Insulin is a life-saving medicine. It is the safest of all the medicines that are used to treat patients with Diabetes mellitus.
However, certain side effects may occur with insulin as well. Common Insulin side effects that you may develop include:
- Hypoglycemia
- Weight gain
- Edema
- Injection site reaction
- Retinopathy
- Neuropathy
- Hypokalemia
One common myth regarding insulin is that once you have started insulin injections, you can never go back on medicines. Insulin treatment can be started and discontinued at any time.
However, insulin is essential in the following situations:
- People with long-standing diabetes who have developed complications such as advanced kidney, liver, or heart diseases
- Those who have poor control of diabetes despite maximum doses of three or more diabetes medicines
- Type 1 diabetes mellitus
- Patients with an acute medical condition such as diabetic ketoacidosis, Hyperosmolar hyperglycemia, Heart failure, or stroke requiring hospitalization, and perioperatively.
- Gestational diabetes that is not controlled with metformin.
Insulin Side Effects and How to Manage Them:
Among all the medicines used to treat diabetes mellitus, insulin is the safest of all if properly administered and the dose is properly titrated.
The frequency of Insulin side effects may slightly differ with the different formulations. However, more or less, they are the same.
1. Hypoglycemia (Low blood sugars):
Hypoglycemia (or low blood glucose) is the most common side effect of insulin. The incidence of hypoglycemia is more common with prandial or bolus insulins compared to basal or long-acting insulins.
With prandial or pre-meal insulins, there is a sudden spike and the plasma insulin levels rise resulting in hypoglycemia.
In contrast to prandial insulins, basal insulins do not result in insulin spikes. They provide basal coverage and are least likely to be associated with hypoglycemia.
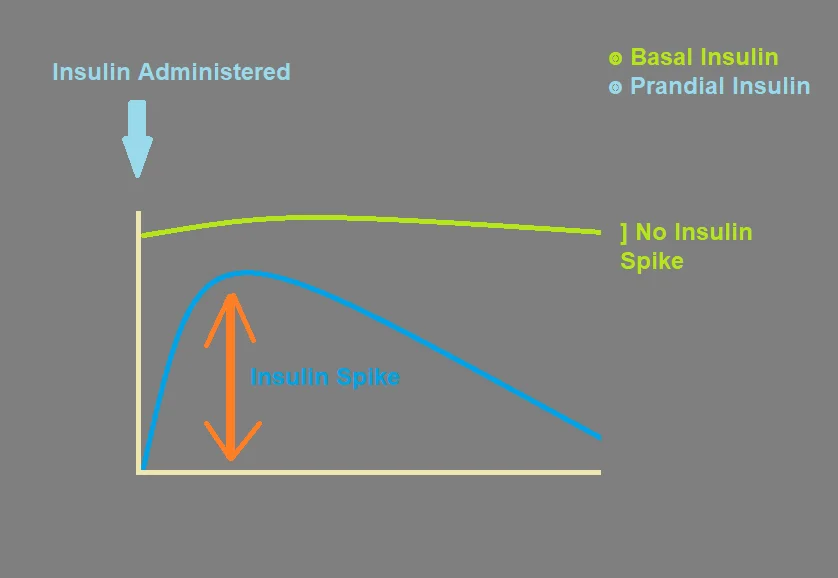
Since long-acting basal insulin does not have a peak time, the risk of hypoglycemia is much less compared to prandial insulin.
Among long-acting insulin, Insulin Icodec and Insulin Degludec have a much less incidence of hypoglycemia compared to insulin Glargine and Detemir.
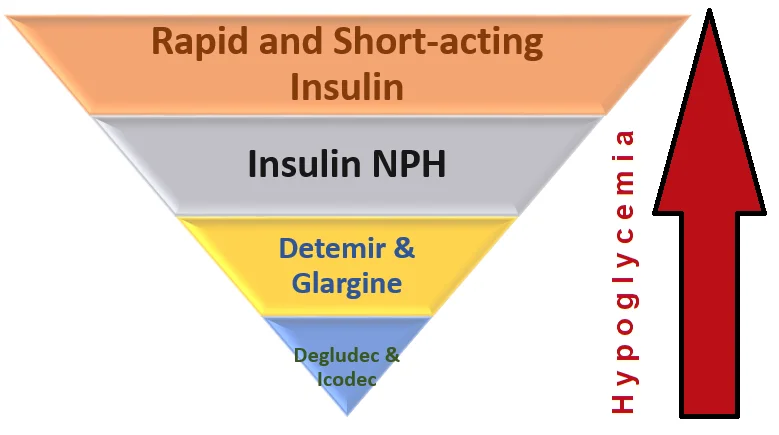
Compared to glargine, the incidence of nocturnal hypoglycemia was 25% less than that of Insulin glargine in one study.
How to manage and prevent hypoglycemia due to Insulin?
Hypoglycemia can be mild, moderate, or very severe. Mild hypoglycemia can be managed at home, while severe hypoglycemia needs emergency hospital visits to prevent brain damage.
Hypoglycemia occurs when the blood glucose falls to less than 70 mg/dl. In mild cases of hypoglycemia, patients can be asked to take some form of glucose at home. Patients may take sugar, candies, biscuits, fruit, or a glass of juice.
In severe cases, blood glucose usually falls to less than 54 mg/dl, and the person is severely symptomatic.
Home treatment is essential before the emergency visit. Patients are usually administered intravenous 50% glucose.
To prevent hypoglycemia, it is important to follow the following steps:
- Start insulin at a low dose and gradually increase the dose
- Start insulin with low hypoglycemic potentials such as Degludec or glargine.
- Discontinue sulfonylureas when initiating premixed or prandial insulins.
- Don’t miss meals.
- Reduce the dose of other oral hypoglycemic medications if administered concomitantly
- Recognize symptoms of hypoglycemia and manage them early at home.
2. Weight gain:
Weight gain is one of the common side effects of insulin. Insulin is an anabolic hormone. It enhances the entry of glucose into the cells and promotes glucose storage in the liver and muscles. It also inhibits lipolysis and the breakdown of proteins.
Weight gain is commonly observed when a patient is started on insulin treatment. It is especially concerning in obese patients who can not afford to gain a single pound.
Patients who are being overdosed and whose blood sugars are in the low normal ranges or those who have frequent hypoglycemia, are much more at risk of putting on more weight.
Patients who overeat or eat foods with a high glycemic index are also at risk of putting on weight more rapidly than usual.
Lastly, prandial insulins (short-acting and rapid-acting insulins) are associated with a much greater weight gain compared to basal insulins.
Insulin detemir is considered to cause less weight gain compared to Insulin NPH and Insulin Glargine.
How to deal with weight gain associated with insulin use?
Weight gain associated with insulin can be prevented by following these steps:
- Use the lowest possible dose of insulin that is effective and does not cause hypoglycemia.
- Avoiding hypoglycemia is essential since low blood glucose stimulates hunger, resulting in the intake of more carbohydrates and calories.
- Use insulin that is associated with the least weight gain, such as insulin detemir (Levemir).
- Use insulin in combination with other diabetes medications that neutralize the weight-gaining effects of insulin. These acceptable combinations may include:
- Metformin
- DPP IV inhibitors (sitagliptin, vildagliptin, and Linagliptin)
- GLP 1 analogs (Dulaglutide, Semaglutide, and Liraglutide)
- SGLT 2 Inhibitors ( Empagliflozin, Dapagliflozin, Ertugliflozin)
- Avoid using sulfonylureas such as glimepiride, glyburide, glipizide, and gliclazide.
- Avoid using thiazolidenediones like pioglitazone
- Take more dietary fiber and avoid consuming lots of carbohydrates.
- Exercise regularly for at least thirty minutes.
3. Edema and Fluid Retention:
Insulin causes weight gain by enhancing fat and sugar storage, however, some weight gain is also attributed to fluid retention. Excessive fluid retention causes edema around the eyes and legs.
Patients usually notice swelling of the legs when they go to bed or at night. Swelling around the eyes is first noticed in the morning because of the gravitational effects.
How to manage edema?
Edema is swelling of the feet and other areas of the body. It is due to the water-retaining properties of insulin.
- Avoid water retention by reducing salt in the diet.
- Avoid prolonged sitting or standing
- Do not take medications that can exacerbate the swelling. Medications that may cause swelling include:
- Calcium channel blockers like amlodipine (Norvasc)
- Thiazolidenediones (pioglitazone)
- Oral contraceptive pills
- NSAIDs ( Non-steroidal anti-inflammatory drugs)
- Use medications that may reduce body swelling, such as SGLT 2 inhibitors (empagliflozin, dapagliflozin, and ertugliflozin)
- Use antihypertensive medications (if needed) that do not cause fluid retention, such as ACE inhibitors or ARBs, or in combination with diuretics.
4. Injection site reactions:
Injection site reactions may include pain, redness, swelling, or induration. Pain is the most common injection 💉 site reaction.
Patients may develop an infection at the site of insulin injection, resulting in cellulitis. If left untreated, an abscess may develop in the area, which may be very difficult to treat and require repeated surgical debridements.
Prolonged administration of insulin into one area may result in lipohypertrophy. Patients may complain of lumpy swellings over the abdomen that may become painful. Pain is especially felt after insulin injections.
How to avoid injection site reactions?
Pain is the most common injection site reaction. Pain can be reduced by using the smallest gauge needle. The injection technique may need to be corrected. Patients should be asked to rotate the site of injections.
Skin infection and cellulitis are not common however, in patients with poor body hygiene, the risk may be very high. Ask patients to wipe the area with a spirit swab or wash it before injecting insulin in such cases.
Patients should be advised to change insulin needles at least after three days of use and more frequently in case of recurrent infections.
Furthermore, insulin should not be injected into the skin that is red, tender, indurated, or has an active infection.
Also, avoid injecting insulin close to the navel and groin areas, where the chances of infections are very high.
5. Retinopathy (Diabetic Eye Disease):
Diabetic eye disease or retinopathy is a common and one of the earliest microvascular complications of diabetes mellitus.
Rapid glucose changes, as may occur with insulin treatment, have been associated with the worsening of diabetic retinopathy. Patients may notice blurring or a change in vision after insulin initiation.
Most experts think that the worsening of eye disease is primarily due to rapid changes in blood glucose. With rapid fluctuations in plasma glucose, the retinal fibers are more likely to be damaged.
Like insulin, other diabetes treatments that cause rapid glucose changes, especially Semaglutide (Ozempic), have also been associated with the worsening of diabetic eye disease.
How to prevent the worsening of diabetic eye disease?
It is very difficult to prevent the ongoing damage to the eyes caused by diabetes. However, one can prevent rapid plasma glucose changes.
Insulin treatment should be initiated in low doses, and the dose should be titrated slowly until the blood glucose goals are achieved.
Patients may be advised to take adequate amounts of vitamin A and beta-carotene.
6. Neuropathy (Insulin Neuritis)
Diabetic neuropathy is the most common complication of diabetes mellitus. It may start as early as prediabetes and progress rapidly over time. It is more common in patients with depression and in men who have impotence or erectile dysfunction.
With insulin treatment, people may develop worsening symptoms of diabetic neuropathy. These symptoms may include numbness, tingling, burning, or paraesthesias. Some patients develop acute painful neuropathy, which is also referred to as insulin neuritis.
The exact mechanism of insulin neuritis is not known, however, it is thought to be caused by ischemia, hypoglycemia, neuronal damage, and neuronal regeneration [Ref].
How to manage and prevent insulin neuritis?
Insulin neuritis may partially be avoided by starting insulin in lower doses and gradually titrating the dose. It is especially a problem in patients who have preexisting neuropathy and those who develop hypoglycemia following insulin administration.
Insulin neuritis is reversible. It takes three to six months for patients to recover if the blood sugars are maintained in the normal range.
Treatment is usually difficult; however, supplementation with vitamin B12 and using analgesics like paracetamol and tramadol may be helpful.
Some patients may need to be started on specific medicines that are used to treat neuropathy. These medicines may include Gabapentin, Pregabalin, or duloxetine.
Patients must be advised to wear shoes that are protective and to inspect their feet daily for any ulcers or wounds. Nails must be properly cut to avoid ingrown toenails.
7. Hypokalemia:
Hypokalemia rarely develops in patients who are on high doses of insulin. It is particularly concerning in patients who are administered continuous intravenous insulin infusions.
Hypokalemia is, hence, most commonly reported while patients are treated for Diabetic Ketoacidosis and HHS (Hyperosmolar Hyperglycemic states).
How to manage hypokalemia while on Insulin infusion?
Potassium is added to intravenous fluids once the patient has adequate urine output and can eat via mouth.
Insulin infusion should be avoided in patients who have a baseline serum potassium of less than 3 mEq/L.
Potassium replacement is recommended, along with insulin for all patients who have a serum potassium of less than 5.3 mEq/L.
Oral potassium can be added in stable patients who are out of the acute hyperglycemic emergency (DKA and HHS).
In severe hypokalemia and those patients with cardiac arrhythmias associated with hypokalemia, potassium chloride should be given as a slow intravenous infusion via a central line with cardiac monitoring.
To Summarize Insulin Side effects:
Insulin is one of the safest diabetes medicines. However, side effects can occur. Some of the insulin side effects are very common and can be avoided.
Hypoglycemia is the most common side effect of insulin and can be prevented by initiating insulin in a low dose and titrating the dose slowly.
Other common insulin side effects may be prevented to some extent. These include weight gain, edema, injection site reactions, neuropathy, and retinopathy.
- Premium Ingredients: Our tea blend features high-quality Berberine, aromatic Oolong, and refreshing Mint, all organicall…
- Mint Flavored: Enjoy the cool, crisp taste of mint that perfectly complements the robust flavors of Berberine and Oolong…
- Unsweetened with Zero Calories: Crafted for those who appreciate the natural flavors of tea, our blend is completely uns…
- PRACTICAL DESIGN. The expansion zipper increases capacity by 40% and the triple-layer compartment of the diabetic bag pr…
- LONGER COOLING EFFECT. This insulin case has 2 latex-free ice packs and each weighing 180g, so it can keep cool for 8-10…
- OPTIMAL INSULATION. Made of Oxford fabric exterior + thickened pearl cotton + aluminum interior, the insulated medicatio…
- 3 COOLING METHODS FOR ULTIMATE FLEXIBILITY – Our insulin travel case TSA approved offers 3 distinct cooling methods to m…
- LARGE STORAGE & STAINLESS STEEL DESIGN – This medicine travel case can store 1-7 insulin pens, vials, or diabetic suppli…
- MULTIFUNCTIONAL COOLER WITH USB CHARGER – By switching the lid, you can transform this insulin cooler travel case USB-bu…
- LED screen temperature touch control screen; Portable; 0~8° fast cooling;Easy using. Charge the battery fully for 7 hour…
- Multiple charging modes :110V-240V adapter,USB cable,portable batteries,/car/home/battery can be used,suitable for trave…
- 1 year warranty and TSA Approved. QIRDLP insulin cooler travel case is for diabetics.Thank you for choosing our products…








