The hunger hormone in the stomach is called Ghrelin. It is a peptide hormone that is produced mainly by the stomach in the fasting state.
It is mostly excreted during periods of starvation and anorexia when a person is in a negative energy balance.
This stomach hormone in the stomach is associated with weight gain. Its levels drop in fed states and when the blood glucose is high.
Apart from appetite stimulant effects and regulating food and energy intake, it has been found to have some role in memory and growth as well.
Go Organic! Try Our Premium Organic Brands
What is Ghrelin? The Hunger Hormone in the stomach:
Ghrelin is a 28-amino acid peptide. It acts on growth hormone receptors and stimulates the secretion of growth hormone.
Ghrelin can be administered intramuscularly or centrally to stimulate the secretion of growth hormone and increase food intake.
Because it is released in states of hunger and fasting, it is associated with weight gain.
Where is the Ghrelin hormone distributed in the human body?
Ghrelin was first discovered in 1999 after it was found that tissue from the stomach of rats activated the growth hormone secretagogue (GHS-R).
Since then, it has been established that the stomach is the best source of ghrelin. Up to 99% of the total Ghrelin in our body is found in the stomach.
It is also found in the pancreas, duodenum, pituitary, kidney, and placenta. A small amount of Ghrelin is also found in the hypothalamus arcuate nucleus.
Ghrelin is found in the stomach fundus, where it is most abundant. It is produced in oxyntic cells by distinct endocrine cells called P/D1 cells.
Because most of it is released from the stomach, it is also termed “the hunger hormone of the stomach”.
Where are Ghrelin receptors located?
Ghrelin (growth hormone secretagogue receiver [GHS-R]), is a member of a G protein-coupled receptive (GPCR) subfamily, which also includes neurotensin, motilin, and neuromedin U.
GHS-R1a and GHS-R1b are two forms of this receptor. They both result from alternative mRNA sequencing from one gene.
GHS-R1a expression is found in the peripheral and central nervous systems. GHS-R1a is expressed in both the central nervous system and peripheral tissues.
It is found most prominently in the hypothalamus. However, it can also be found in the parasympathetic preganglionic neuronal neurons and the dorsal motor nucleus.
Ghrelin receptors are expressed in the Central and Peripheral Nervous systems.
GHS-R1a is co-expressed in hypothalamic nuclei with neuropeptides Y (NPY), and agouti-related peptides (AgRP), which regulate food consumption and satiation [Ref].
GHS-R1a can be found in peripheral tissues such as the anterior pituitary and islet cells of the pancreas, thyroid, adrenal, and glands.
GHS-R1a can also be found on autonomic and enteric neurons, but not on smooth muscle. GHS-R1b, a shorter form of the receptor, is distributed more widely than GHS-1a. It does not interact with the G protein complex so its biological actions are unknown.
How is the hunger hormone in the stomach secreted?
Ghrelin levels in the blood rise during fasting, and spikes occur just before meals. This stomach hormone is under sympathetic and vagal nervous system control.
One can modulate the effects of Ghrelin which may help in meal preparation. After eating, Ghrelin levels drop.
The suppressive effects of food seem to be nutrient-specific. Carbohydrates have the most effect, followed closely by protein and lipids.
Postprandial suppression is not related to intraluminal nutrient exposure or meal effects on gastric distention but occurs via non-vagal neural signals.
Ghrelin expression was detected in some types of cancers, including most gastric carcinoids as well as some pancreatic and intestinal neuroendocrine tumors.
Ghrelin has been shown to promote growth in vitro. It is also suggested that ghrelin might be a potentiator of cancer growth. This could be one reason why obese people are at risk of developing cancer.
Paradoxically, low baseline levels of ghrelin have been linked to gastric cancers, esophagogastric Junction, and other cancers.
This could be because serum ghrelin levels decline in chronic inflammation and atrophy.
Fasting plasma levels of ghrelin are between 550 and 650 pg/mL in lean people. In obesity, circulating ghrelin levels fall to 200 to 350 pg/mL in states of positive energy balance and between the two.
A decrease in plasma ghrelin has been linked to gastritis. This could be caused by Helicobacter Pylori infection. Serum ghrelin may be a useful indicator of gastric atrophy.
Fasting, anorexia, and cachexia all have high levels of ghrelin. The fasting levels of ghrelin are over 1000 pg/mL. Weight loss is associated with an increase in circulating ghrelin.
Numerous reports have shown that the gut microbiome influences ghrelin production by releasing bacterial metabolites, including lipopolysaccharides and hydrogen sulfide. These relationships are complicated and poorly understood.
What are the effects of Ghrelin?
Ghrelin can be intravenously administered to stimulate growth hormone secretion. It causes mild elevations in cortisol (ACTH), cortisol, and prolactin.
Ghrelin and growth hormone-releasing hormone (GHRH), together, can increase growth hormone levels.
The effects of ghrelin on growth hormone release may be mediated by neural afferent vagal pathways. This may include stimulation of GHRH.
The effects of hunger hormones in the stomach on energy balance and food intake:
Ghrelin can stimulate appetite and induce a positive energy balance, which can result in weight gain.
Ghrelin plays a role in mealtime hunger and meal initiation. Ghrelin was the first hormone that can increase feeding rate when administered peripherally.
Ghrelin is the only known orexigenic hormone transmitter that stimulates feeding when administered peripherally.
Ghrelin is believed to signal the body to initiate feeding. Ghrelin is a hormone that increases the quantity but not the size of meals. Ghrelin is responsible for regulating short-term eating habits and regulating body weight over time.
Ghrelin levels that are elevated during fasting are associated with activation in reward centers in the hypothalamus, amygdala, and prefrontal cortex. This indicates that food intake is more complex than hunger and satiety.

The effect of hunger hormone in the stomach on Adiposity:
Normal postprandial suppression is impaired in obese subjects. Ghrelin can also induce adiposity, which is maintained as long as ghrelin levels remain elevated.
It counteracts energy storage decreases and prevents starvation. Ghrelin was the first hormone that signaled starvation and is believed to play a role in long-term regulation.
Ghrelin effect on Neuropeptide Y:
Ghrelin is a neurotransmitter that activates AgRP-producing and NPY neurons in the hypothalamus arcuate nucleus. This area of the brain is important in the regulation of food intake.
The ghrelin hormone-secretagogue receptor GHS-1a is also expressed in the pituitary, hypothalamus, and substantia nigra.
Ghrelin is known to have a profound effect on the brain’s higher functions such as memory, sleep, and reward-seeking behavior.
The effect of Ghrelin on Gastric motility:
Ghrelin, which is similar to motilin stimulates gastric contractions and increases stomach emptying.
It also increases phase III-like contractile activities of the stomach, duodenum, and duodenum. These effects are caused by the vagal cholinergic pathway.
Ghrelin was shown to depolarize Cajal interstitial cells, which regulate the gastrointestinal pacemaker function in murine models.
Ghrelin’s prokinetic effects are stronger than those of other gastrointestinal proteins, such as Cholecystokinin which acts as hunger signals.
Ghrelin effect on Immune function:
Evidence suggests that ghrelin might have anti-inflammatory properties.
One study found that ghrelin receptors on human T cells, and monocytes, inhibited proinflammatory and anorectic chemicals, such as interleukin-1 beta and tumor necrosis factor-alpha [Ref].
Ghrelin effect on Bone formation and body weight:
Ghrelin could also be thought to affect bone metabolism. Growth hormone has been shown to increase bone formation.
GHS-R1a has been identified in osteoblasts, which indicates that ghrelin can stimulate osteoblast cell proliferation as well as differentiation.
Ghrelin has been shown to increase bone mineral density in normal and growth hormone-deficient animals.
Serum ghrelin levels appear to be independent predictors of BMD in healthy adolescent girls as well as those suffering from anorexia, which is a disorder that causes higher than normal ghrelin secretion.
As we age, growth hormone secretion decreases. This may lead to sarcopenia in older adults. Ghrelin-agonists have been shown in studies to increase pulsatile growth hormone secretion.
Axis of growth hormone: Short stature has been linked to GHS-R defects. The GHS-R locus seems to be a source of genetic variation for height.
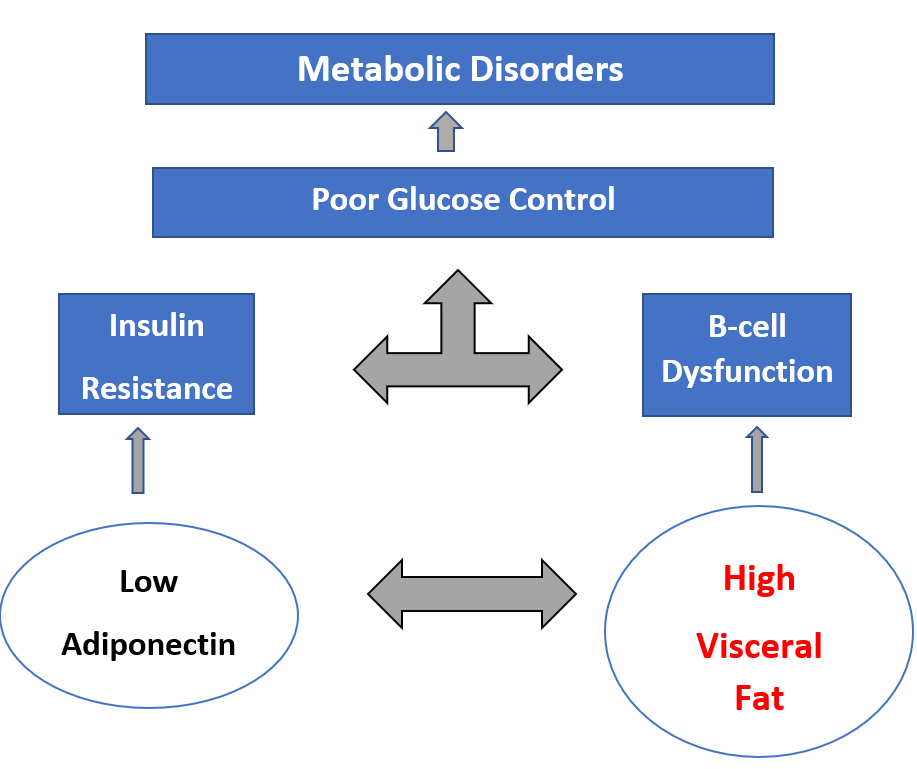
The function of the Islet: GHS-R1a expression is predominant in pancreatic islets. This indicates that insulin and glucagon secretion is inhibited indirectly by ghrelin. Ghrelin, consistent with its receptor expression inhibits glucose-stimulated insulin production.
The role of hunger hormone in the stomach in various diseases:
Ghrelin in Obesity:
- Ghrelin levels in obese people are low and are associated with insulin resistance and weight gain. Ghrelin levels that are higher in obese individuals are linked to low-calorie diets, exercise, and cachexia.
- Obese individuals who binge eat are more likely to have low levels of ghrelin, which suggests that ghrelin may be a result rather than a cause.
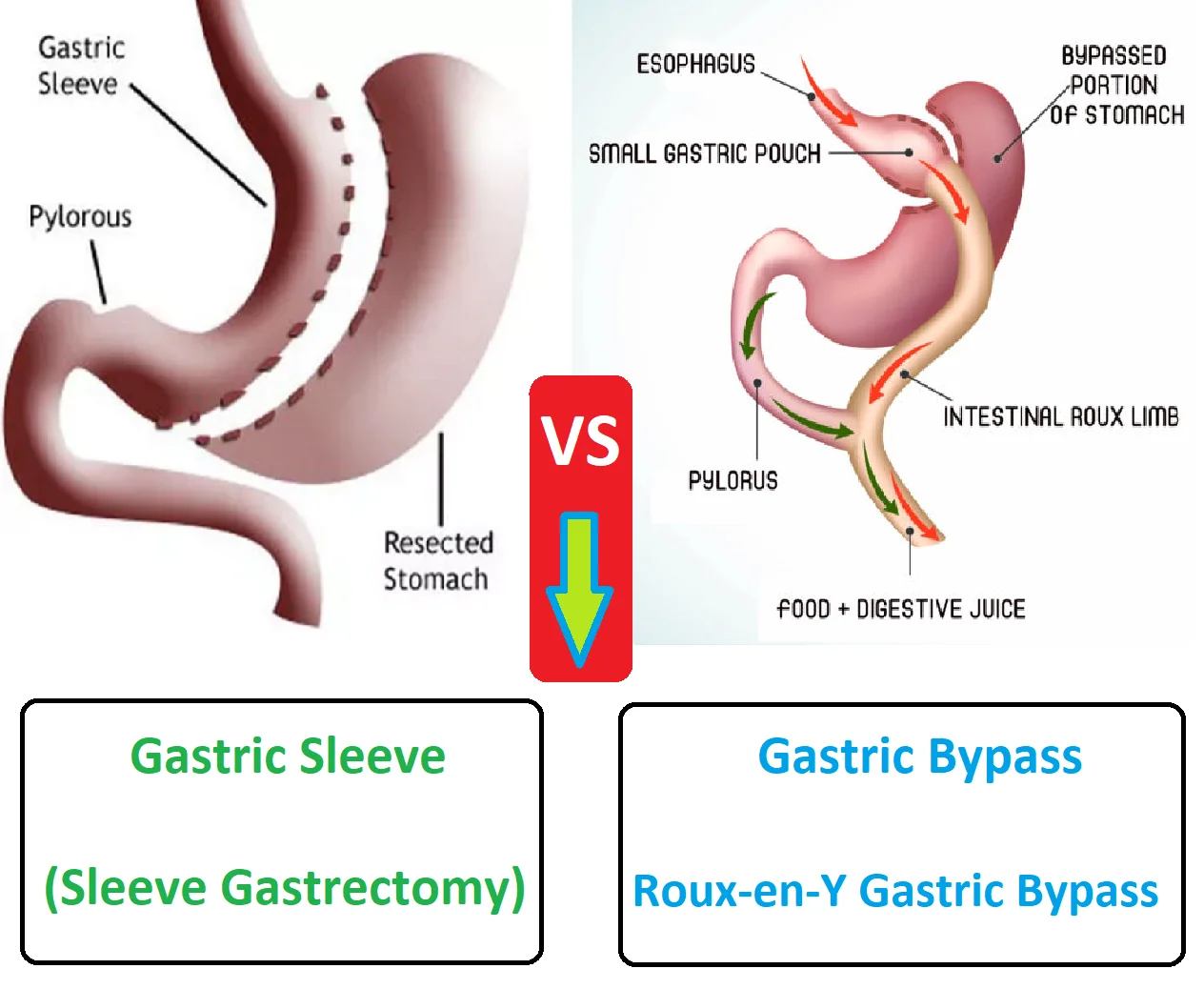
Ghrelin in Gastric Bypass surgery:
- Some bariatric surgeries can lower the levels of ghrelin. Patients with obesity are often treated by gastric bypass surgery. This is a common and effective treatment.
- The operation creates a small pouch in the stomach that is drained by the intestinal limb. In this way, most of the stomach, duodenum, and jejunum are bypassed.
- Patients undergoing gastric bypass have different plasma ghrelin profiles.
- Furthermore, abnormal ghrelin levels can result in abnormal GI and neuroendocrine functions [Ref].
- They do not have the same premeal plasma ghrelin increase as normal people, and their cumulative ghrelin secretion levels are much lower.
- Sleeve gastrectomy also reduces ghrelin levels. The lack of ghrelin responses may be one reason for the decreased effectiveness and lower energy balance after surgery.
- Ghrelin secretion may be reduced after gastric bypass surgery, which could improve glucose tolerance.
- Ghrelin, under normal circumstances, stimulates the secretion of insulin counter-regulatory hormones and suppresses adiponectin production. It also inhibits insulin secretion.
- Ghrelin may have a negative impact on insulin secretion.
Ghrelin’s role in patients with Prader-Willi syndrome:
- Prader-Willi Syndrome is a condition that causes severe hyperphagia, growth hormonal deficiency, and hypogonadism.
- It also has dysmorphic features and cognitive impairment. Functional loss of several genes that are paternally expressed in an imprinted region on chromosome 15, is the genetic basis.
- Low ghrelin levels are often associated with obesity. However, Prader-Willi syndrome is associated with high circulating levels of ghrelin that do not decrease after eating.
- This syndrome has a similar level of ghrelin to the levels that stimulate appetite and increase food intake for people who receive exogenous Ghrelin.
- It is unknown if the persistently high levels of ghrelin are the cause of the low growth hormone secretion. This could be due to desensitization.
Potential Clinical Uses of Ghrelin:
Ghrelin’s short half-life makes it difficult to use therapeutically. However, there are many longer-acting alternatives. Ghrelin is a mimetic drug.
Macimorelin is one of the longer-acting alternative drugs that has been approved by the US Food and Drug Administration (FDA) for diagnosing growth hormone deficiency [Ref].
It is safe, effective, and has comparable efficacy to the Arginine GHRH test.
Ghrelin is an important signal that stimulates food intake and promotes positive energy balance and weight gain.
Therefore, it is reasonable that ghrelin antagonists will block these orexigenic signals and may prove to be effective anti-obesity treatments.
Pharmaceutical companies are focusing their efforts on developing ghrelin antagonists.
It will be particularly interesting to see if interventions that lower the circulating levels of ghrelin or ghrelin receptor analogs can effectively treat hyperphagia/obesity of Prader-Willi Syndrome.

Ghrelin agonists could also be used to treat anorexia. It may have a role in treating cachexia based on its effects on food intake and ability to inhibit the production of anorectic proinflammatory chemicals cytokines.
For the treatment of unexpected weight loss in pets, capromorelin, an oral ghrelin-agonist, has been approved by veterinary authorities.
Advanced clinical trials are currently evaluating ghrelin-agonists for the treatment of gastrointestinal motility disorders including gastroparesis.
One macrocyclic ghrelin mimetic failed to meet clinical endpoints during late-stage clinical trials. However, smaller molecule ghrelin antagonists might be more effective.
Ghrelin mimetics could be used to treat frailty among older adults. The anti-aging effects of caloric restriction may be due to the increased circulating levels of ghrelin associated with fasting. It is possible that ghrelin-mimetics could have other effects than reducing frailty.
Ghrelin was suggested to prevent neurodegenerative conditions like Alzheimer’s disease, due to its ability to stop beta-amyloid accumulation in animal models.

Summary:
Ghrelin is most abundant in the stomach. It makes up over 90% of the body’s total. It is found most often in the stomach fundus, where it is made in distinct endocrine cells called P/D1 cells.
Ghrelin (a 28-amino acid peptide) is the natural ligand of the growth hormone secretagogue regulator (GHS-R). GHS-R belongs to a subfamily of G protein-coupled receptors (GPCR), which also includes neurotensin, motilin, and neuromedin.
Ghrelin levels in the blood rise during fasting and then surge just before meals. After eating, its levels drop. Food appears to have a specific effect on its plasma levels.
The most suppressive effects are seen in carbohydrates, followed by protein, and lipids.
Ghrelin can stimulate appetite and induce a positive energy balance which may lead to weight gain. It plays a key role in mealtime hunger management and meal initiation.
There is evidence that it also plays an important role in the neurohormonal regulation of energy and food intake.
Go Organic! Try Our Premium Organic Brands