SGLT2 inhibitors are a novel class of medicines. In comparison to Sulfonylureas, and other drugs commonly used to treat diabetes, SGLT2 Inhibitors have the advantage of improving cardiovascular and renal outcomes as well.
SGLT2 Inhibitors include:
- Canagliflozin (Invokana),
- Empagliflozin (Jardiance),
- Dapagliflozin (Forxiga or Farxiga), and
- Ertugliflozin (Steglatro).
These drugs act by inhibiting the sodium and glucose transporter 2 channels present in the renal tubules resulting in glucose excretion via the kidneys.
SGLT2 inhibitor drugs, thus, are used in the treatment of patients with Diabetes mellitus type 2.
Since these drugs also cause osmotic diuresis, they are also effective in reducing blood pressure and relieving symptoms of fluid overload such as heart failure.
These drugs also halt the progression of diabetic nephropathy and may cause a modest degree of weight loss.
A comparison of the common SGLT2 inhibitors and the results of some of the important clinical trials are discussed here.
SGLT2 Inhibitors Comparison: Effect on Blood Glucose and A1C:
SGLT2 inhibitors have a weak effect on glucose-lowering agents. Their mean A1C reductions are between 0.4 and 1.1 percent, depending on the baseline level of hyperglycemia. They can be used alone or in combination with other therapies.
Meta-analyses of clinical trials comparing SGLT2 inhibitions with placebo and active comparators (metformin, sulfonylurea, dipeptidyl peptidase-4 [DPP-4] inhibitors, insulin) showed that SGLT2 antagonists reduced A1C by about 0.5 to 0.7 percentage points (mean difference versus active comparator -0.06 percent to -0.13%).
SGLT2 Inhibitors Comparison in Clinical Trials:
Important clinical trials which demonstrated the glycemic efficacy of SGLT2 Inhibitors are compared one by one.
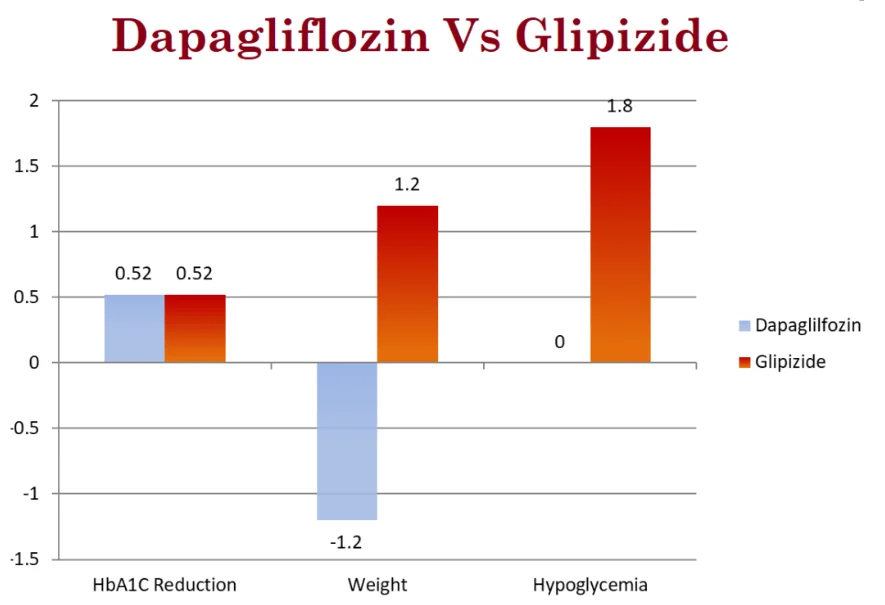
Dapagliflozin Vs Glipizide [Ref]:
In a double-blind, 52-week-long trial, 814 patients suffering from type 2 diabetes who had uncontrolled diabetes with metformin (mean average A1C 7.7%) were randomly assigned to either dapagliflozin or Glipizide.
- Both dapagliflozin and Glipizide reduced A1C by -0.52 percentage points.
- Dapagliflozin resulted in a mean weight loss of -1.2 kg while +1.2 kg weight gain was noted with glipizide.
- No episodes of severe hypoglycemia were observed in the Dapagliflozin group compared to glipizide (0 versus 0.7% with glipizide).
Dapagliflozin Vs Placebo in patients receiving high doses of Insulin [Ref]:
In another study, 808 patients suffering from type 2 diabetes mellitus with poorly controlled diabetes despite using insulin were randomly divided into two groups.
One group of patients received dapagliflozin in different doses (2.5, 5, or 10 mg once daily) and the other group was given a placebo medicine.
HbA1C dropped by 0.79 to 0.96 percentage points with dapagliflozin, compared to 0.39 percent with placebo (mean difference 0.40 to 0.57 percent in the 2.5-10 mg groups).
Daily insulin dose was decreased by 0.63 to 1.95 units when dapagliflozin was used and increased by 5.65 units when using a placebo.
Dapagliflozin use was associated with a weight reduction of -0.92 to 1.61 kg compared with +0.43kg weight gain with a placebo.
In the dapagliflozin-treated group, hypoglycemic episodes were more frequent (56.6% versus 51.8%) but were not statistically significant.

Canagliflozin Vs Sitagliptin [Ref]:
Canagliflozin is considered the most effective SGLT2 inhibitor. It is available under the brand name, Invokana. Sitagliptin is a DPP-IV inhibitor that is one of the most commonly used anti-diabetic drugs nowadays. It is available under the brand name, Januvia.
In a double-blind, 52-week-long trial, 755 patients suffering from type 2 diabetes who were poorly controlled while using metformin plus a sulfonylurea (mean baseline A1C 8.1%) were randomly divided into two groups:
- Sitagliptin (100mg daily) or
- Canagliflozin (300 mg daily).
A1C reduction was greater in the Canagliflozin (Invokana) group compared to Sitagliptin (least-squares change of -1.03 percent and -0.66 percent, respectively).
Canagliflozin decreased weight (-2.5 percent versus 0.3%) and systolic pressure (-5.1, versus 0.99 mmHg), respectively, to a greater extent compared to Sitagliptin.
The incidence of adverse events for both drugs was nearly the same, but genital fungal infections were six times more commonly observed with Canagliflozin compared to Sitagliptin.
This study’s overall results should be considered cautiously, as nearly 40 percent of subjects didn’t complete the entire year-long study.

Canagliflozin Vs Glimepiride [Ref]:
Canagliflozin and Glimepiride are both potent antidiabetic medications. Glimepiride is one of the most commonly used sulfonylureas, available by the brand name of Amaryl.
In a double-blind, 52-week-long trial, 1452 patients suffering from type 2 diabetes that was not controlled with metformin (mean average A1C 7.8%) were randomly assigned to either glimepiride (titrated according to blood glucose, median dosage 5.6 mg daily or canagliflozin 100 or 300 mg daily).
The average reduction in A1C was similar between the lower-dose and higher-dose glimepiride groups (-0.81 percentage points and -0.82 percentage points, respectively), and better by 0.1 percentage points in high-dose canagliflozin (-0.93 percentage point).
Patients with an A1C of 7% or below 6% were equally likely to be in the same group (approximately 56 percent and 31%, respectively).
Canagliflozin had a weight reduction of -4.2 to -4.4 kg, compared to +0.8 kg with Glimepiride.
However, it was associated with less severe hypoglycemia (1 as compared to 3%) and more frequent genital yeast infections in women (11 to 14 percent versus 2% with Glimepiride).

Canagliflozin was equally effective in terms of A1C reduction but much safer as it was associated with significantly lower chances of hypoglycemia.
In addition, it was associated with significant weight loss compared to the weight gain associated with glimepiride.
Empagliflozin Vs Placebo [Ref]:
Empagliflozin is another SGLT2 inhibitor that is very potent and has been proven to favorably affect the outcome in cardiovascular patients. It is available under the brand name, Jardiance.
In a 52-week study, type 2 diabetes patients who were not adequately controlled with metformin and multidose insulin (mean A1C 8.3%) were randomly assigned to either empagliflozin (10 mg or 25 mg once daily) [19].
Empagliflozin had a greater reduction in A1C (-1.18, 1.21, and -0.81 respectively for empagliflozin 10, 25 mg, and placebo).
Compared with placebo, empagliflozin decreased insulin doses by 9-11 units per day and weight loss by 2.4kg.

Ertugliflozin Vs Glimepiride [Ref]:
Ertugliflozin is a very potent SGLT2 inhibitor. It is probably more potent than Jardiance but less potent than Canagliflozin.
However, because its cardiovascular and renal benefits are only modest. It is available under the brand name, Steglatro.
In a 52-week double-blind study, 1326 patients with type-2 diabetes not controlled with metformin (mean average A1C 7.8%) were randomly assigned to either ertugliflozin (15 mg or 5 mg daily) or glimepiride (3 mg daily, titrated according to blood glucose).
The average A1C reduction with ertugliflozin 15mg daily was not statistically significant compared to glimepiride (-0.6% and -0.7%, respectively).
Ertugliflozin had a lower weight than glimepiride (-3.4kg compared to +0.9kg with glimepiride) and was associated with less severe hypoglycemia (0.2% compared to 2.3%), but more frequent genital yeast infections in women (10 versus 1.4% with glimepiride).

Comparing Cardiovascular effects of SGLT2 Inhibitors Drugs:
Atherosclerotic cardiomyopathy (CVD):
Empagliflozin (Jardiance) and Canagliflozin (Invokana):
- Patients with type 2 diabetes or overt CVD have had their mortality and atherosclerotic cardiovascular morbidity decreased by using them.
Dapagliflozin (Farxiga):
- Dapagliflozin did not reduce atherosclerotic cardio morbidity or mortality in one trial. However, it improved the cardiovascular parameters and outcomes in the subanalysis of the primary trial [Ref].
Ertugliflozin (Steglatro):
- Ertugliflozin did not demonstrate superior benefits in the composite outcome of nonfatal stroke, cardiac death, and nonfatal myocardial injury [Ref].
Comparing the efficacy of SGLT2 Inhibitors drugs in patients with Heart failure:
All SGLT2 inhibitors showed positive effects in patients with type 2 diabetes and heart disease.
A meta-analysis of three major CVD outcomes trials (empagliflozin/canagliflozin, and dapagliflozin) showed that SGLT2 inhibitors compared to placebo decreased the risk of major adverse cardiac events (86.9 versus 96.6 events per 1000 patients-years; hazard ratio [HR] 0.89; 95% CI 0.83-0.96); and a composite outcome (CV death or hospitalization due to heart failure) (48.2 versus 65.6, HR 0.77, HR 0.77, 95% CI 0.71-0.84, 95% 0.91-0.84) [Ref 1 and 2]
Patients with atherosclerotic CVD were only shown to have a clinical benefit from SGLT2 inhibitors. There was no benefit for patients with multiple CVD risk factors.
Contrary to the major adverse cardiovascular events findings, there was a decrease in hospitalizations for heart failure due to SGLT2 inhibitions.
It is not yet known if empagliflozin or canagliflozin will cause similar CVD symptoms in type 2 diabetics who don’t have overt cardiovascular disease.
Recent studies have proven the beneficial effects of Jardiance and Farxiga in patients with HFpEF (heart failure with preserved ejection fraction).
The efficacy of Empagliflozin (Jardiance) in patients with heart failure [Ref]:
A trial to assess cardiovascular morbidity in patients with type-2 diabetes and established CVD involved 7028 patients (mean A1C about 8%) and CVD.
They were randomly assigned to empagliflozin (10, 25 mg) or a placebo daily. Most patients were on metformin and antihypertensives.
The majority also took lipid-lowering drugs (equally distributed in both groups) to manage blood glucose, blood pressure, and cholesterol. About 48 percent of patients in each category were using insulin.
After three years, the primary outcome, a composite of death due to cardiovascular causes, nonfatal cardiac infarction, or stroke, occurred in fewer patients who were given empagliflozin rather than placebo (10.5 percent versus 12.1%).
These findings were driven by a significantly lower risk of death due to cardiovascular causes (3.7 percent versus 5.9% with placebo; HR 0.62 and 95% CI 0.49–0.77).

The occurrence of individual components of nonfatal heart attack (4.5 versus 5.2% with placebo; HR 0.62, 95% CI 0.49-0.77) was not significantly different. The results were the same in all empagliflozin doses.
The empagliflozin patients had a lower rate of heart failure hospitalization (2.7 percent versus 4.1%).
Patients taking empagliflozin had lower levels of A1C (mean 7.8 percent versus 8.2%) and reduced weight and waist circumference (with no rise in heart rate) as well as lower levels of uric acid.
Patients taking empagliflozin showed small increases in low-density lipoprotein cholesterol (LDL), and high-density lipoprotein (HDL).
The efficacy of Canagliflozin in patients with Heart Failure [Ref]:
In two studies that evaluated the safety and cardiovascular outcomes of canagliflozin in patients with type 2 diabetes (mean A1C 8.2%), 10,142 patients were randomly assigned to canagliflozin.
Most patients were on metformin and antihypertensives. The majority also took lipid-lowering drugs (equally distributed in both groups) to manage blood glucose, blood pressure, and cholesterol. About 50 percent of the patients in each group were using insulin.
The primary outcome, which was a composite of nonfatal stroke, death from nonfatal myocardial injury, and cardiovascular causes, occurred in fewer patients who were part of the canagliflozin study (26.9 versus 31.5 per 1000 patient-years, HR 0.86, 95%CI 0.75-0.97).

Statistics did not show statistically significant reductions in the incidence of individual components of the composite outcome among patients randomized to canagliflozin (11.6 versus 11.8, 9.7, and 11.6, respectively, and 8.4 versus 7.1 patients per 1000 patient-years, respectively).
The rate of heart failure hospitalizations was lower in the canagliflozin-treated group (5.5 versus 8.7 per 1000 patient-years in the placebo group; HR 0.67, 95%CI 0.52-0.87).
Patients taking canagliflozin had lower levels of A1C (mean difference -0.58%) and weight reductions.
A subsequent trial was designed to evaluate the renal outcomes of patients with type 2 diabetes. It showed similar reductions in cardiovascular events (6%).
The efficacy of Dapagliflozin in patients with heart failure [Ref]:
In a study to evaluate the effect of dapagliflozin (tendency 10 mg or placebo) on cardiovascular and renal outcomes in type 2 diabetes patients, 17.160 people were randomly assigned to either dapagliflozin (10mg) or placebo daily.
Most patients were on metformin and antihypertensives. The majority also took lipid-lowering drugs (equally distributed in both groups) to manage blood glucose, blood pressure, and cholesterol. About 40 percent of the patients in each group were using insulin.
The first primary outcome, a composite of nonfatal myocardial injury, death from cardiovascular causes or stroke, occurred in 8.8 percent and 9.4 percent of patients who took dapagliflozin, respectively (HR 0.93; 95% CI 0.84-1.03).
The second primary outcome, which is a composite of cardiovascular death and hospitalization for cardiac failure, saw a significant decrease in incidence (6.2 percent versus 8.5% with placebo, HR 0.73; 95% CI 0.681-0.88).

The death rate from any cause was not different between the two groups (6.2 percent versus 6.6% in the placebo group; HR 0.93, 95%CI 0.82-1.04).
Dapagliflozin trials included enough participants who had a history of cardiovascular disease or other risk factors and were randomized to dapagliflozin (or placebo) to conduct subanalyses between the two groups and compare them.
Dapagliflozin decreased the co-primary cardiovascular outcomes for participants who had previously suffered from myocardial damage (HR 0.84, 95%CI 0.72-0.99]).
However, it did not reduce the incidence of atrial fibrillation/atrial flutter adverse events in participants without prior myocardial injury (7.1 versus 7.1% [HR 1.00, 95%CI 0.88-1.13]).
In patients with diabetes or not, dapagliflozin has been shown in studies to decrease all-cause mortality and worsening heart failure in patients with heart failure with reduced Ejection Fraction (HFrEF).
This includes adults with heart failure with reduced Ejection Fraction (HFrEF), who are in New York Heart Association functional classes II, III, or IV [44].
The efficacy of Ertugliflozin (Steglatro) in patients with Heart Failure [Ref]:
In a study to assess the impact of lack of inferiority on composite cardiovascular outcomes, 8246 people with type 2 diabetes (mean A1C 8.2%) and prevalent CVD were randomly allocated to either ertugliflozin (15 or 15 mg) once daily.
Most participants who took part in the survey were on metformin. About 47 percent of patients were on insulin (76%).
The primary composite endpoint of death due to cardiovascular causes, nonfatal cardiac infarction, or stroke (ertugliflozin) was not superior to placebo after a mean follow-up of 3.5 years.
The hospitalization rate for heart failure was significantly lower than the 3.6 percent that was reported with placebo (HR 0.7, 95%CI 0.54-0.90].
These studies should be viewed in context. Although the relative cardiovascular benefits of empagliflozin or canagliflozin were impressive, they were only applicable to a high-risk population with already established CVD.
The absolute risk reduction of canagliflozin and empagliflozin is between 10 to 15 cases per 1000 patient years. Patients taking canagliflozin must balance the risk of having to have amputations.
There was no difference in blood glucose between the treatment groups, which suggests that the CVD result may have been due to extra-glycemic effects. It appears that SGLT2 inhibitors have a beneficial effect on heart failure outcomes.
Comparing the effect of SGLT2 Inhibitors drugs on microvascular Complications:
A growing number of clinical trials are evaluating microvascular outcomes for patients receiving SGLT2 inhibitors. A meta-analysis of three major CVD outcomes trials was done.
Empagliflozin (Jardiance), Canagliflozin (Invokana), and Dapagliflozin (Forxiga) reduced the progression of diabetic renal disease. A similar effect was observed in patients with CVD, or multiple risk factors [Ref].
The benefit was found to be present at all estimated glomerular filter rates (eGFRs), but it appeared to be less beneficial for those with severe kidney disease. Patients with an eGFR of 30 or 45 mL/min/1.73m² should not be initiated with SGLT2 inhibitors.
Although the mechanism of SGLT2 inhibitors’ reduction in nephropathy is multifactorial, it is believed to be primarily related to a direct renovascular impact.
Due to the short duration of the studies, and the modest improvement in glucose levels compared to placebo, it is unlikely that glucose-lowering could explain the decreases in late-stage nephropathy.
The effect of empagliflozin (Jardiance) on microvascular complication [Ref]:
The empagliflozin study was specifically designed to assess cardiovascular morbidity in patients with type 2, CVD, and established mortality.
The microvascular disease was an unspecified secondary outcome. In the empagliflozin-treated patients, there were 14 versus 20.5 percent who met the composite microvascular endpoint.
This was due to a decrease in the incident or worsening renal disease (defined as progression of macroalbuminuria or doubling of serum creatinine levels or death from kidney disease) which occurred in 12.7 percent and 18.8 percent respectively in empagliflozin (HR 0.61, 95%CI 0.53-0.70] [Ref].
Except for the death from renal disease, there were significant reductions in all components of the outcome. Three deaths due to renal disease occurred in the empagliflozin-treated group (0.1%), while none were reported in the placebo group.

Read: Side effects of Jardiance (Empagliflozin): SGLT2 Inhibitor
The effect of Canagliflozin (Invokana) on microvascular complications [Ref]:
In the canagliflozin study (described above), which assessed cardiovascular, renal, and safety outcomes for patients with type 2 diabetes and a high risk of developing complications, progression to albuminuria (a secondary outcome) was less frequent in the canagliflozin-treated group (89.4 participants per 1000 patient-years compared to 128.7 in the placebo group; HR 0.73, 95%CI 0.67-0.79).
A posthoc exploratory analysis of a composite result of a sustained 40 percent decrease in estimated glomerular filter rate (eGFR), showed that the need for replacement therapy or death from kidney causes was less frequent in the canagliflozin group than in the placebo group (5.5 versus 9.0 patients per 1000 patient-years, HR 0.60; 95% CI 0.47-7.777).

A subsequent trial was specifically designed to assess renal outcomes. 4401 patients with type-2 diabetes and albuminuria (mean glucose level 56.2 mL/min/1.73m², median urine albumin-to-creatinine ratio 927 [mg/g]), were randomly assigned to canagliflozin 100 mg daily or placebo [Ref].
A majority of patients were on insulin and/or Metformin. About 30 percent were on a sulfonylurea. All patients received an angiotensin-converting enzyme inhibitor or angiotensin blocker. After a median follow-up of 2.6 years, the trial was terminated early to preserve its benefits.
The primary outcome, which was a combination of ESKD, doubling of serum creatinine, or death due to renal or cardiovascular disease, occurred in a lower proportion of patients receiving canagliflozin (43.2 versus 61.2 events per 1000 patient-years, HR 0.70, 95%CI 0.59-0.82).

Except for renal death (two versus five patients who died from it), the effect size was comparable across all components of the primary outcome.
The most significant renal protective effect was observed in patients with an eGFR of 45 to 60 mL/min/1.73m² at study onset. However, it was also seen in patients with eGFRs as low as 30mL/min/1.73m².
The effect of Dapagliflozin (Forxiga) on microvascular complications [Ref]:
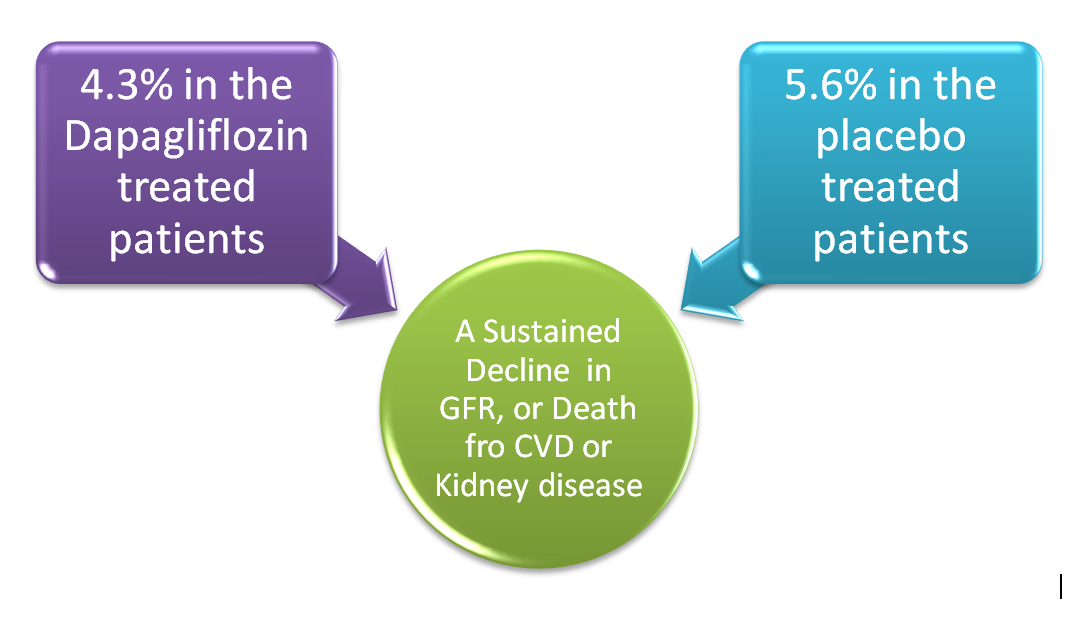
In the dapagliflozin study, which assessed cardiovascular and renal outcomes for patients with type 2 Diabetes who had or were at high risk of developing CVD, there was a decrease in the renal outcome.
This is a combination of a sustained decline of 40 percent or more of eGFR to 60 mL/min or death from kidney or cardiovascular disease. It occurred in 4.3 percent and 5.6 percent respectively in the dapagliflozin.
A subsequent trial was conducted to evaluate renal outcomes. 4304 patients with an eGFR of 25 to 75 mg/min/1.73m2 and a urine albumin-to-creatinine ratio 200-5000 mg/g (median, 995 mg/g), were randomly assigned to either dapagliflozin (10mg once daily) or placebo [Ref].
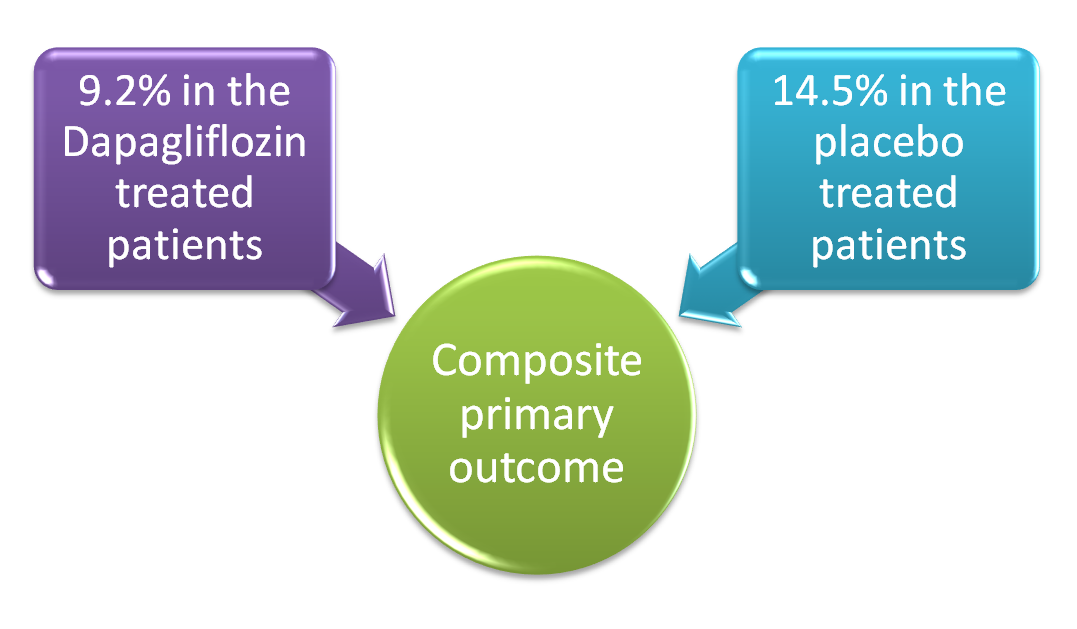
The composite primary outcome, sustained decline in eGFR >=50%, ESKD or death due to renal or cardiovascular disease, occurred in fewer patients who were in the dapagliflozin-treated group (9.2 versus 14.5%), HR 0.61, 95% confidence interval (CI 0.51-0.72).
Except for renal death (two versus six patients who died from it), the benefit was similar across all components of the primary outcome.
The effect of Ertugliflozin (Steglatro) on Microvascular Complications [Ref]:
In the ertugliflozin study that assessed cardiovascular outcomes in patients with type-2 diabetes and prevalent CVD (3.2 percent versus 3.9%) [HR 0.81; 95% CI 0.63-1.04].
The trend is statistically insignificant, but it is similar to other drugs of the same class, despite the stricter prespecified renal outcomes.
Comparing the weight loss effect of SGLT2 Inhibitors Drugs:
SGLT2 Inhibitors Drugs have been proven to cause sustained weight loss. SGLT2 inhibitors reduce weight. It appears that the weight loss is sustained over time.
A meta-analysis of longer-term trials (one- to two years) comparing SGLT2 inhibitions with placebo showed a significant weight loss with SGLT2 inhibits (mean difference at 2 years -2.99kg, 95% CI -3.64 – -2.34) [Ref].
Conclusion:
SGLT2 Inhibitors Drugs have beneficial roles in diabetic patients with cardiovascular diseases, kidney diseases, and atherosclerotic diseases.
These drugs have a modest effect on plasma blood glucose and cause sustained weight loss over time.
Join Our Organic Movement: Buy Our Premium Berberine Tea