Insulin Degludec is available in the markets under the brand name Tresiba (Tresiba Flexpen). It is also available with other diabetes medications:
- Injection Ryzodeg is a combination of Degludec and Insulin Aspart
- Injection Xultophy is a combination of Degludec and Liraglutide.
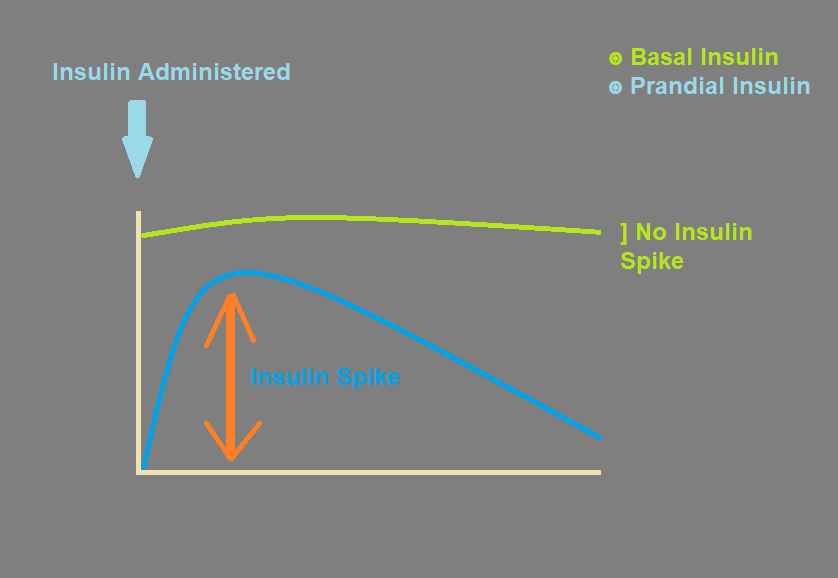
Degludec is one of the longest-acting insulins. It is usually added to the treatment regimen of diabetic patients as basal insulin. Basal insulin provides insulin coverage throughout the day.
Because of the absence of insulin peak, basal insulins are the least associated with hypoglycemia. Hypoglycemia is one of the main reasons that physicians prefer using basal insulins.
Other basal insulins currently available in the markets include:
- Insulin Glargine (Injection Lantus, Toujeo, or Basaglar)
- Insulin Levemir (Injection Detemir)
Intermediate-acting Insulins that are sometimes used as basal insulin include:
- NPH Insulin (Neutral Protamine Hagedorn)
- Insulin Aspart Protamine
- Insulin Lispro Protamin
| You may also like to read: |
Insulin Degludec Class, Pharmacology, and Peak Time:
Insulin Degludec is an ultra-long-acting Insulin [Ref] commonly classified as a basal Insulin. Like all other insulins, Insulin Degludec lowers blood glucose by promoting the synthesis of glycogen and fatty acids in the liver [Ref].
It also promotes protein and glycogen synthesis in the muscles and regulates lipoprotein metabolism in the adipose tissues.
Insulin Degludec promotes the cellular uptake of proteins and potassium by acting on the sodium-potassium-ATPase channels.
The onset of action and Peak Time of Insulin Degludec (Tresiba):
The onset of action of Insulin Degludec is about one hour after subcutaneous administration. It is regarded as peak-less insulin, however, the maximum levels of Insulin Degludec have been observed after 9 hours of its administration.
The action of Insulin Degludec lasts for more than 42 hours. Compared to Insulin Glargine and Insulin Levemir which have a half-life elimination of about 12 to 16 hours, the half-life elimination of IDeg (Insulin Degludec) is about 25 hours.
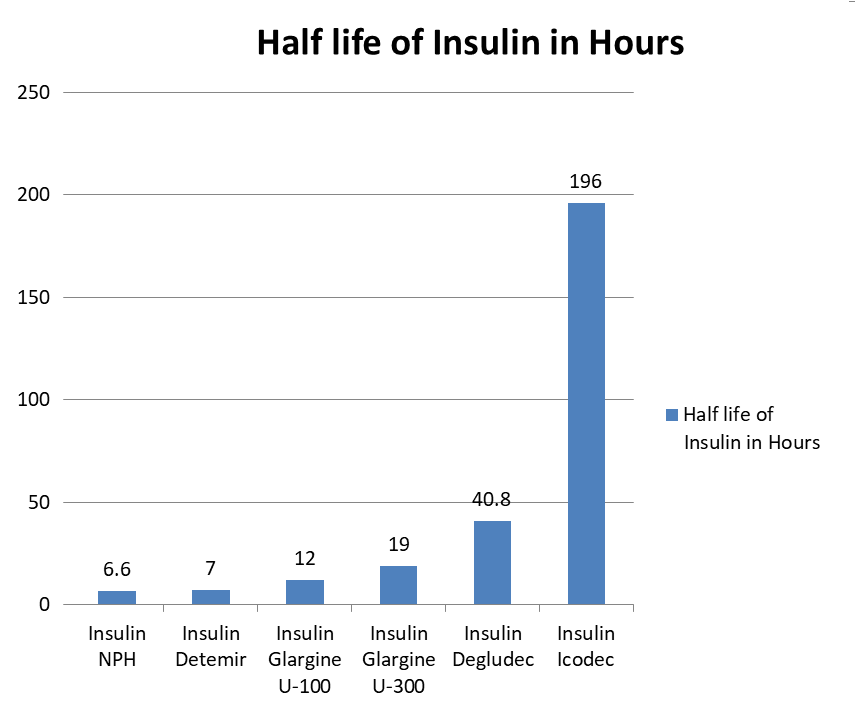
The steady state is reached within three days. The timings of insulin administration do not affect insulin levels. Therefore, unlike insulin Glargine and Levemir that is administered at a fixed time of the day, Insulin Degludec can be administered at any time of the day.
When compared to Insulin Glargine (IGlar), it has about four times more stable glucose-lowering effects.
| You may also like to read: |
Insulin Degludec Brand Name and Price:
Insulin Degludec is available by the brand name:
- Injection Tresiba
Tresiba Insulin is available in vial formulations and Flextouch Pens.
It is also available with Insulin Aspart as Insulin Ryzodeg (Penfilled/ Flextouch pens) and in combination with Liraglutide as Xultophy Injection.
Insulin | Brand | Price |
| Insulin Degludec | Injection Tresiba | 1 vial of 10 ml (100 units/ml):
3 ml Flextouch Pens (200 Units /ml):
|
| Insulin Degludec + Insulin Aspart | Injection Ryzodeg | Injection Ryzodeg is no more marketed in the United States. |
| Insulin Degludec + Injection Liraglutide | Injection Xultophy | Five 3 ml pens of 100 units/ml:
|
Insulin Degludec Dosage and Dosage Chart:
Insulin Degludec is basal insulin. Because of the once-daily administration, it is one of the preferred insulin. It is also preferred by people who have a busy schedule, are scared of needles, and are at risk of hypoglycemia.
Treatment with insulin is recommended in patients who have uncontrolled blood sugars despite medications or the blood sugars are greater than 300 mg/dl and the glycated hemoglobin exceeds 10%.
How to initiate insulin treatment using Insulin Degludec?
To avoid hypoglycemia, it is recommended to initiate insulin in low doses. The usual recommended doses are either weight-based or fixed insulin units:
- Start Insulin Degludec (Tresiba) as 8 or 10 units once daily at bedtime or any time of the day.
- Alternatively, Insulin Degludec can be initiated as 0.1 to 0.2 units/kg/day. However, if the blood sugars are very high such as in those patients with glycated hemoglobin exceeding 8%, the initial dose can be increased to 0.2 to 0.3 units/kg/day.
When given with other short-acting insulins (Regular Insulin) or rapid-acting insulins (Aspart, Lispro, or Glulisine), or Ultra-rapid acting insulin (FiASP, Insulin Lyumjev or Lispro AABC, or Insulin Afrezza – inhaled insulin), 40 to 50% of the total daily dose of insulin is administered as basal insulin.
For example, a person requires 40 units of insulin daily. 20 units will be administered as basal insulin (Insulin Tresiba) and the remaining 20 units of insulin will be divided into two or three doses prior to each meal.
| You may also like to read: |
How to titrate Insulin Degludec dose?
Dose titration is important before you assume that Insulin Tresiba is not effective. Generally, dosage titration is done by increasing the dose of insulin by 2 to 4 units at weekly or twice weekly intervals.
Alternatively, the dose may be titrated based on the body weight especially when the dose of insulin required is too less or too high. It is recommended to increase the Insulin Tresiba dose by 10% to 15% at weekly or twice weekly intervals.
The dose is titrated up until you reach a dose of at least 1 unit per kg. For example, an 80 kgs weighted person can titrate the dose to the maximum of 80 units daily.
If the blood sugars are still not controlled, it is better to consult your healthcare provider. At this point, your physician might advise any of the following:
- switching to another type of insulin regimen (basal-bolus or premixed insulin),
- adding another oral medicine, or
- increasing the dose further.
It should be noted that before adding other medicines and increasing the dose, always cross-check the following factors:
- your insulin administering technique,
- whether or not the insulin may be ineffective due to very high or low temperatures, and
- if you have recently been prescribed medicines that might increase your blood glucose such as corticosteroids, and
- if you have got an infection like UTI (urinary tract infection) or chest infection.
How to adjust Insulin Degludec dose if a person develops hypoglycemia?
A single episode of hypoglycemia that is not serious enough might not need any dosage adjustment. This is true especially if you missed your dose or had a temporary gastrointestinal upset.
However, if you experience frequent hypoglycemia, it is recommended to adjust your Insulin Degludec dose. It is usually recommended to reduce the insulin dose by 10 to 20% of the usual dose.
For example, if a person is injecting 40 units of Degludec daily, he should lower the dose by 20% of the 40 units (40 x 20% = 8). He should reduce the dose by 8 units. His total daily dose should be 32 units per day.
How to adjust the dose if a person is also advised premeal insulin along with Insulin Degludec?
If a person is switched to a basal-bolus insulin regimen i.e. adding premeal insulin to the basal insulin, the total daily dose should be reduced by 10% if the glycated hemoglobin is less than 8%.
For example, if a person is using 60 units of Insulin Tresiba daily, his total insulin dose will be reduced by 10% (60 x 10% is 6).
So, his total insulin dose will be 54 units per day. Out of 54 units, 40 – 50% will be administered as Injection Tresiba. About 24 units will be prescribed as Injection Tresiba and 10 units of short-acting or rapid-acting insulin will be prescribed before each meal.
If the glycated hemoglobin is more than 8%, the total daily dose should be divided into basal and bolus insulin.
For example, if a person on 60 units of Insulin Tresiba with glycated hemoglobin of 9% is being switched to basal-bolus insulin, the total daily dose will remain the same i.e. 60 units.
40 to 50% of the total daily dose will be administered as basal insulin (Degludec) while the remaining dose will be divided into two or three and administered before each meal.
In this case, the person will be advised 30 units of Insulin Tresiba once daily and 10 units of short-acting or rapid-acting insulin before each meal (thrice daily).
How to adjust the Insulin Degludec dose before surgery?
Because patients are kept NPO (nothing per oral) and the stress of surgery can alter the blood glucose levels, it is recommended to adjust the insulin dose before surgery.
A person who is using less than 10 to 12 units of Insulin Tresiba daily can totally miss the dose. However, it is generally recommended to reduce the last dose of Insulin Tresiba by 20 to 40%.
If a person is on 60 units of Insulin daily, the recommended dose one day before surgery will be 36 to 48 units depending on the blood glucose.
How to adjust the dose when switching from another basal insulin?
When switching from another basal insulin such as Insulin Glargine (Injection Lantus, Toujeo, or Basaglar) or Insulin Detemir (Injection Levemir), it is recommended to reduce the dose of Degludec by 20% of the total dose.
For example, if a person is injection Injection Lantus 60 units daily, the dose of Degludec should be reduced by 20%. Thus, the dose of Degludec should be 48 units per day.
However, the same dose should be administered if the person has uncontrolled blood glucose or the glycated hemoglobin is 8% or more.
What to do if you miss your dose?
Insulin Degludec can be administered at any time of the day. If you were used to injecting Insulin Tresiba at night and you missed the dose, you can inject it the other day.
If you were injecting Injection Tresiba in the morning and you missed the dose, you can inject it in the evening.
It is important to give a gap of at least 8 hours between two doses.
Insulin Degludec Dose in Children:
The dose of Insulin Degludec in children is different in insulin naive vs insulin-experienced ones.
The usual total daily dose of insulin is 0.2 to 0.4 units/kg. About 60% to 75% of the total dose is administered as basal insulin while the rest is given as prandial insulin before each meal.
Children who require less than 5 units of insulin per day should not be started on Degludec Insulin.
Children who are already using another basal insulin should be advised of Degludec in a dose equal to 80% of the total basal insulin.
For example, a child on 20 units of insulin glargine should be advised 16 units of Degludec.
| You may also like to read: |
Insulin Degludec (Tresiba) Side effects:
Hypoglycemia:
Insulin Degludec is a relatively safe insulin because it does not have a peak. Because of the absence of a peak, it is less likely to be associated with hypoglycemia compared to other insulins.
Like all other insulin, the most common side effect of Degludec is hypoglycemia. Hypoglycemia can occur with any insulin if the dose exceeds the patient’s requirements.
In one study, the risk of daytime hypoglycemia with Insulin Degludec and Insulin Glargine was comparable. However, the risk of nocturnal hypoglycemia (hypoglycemia at night) was significantly lower with Degludec (Tresiba) compared to Insulin Glargine [Ref].
The risk of hypoglycemia is also more common in patients with renal and hepatic impairment.
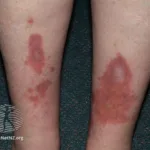
Injection site reactions:
Because Degludec is administered as a subcutaneous injection, it can cause local injection site reactions.
Lipohypertrophy:
Lipohypertrophy is the accumulation of fats at the site of insulin injection. It is more common in patients who inject insulin at the same site.
To avoid lipohypertrophy with insulin Tresiba, it is advisable to rotate the sites of injection. The recommended site of injection is the anterior abdominal wall slightly away from the umbilicus.
Hypokalemia:
Hypokalemia is another side effect common to all insulins. Insulin causes the shift of potassium inside the cells. Hypokalemia can result in serious cardiac arrhythmias.
Weight gain:
Weight gain is a side effect of all insulins. The weight gain associated with Degludec has been documented as 1 to 3 kgs and is comparable to Insulin Glargine.
| You may also like to read: |
Other Formulations of Insulin Degludec:
- Injection Xultophy (Insulin Degludec/liraglutide)
- Injection Ryzodeg (Insulin Aspart and Degludec)
Injection Xultophy (Insulin Degludec/liraglutide):
Injection Xultophy is a combination of Injection Tresiba and Injection Liraglutide. Degludec is ultra-long-acting insulin while Liraglutide is a GLP-1 analog.
The combination of Degludec and Liraglutide not only improves the glycemic effects but also reduces the chances of weight gain associated with Insulin Degludec alone.
Since it is a combination of two injectable medications, it also reduces the number of injection pricks by half and may improve compliance with treatment.
Injection Ryzodeg (Degludec and Aspart):
Insulin Ryzodeg is a combination of rapid-acting and ultra-long-acting insulin. It has been recently discontinued in the US.
Insulin Ryzodeg is however a very attractive option for people who take one major meal per day. This is especially true for Muslims during Ramadan when most people take one major meal at Iftar.
Insulin Aspart provides meal coverage while Degludec provides basal insulin coverage.
| You may also like to read: |