Nocturnal Hypoglycemia is when your blood sugar falls at night. It is a serious condition and is often misdiagnosed since the symptoms may not be recognized.
Furthermore, the body responds by increasing blood sugar. Thus, patients have hyperglycemia in the morning, which is then wrongly treated by increasing the dose of diabetes medications.
What is Nocturnal Hypoglycemia?
Nocturnal hypoglycemia is generally described as low blood sugar levels at night. It frequently happens among those who take insulin to treat their diabetes.
However, it can be observed with any diabetes medication. Nocturnal hypoglycemia can also occur if a person misses his/ her dinner.
The symptoms of hypoglycemia may occur at different blood glucose levels in different people, depending on the person’s body response.
People who have prolonged hyperglycemia may develop symptoms of hypoglycemia even at a blood glucose level of 100 to 150 mg/dl.
Generally, hypoglycemia is when a person’s blood glucose levels fall below 70 mg/dl while sleeping.
According to studies, about half of all low blood glucose episodes and more than half of all severe episodes occur at night while sleeping.[Ref]
Daytime hypoglycemia is frequently treated by monitoring blood sugar levels and responding to symptoms.
Hypoglycemia, during the night, on the other hand, may go unnoticed. As a result, blood sugar levels may fall to dangerously low levels.
You can treat and prevent nighttime hypoglycemia with a few key techniques. Understanding the causes and taking steps to prevent blood sugar levels from falling are both effective ways to minimize the risk.
This can be avoided with proper planning and training of roommates and partners in how to recognize and treat it.

Who is at risk of developing Nocturnal Hypoglycemia?
Nocturnal hypoglycemia occurs almost always in people who have diabetes. It is commonly a side effect of diabetes medications rather than a disease state.
Exogenous insulin and other diabetes medications cannot replicate the normal physiological insulin secretion. An imbalance in blood glucose and insulin levels might cause hypoglycemia.
Factors that might lead to hypoglycemia among people who take insulin are:
HbA1c levels less than 6:
People with tightly controlled blood glucose are more at risk of developing hypoglycemia than those with poorly controlled blood glucose levels.
Moderate to high-intensity exercises during the day or before sleeping:
A high-intensity exercise causes the shift of glucose from the blood to the muscles that is not dependent on the plasma insulin levels.
Episodes of hypoglycemia during the day:
People who have hypoglycemia during the daytime are at risk of developing hypoglycemia at night as well. This is indicative of an overall overtreatment.
The low blood glucose level at bedtime that goes unmonitored:
People who do not monitor their blood glucose at night are at risk of developing low blood glucose at night.
Alcohol consumption:
Alcohol is rapidly utilized by the body. People who use alcohol have poor glycogen reserves and therefore are at an increased risk of developing nocturnal hypoglycemia.
A diet too low in carbohydrates:
People consuming fewer carbohydrates at night such as those on a weight loss diet and high-protein diet may develop nocturnal hypoglycemia.
High dosage of insulin:
This is probably the most common cause of nocturnal hypoglycemia. The insulin dose is often increased when the fasting or early morning blood glucose is high.
However, in some cases, fasting hyperglycemia is due to the body’s response to nocturnal hypoglycemia. This is called the Somogyi effect.
Inappropriate timings of taking insulin:
Administering insulin at times other than the prescribed time may cause the blood glucose to fall at midnight.
Skipping meals:
Skipping meals or people who develop nausea, vomiting, or diarrhea are also risk factors for nocturnal hypoglycemia.
What are the symptoms and signs of Nocturnal Hypoglycemia?
When people are awake during the day, they usually notice when their blood sugar is low because of symptoms or because they monitor their sugar levels, but these signs often go unnoticed during the night.
People who have Nocturnal Hypoglycemia can have any of the following signs and symptoms, depending upon the severity of hypoglycemia:
- Excessive sweating
- Shaking or trembling
- Increased heart rate
- Irritability, tiredness, and confusion after waking up
- Crying out during sleep
- Having vivid dreams or nightmares
- Restlessness
- Rapid or slow breathing
Most of the above symptoms may be related to a sleep disorder. Occasionally, nightmares and abnormal dreams may be the only symptoms.
Some people notice early morning fatigue, tiredness, and confusion and may relate these symptoms to stress.
High blood sugar in the morning may be the only sign of nocturnal hypoglycemia. This is also called paradoxical hyperglycemia or the “Somogyi effect“.
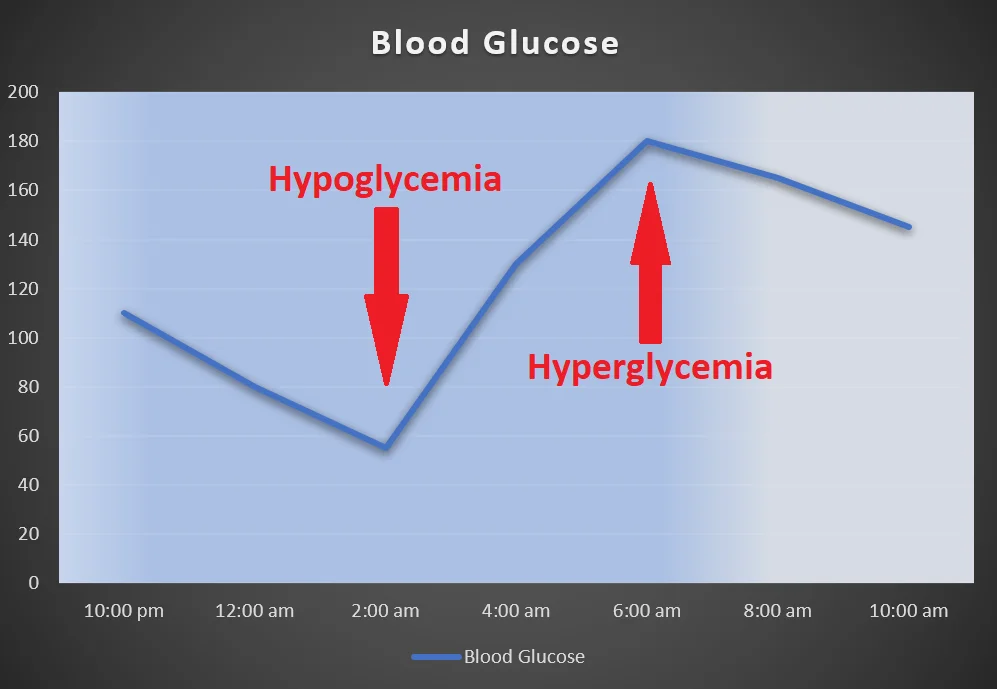
When the blood glucose drops to less than 70 mg/dl, counter-regulatory hormones are produced by the body to raise the blood glucose.
These include stress hormones, including cortisol and adrenaline. These hormones raise the blood glucose and the patient can develop fasting hyperglycemia.
It is very important to keep in mind the Somogyi effect since increasing the night-time insulin may result in further hypoglycemia. Severe hypoglycemia can be fatal.
It is important to check the blood glucose with a glucometer at night (preferably at 1 o’clock) to confirm hypoglycemia. Alternatively, patients may reduce their nighttime insulin.
If reducing the nighttime insulin corrects the fasting hyperglycemia, then the person has Somogyi’s phenomenon due to an overdose of diabetes medications, especially insulin.
How can you Diagnose Nocturnal Hypoglycemia?
Nocturnal hypoglycemia is difficult to detect because it goes unnoticed during sleep. However, a roommate or partner can detect it based on the above-mentioned signs and symptoms.
Another way to detect nighttime hypoglycemia is a Continuous Glucose Monitor (CGM).
A continuous glucose monitor (CGM) is a gadget that monitors blood glucose levels throughout the day and night.
If the blood glucose drops too quickly, an alarm will sound. If a person has nocturnal hypoglycemia, this device is loud enough to wake them up.
In developing countries, these gadgets may not be available. Waking up at 1 o’clock and checking blood glucose with a glucometer is also acceptable and can confirm the diagnosis of nocturnal hypoglycemia in most cases.
How to prevent Nocturnal Hypoglycemia?
Some prevention tips include:
Check your sugars:
Check your blood glucose levels before going to bed. If the levels are close to 70mg/dl during bedtime, then there might be a risk of hypoglycemia at night.
To avoid this, you must take complex carbohydrates like apples and some sandwiches, whole grain toast, etc.
Don’t skip your dinner:
Avoid skipping your dinner. Or if you skip dinner, you must skip rapid-acting insulin too. This will reduce the risk of decreased blood sugar levels.
You must always match your meals with your medications.
Avoid strenuous activity at night:
Monitor your blood sugar levels before and after a workout. Avoid high-intensity exercises during nighttime.
If your blood glucose levels are low before or after the workout, consume 10-15 grams of carbohydrates (such as an apple or bran bread).
Avoid alcohol consumption.
Alcohol shifts glucose metabolism. It also causes liver injury and may result in hypoglycemia.
Adjust your diabetes medications:
You can also switch your diabetes medications. Preferably, sulfonylureas and other diabetes medications that lower the plasma glucose should be taken in the morning.
If you are on twice-daily premixed insulin, it is better to take about two-thirds of your dose in the morning and one-third in the evening.
People on NPH insulin may be switched to glargine or Degludec. Degludec is associated with far fewer events of nocturnal hypoglycemia than glargine and NPH insulin.
What is Hypoglycemia unawareness?
Some people are unaware that they have hypoglycemia. They might not show any of the physical signs of low blood sugar.
These people are more likely to sleep through a nocturnal hypoglycemic episode.
This is often caused by continuous episodes of hypoglycemia that lead to failure of the autonomic nervous system. [Ref]
They’re also more likely to develop severe hypoglycemia (less than 55 mg/dL), which can be difficult to manage without help.
You’re more likely to be unconscious of hypoglycemia if:
- You’ve been dealing with diabetes for a long time (5-10 years)
- You get low blood sugar episodes on a regular basis.
- You take beta-blockers and other drugs that blunt the adrenergic effects in response to hypoglycemia.
The treatment of hypoglycemia unawareness is difficult and requires a comprehensive approach that includes clinical care and systematic patient education.
How to treat Nocturnal Hypoglycemia at home and in the hospital:
Early recognition is crucial for the treatment of nocturnal hypoglycemia. Studies suggest that the following treatment options can be effective.[Ref]
If you are awake, mild to moderate hypoglycemia can be treated by ingesting a snack that contains approximately 5 grams of simple carbohydrates.
These include cookies, sandwiches, or glucose tablets. This can increase blood glucose levels by 15-20 mg/dL
High-fat foods must be avoided while treating hypoglycemia, these foods delay the absorption of glucose which prolongs the episode of hypoglycemia.
Subcutaneous glucagon is administered if the hypoglycemia is suspected to be severe. Glucagon stimulates gluconeogenesis and glycogenolysis which raises blood glucose levels rapidly.
If the patient does not rapidly respond to glucagon, intravenous glucose must be administered by a health care professional.
Glucose is usually administered orally in patients with mild symptoms and who are conscious. Intravenous 50% glucose is required in patients with severe hypoglycemia.
It is important to observe the patient at the hospital for some time after the correction of hypoglycemia. The observation period depends on the medications and co-morbid conditions of the patients.
People on long-acting hypoglycemic medications like glyburide (Glibenclamide or Daonil) may need observation for three to five days.
Why is it important to treat Nocturnal Hypoglycemia?
Frequent and prolonged episodes of hypoglycemia might put you at risk of other medical complications such as:
- Weakness
- Dizziness
- Cognitive Impairment
- Cardiovascular disturbance
- Coma
- And even Death
People with cardiovascular conditions and elderly frail patients may develop angina because of the increased adrenergic stimulation in response to hypoglycemia.
Sudden death is a rare complication of nocturnal hypoglycemia, especially in elderly patients.
Causes of Nocturnal Hypoglycemia in Non-Diabetic Individuals
Besides the diabetic population, several other conditions might also cause nocturnal hypoglycemia such as:
- Gastric bypass surgery
- Enzyme deficiencies
- Carbohydrate sensitivities
- Low levels of certain hormones, such as adrenal insufficiency and hypothyroidism
- Pancreatic tumors, especially insulinomas (insulin-secreting tumors)
- Alcohol users
- Malignant conditions (insulin-secreting paraneoplastic syndromes)
- Advanced liver, kidney, or cardiac diseases
- Medications other than diabetes medications, such as antimalarials, quinolones, and beta-blockers
When to Contact Your Doctor?
Once you know or suspect you’ve had nocturnal hypoglycemia, it’s critical to contact your doctor. Your diabetes care plan can then be discussed with your doctor.
Your doctor may advise the following options:
- Changing the dosage, timing, or type of insulin
- Altering the dosage and timing of other anti-diabetic medications
- Creating a novel blood glucose monitoring approach, such as continuous glucose monitoring
Conclusion:
Low blood sugar during sleep is known as nocturnal hypoglycemia. To minimize the risk, keep a close check on your blood sugar levels and stick to a healthy diet and insulin-dosing schedule.
If you have nocturnal hypoglycemia, work with your doctor to come up with a solid management plan to avoid it in the future.








