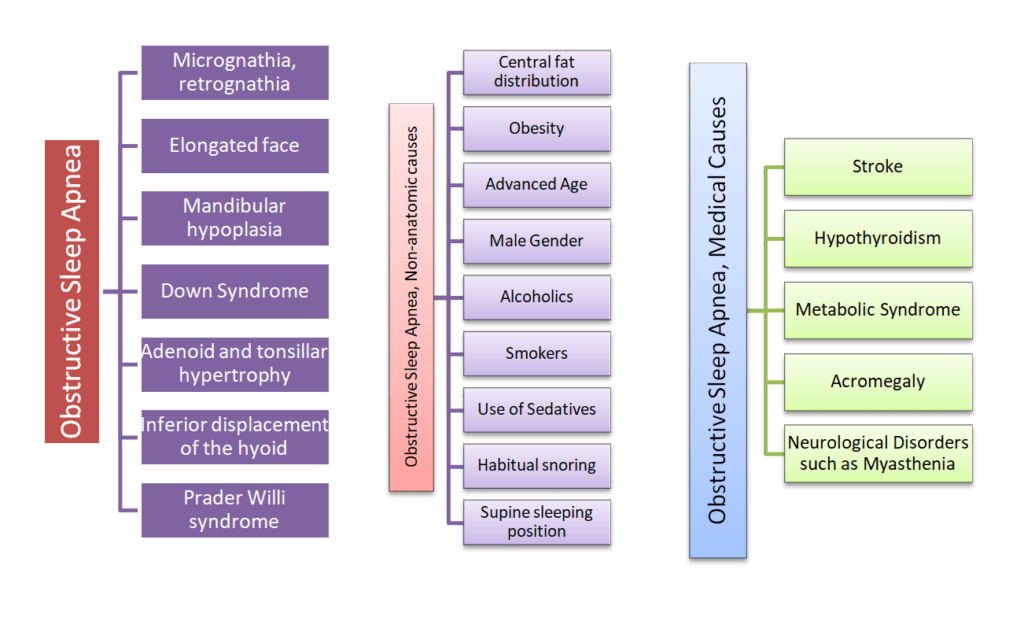
What are Apnea and Hypopnea?
When the muscle tone drops during rapid eye movement (REM) sleep, the airway collapses. When 90% of the airway collapses from its anterior or posterior sides, apnea occurs.
This episode can last for ten seconds or more resulting in oxygen desaturation or arousal.
When 30% or more of the airway collapses, hypopnea occurs. This episode can last for ten seconds or more and the patient desaturates or wakes up.
You may like reading:
What are the symptoms of Obstructive Sleep Apnea?
Adult patients with obstructive sleeping apnea are usually obese or overweight and experience loud snoring at night. Most patients have symptoms starting in middle age.
Patients may have a nocturnal awakening, irritability, palpitations, night sweats, nocturia, and insomnia.
Patients may have a larger-than-normal neck circumference (usually more than 17 inches in males), a crowded oropharynx (3 to 4 mallampati), and a larger tongue.
Patients may develop refractory atrial fibrillation, resistant hypertension, and stroke or heart disease.
Children may have attention deficit hyperactive disorder (ADHD), recurrent limb movements, night sweats, difficulty in maintaining sleep, nocturnal enuresis, and nocturnal reflux.
A physical exam can often be used to detect adenoidal facies and tonsillar hypertrophy. Hyponasal speech, high-arched palate, and tonsillar hypertrophy.
Patients with Down syndrome or any other hypotonia-related condition should be checked for obstructive sleeping apnea.
You may like reading:
The Epworth Sleepiness Scale:
The Epworth Sleepiness Scale is a tool that can be used to assess the likelihood of a patient falling asleep in different situations.
This can indicate inadequate nighttime sleep. A score of more than 10 indicates a sleep disorder and not generalized fatigue [Ref].
Would never nod off 0 | Slight chance of nodding off 1 | Moderate chance of nodding off 2 | High chance of nodding off 3 | |
| Sitting and reading | ||||
| Watching TV | ||||
| Sitting, inactive, in a public place (e.g., in a meeting, theater, or dinner event) | ||||
| As a passenger in a car for an hour or more without stopping for a break | ||||
| Lying down to rest when circumstances permit | ||||
| Sitting and talking to someone | ||||
| Sitting quietly after a meal without alcohol | ||||
| In a car, while stopped for a few minutes in traffic or at a light |
The STOP-BANG score is more specific for obstructive sleeping apnea. Each word is used for one symptom or risk factor.
A score of 0 to 2 is a low STOP-BANG score, 3 to 4 is intermediate, and more than 4 is a high-risk score. The higher the score, the greater the risk of the person falling asleep at unusual places.
The STOP-BANG Score:
| S | Snoring: Do you Snore loudly | Yes | No |
| T | Tiredness: Do you feel unusually tired and fatigued | ||
| O | Observed Apnea: Has someone observed that you stopped breathing | ||
| P | High blood pressure: Do you have hypertension? | ||
| B | BMI: Is your BMI more than 35 kg/m2? | ||
| A | Age: Are you older than 50 years? | ||
| N | Neck Circumference: Is your neck circumference more than 40 cm? | ||
| G | Gender: Are you male? |
Obstructive Sleep Apnea Diagnosis?
Nighttime polysomnography (PSG) is still considered the gold-standard test to diagnose obstructive sleep apnea. Patients are monitored using EEG leads, pulse oximetry, temperature, and pressure sensors to detect oral and nasal airflow.
Respiratory impedance plethysmography belts around the chest or abdomen detect motion. An ECG lead and EMG sensors detect muscle contractions in the chest, chin, and legs. One of two criteria can determine if hypopnea is present.
A decrease in airflow that is at least 30% from the baseline lasting for 10 seconds or more and associated with a minimum of at least 4% oxygen desaturation is considered significant.
Because they are affordable and easy to use, home sleep tests (HSTs) have become very popular.
These tests are suitable for adults who have a high probability of sleep apnea, but no other medical conditions (advanced heart failure, chronic obstructive pulmonary disease, or neurologic disorders).
The apnea-hypopnea index measures the average number of obstructive apneic or hypopnea episodes per hour.
Adults with obstructive sleeping disorders are diagnosed when the apnea-hypopnea index is greater than or equal to fifteen events per hour.
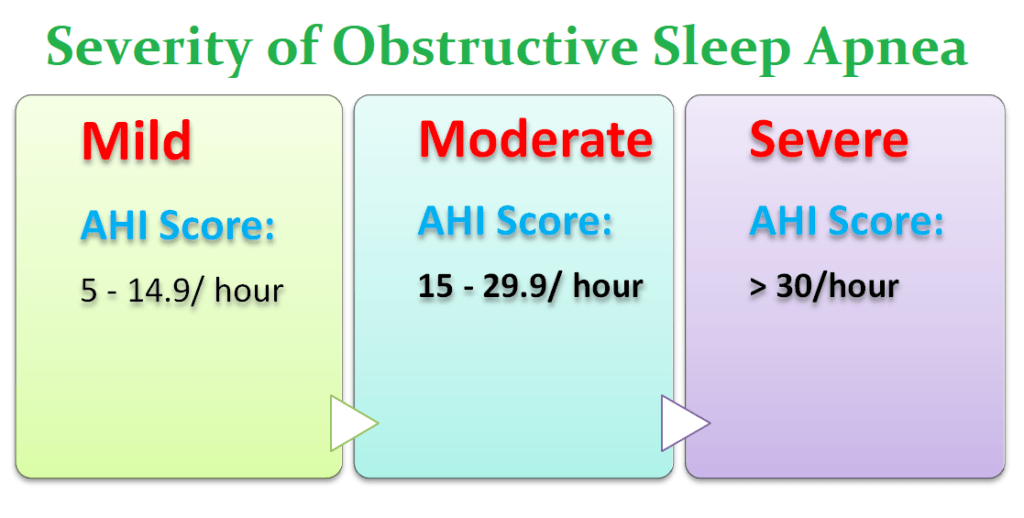
Events between 15 and 29.9 per hour are considered moderate. Events exceeding 30 per hour are considered severe.
Apnea-hypopnea indices between 5 and 14.9/hour are considered mild obstructive sleep apnea.
You may like reading:
Obstructive Sleep Apnea Treatment:
Adults should use continuous positive airway pressure (CPAP). Consistent use of CPAP nightly can lead to a near-complete resolution of symptoms.
Patients who are unable or unwilling or unable to use CPAP, or cannot access electricity reliably can use custom-fitted dental appliances to move the lower jaw forward and alleviate airway obstruction.
Candidates with adequate dentition and mild to moderate sleep disorder will benefit from this appliance.
BiPAP:
- BiPAP can also be used to treat severe obstructive sleeping apnea. Patients who need higher pressure settings (greater than 15 cm to 20 cm H2O) are more likely to tolerate it.
Nasal Steroids:
- All patients should be aware that nasal obstructions can be treated with nasal steroids to treat allergic rhinitis. Surgical repair of the collapse of the nasal valve is also curative.
A positioning device:
- A positioning device can be used to help obstructive sleeping apnea patients with strong positional components.
- Weight loss can be helpful and may reduce the severity of obstructive sleeping apnea. However, it is rarely curative.
Tonsillectomy:
- Tonsillectomy and adenoidectomy are the primary treatments for obstructive sleeping apnea in children. Considerations for surgery should balance the severity of symptoms, age, and physical exam.
- Mild cases may respond to nasal steroids such as fluticasone and montelukast (Singulair). Adults have a few options, but they are reserved for patients with severe sleep apnea or those who are unable to tolerate other non-invasive treatments due to the risks involved and their varying efficacy.
Uvulopalatopharyngoplasty (UPPP):
- Uvulopalatopharyngoplasty (UPPP) is a term used to describe surgically removing the uvula and tissue from the soft palate to create more space in the oropharynx.
- Sometimes, this is done together with an adenoidectomy or tonsillectomy.
DISE (Drug-induced sleep endoscopy):
- Preoperative planning has become easier with drug-induced sleep endoscopy (DISE). This allows for multiple levels of obstruction to be identified in these patients.
- This allows surgeons the ability to treat any hypopharyngeal, soft palate, or nasal obstructions in one surgery.
Maxillomandibular enhancement (MMA):
- Maxillomandibular enhancement (MMA) is another surgical option. In this procedure, both the upper jaws and lower jaws can be detached and surgically moved anteriorly to increase the space in the oropharynx.
- This procedure is most effective for patients suffering from retrognathia. It is less successful for older patients and those with larger neck circumferences.
Implantable hypoglossal neurostimulator:
- The implantable hypoglossal neurostimulator is a newer option. The implantable hypoglossal nerve stimulator stimulates the genioglossus (upper-airway dilator muscles) during apneas, causing protrusion of the tongue and relief from obstruction.
- A permanent surgically implanted device that is only a few years old and has limited long-term data should be considered in specialty centers that have experience in treating sleep-disordered breathing.
Tracheostomy (Tube in the throat):
- The obstructive sleep disorders can be treated with a tube to the throat. This will allow for the obstruction to be removed. Academic or specialty sleep centers are best equipped to handle this management option.
- These patients will face many challenges in managing their tracheostomy. Patients with severe sleep-disordered breathing who require tracheostomy often have multiple comorbidities that will need long-term home-based mechanical ventilation.
- This is not possible in most community sleep medicine practices.
Patients should be advised to stop taking opiates, benzodiazepines, opiates, and other antidepressants that may make their condition worse.
Patients should consider the effects of sleep duration on their health and prioritize getting 7 to 8 hours of sleep each night.
You may like reading:
Differential Diagnosis of Obstructive Sleep Apnea:
The following medical conditions can mimic OSA:
- Asthma
- Central sleep apnea
- COPD (Chronic obstructive lung disease)
- Depression
- GERD (Gastroesophageal reflux disease)
- Hypothyroidism
- Narcolepsy
- Periodic limb movement disorder
Complications of Obstructive Sleep Apnea:
Patients with OSA are at risk of developing the following medical conditions:
- Hypertension
- Heart diseases including Myocardial Infarction and pulmonary hypertension
- Cerebrovascular accidents including stroke
- Depression
- Accidents resulting from sleeplessness and sleep attacks while driving
It is important for obese patients with OSA to lose weight and avoid taking sleep medicines such as sedatives and hypnotics. Patients should also be instructed to avoid driving and use CPAP at night.
Patients may need to consult a dietitian for weight loss, cardiologists, pulmonologists, and psychiatrists in case they develop any complications of OSA. An endocrinologist may be consulted for diabetes and metabolic syndrome.
When compliance with CPAP is a major issue, other methods like nasal and oral devices may be used. Patients should also be evaluated for surgical correction.