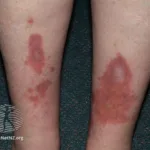
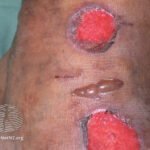
Diabetic Retinopathy is the leading cause of blindness in adults. Blindness can have a severe impact on a person’s life. It severely impairs the quality of life.
Because diabetic retinopathy is the earliest microvascular complication of diabetes, it is often diagnosed when it is already too late.
The ADA recommends fundoscopic examination on diagnosis and then yearly thereafter in patients with Diabetes mellitus Type 2.
The initial eye examination is recommended after five years of diagnosis in Type 1 Diabetes patients and then yearly thereafter.
| Buy: | Read: |
Diabetes – Need to Change Your Lifestyle!
Due to several reasons, diabetes is the most frequently occurring disorder that affects people of all ages but mainly adults.
Risk factors of diabetes including an unhealthy lifestyle, genetics, stress, and many others are commonly found in people.
Diabetes can be prevented but once it has developed it can lead to several other disorders which can be life-threatening if not controlled.
These disorders affect a person’s normal life activities and functioning. Diabetes can drop the quality of life of people who suffer from it so it is wise to control and manage it when you can.
One such disorder that greatly affects diabetics is diabetic retinopathy which is described in detail below.
| Buy: | Read: |
What Do We Know About Diabetic Retinopathy
Diabetic retinopathy, as the name suggests, is one of the most frequent complications of Diabetes. In fact, it is the most common cause of blindness worldwide.
Diabetic retinopathy can affect anyone with diabetes, regardless of the type of diabetes. However, it is most common in individuals with uncontrolled diabetes and those with long-standing diabetes.
Because diabetes affects mainly the blood vessels, and the smaller blood vessels are more prone to get affected, retinopathy is one of the frequent complications.
The retina is one of the most vascular parts of our eyes. Uncontrolled diabetes and glycated end-products damage these fragile blood vessels resulting in visual impairment and blindness.
Diabetic retinopathy can go undetected because it shows no symptoms at the start which is why it usually progresses towards blindness.
Learning about its symptoms can be lifesaving as it can aid in the early detection of it.
| Buy: | Read: |
Stages of Diabetic Retinopathy
Diabetic retinopathy progresses in four stages which are explained here.
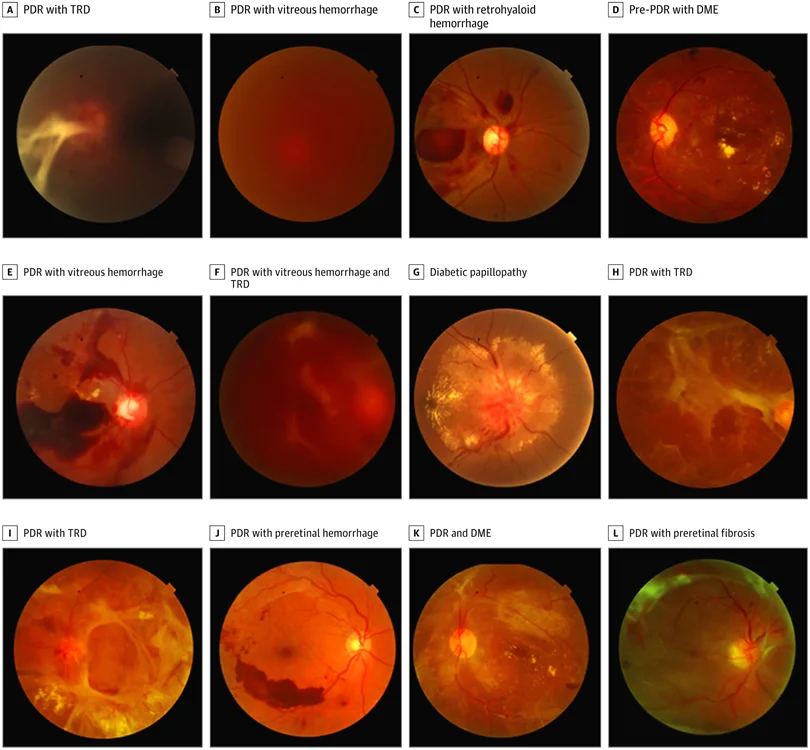
Mild non-proliferative diabetic retinopathy
In the initial phase of diabetic retinopathy, small swellings are formed on the blood vessels of the retina. These are called microaneurysms. Aneurysms are abnormal point dilatation of blood vessels.
At this stage, fluid can leak into the retina which will cause the swelling of the macula which is close to the center of the retina.
The risk of progression to proliferative diabetic retinopathy is 5% per year. At this stage, adequate control of blood glucose is very important to stop the progression of the disease.
Patients should have a retina exam after one year at this stage. Referral to an ophthalmologist is not recommended at this stage.
Moderate non-proliferative diabetic retinopathy
This is the second stage of diabetic retinopathy and involves the accumulation of blood and other fluids in the macula due to the impaired blood flow to the retina caused by the swollen areas.
These are seen as cotton wool spots, microhemorrhages, venous beading, and hard exudates.
The risk of progression to proliferative diabetic retinopathy ranges from 12 to 27% after one year.
Patients should be followed after 6 to 8 months. At this stage, there is no need to refer the patient to an eye specialist.
Severe non-proliferative diabetic retinopathy
Severe non-proliferative diabetic retinopathy is characterized by worsening of the symptoms of moderate diabetic retinopathy and progression to proliferative diabetic retinopathy.
The patient has 20 or more intra-retinal hemorrhages, venous beading at two or more sites, and at least one area of Intraretinal microvascular abnormality (IRMA).
The risk of progression to Proliferative Diabetic Retinopathy is 52% within one year.
These patients should be followed every 3 to 4 months for adequate diabetes control and should be referred to an eye specialist as well.
These patients may need fluorescein angiography and should be examined for macular edema.
Proliferative diabetic retinopathy
The fourth and final phase of diabetic retinopathy has new blood vessels created which are weak and prone to leakage so, this can generate vision issues like blurriness or even blindness.
These patients have neovascularization at the disk, neovascularization elsewhere, and retinal hemorrhages.
These patients need immediate referral to an eye specialist. At this stage, patients may require laser photocoagulation or intra-retinal injection of VEGF (vascular endothelial growth factor) in addition to laser photocoagulation.
These patients must be followed at monthly intervals to halt the disease progression.
| Buy: | Read: |
Symptoms of Diabetic Retinopathy
Knowing about the symptoms in advance can help with the early detection of the disease and taking measures to prevent it
- Sudden problem with your vision:
- sudden inability to see properly
- Fluctuations in vision:
- seeing properly at one time and improperly at other times
- Pain in the eyes:
- pain like dull aches in the eyes
- Redness in the eyes:
- visible redness in the eyes due to the swollen blood vessels
- Night blindness:
- inability to see in the dark
- Blurry vision:
- not being able to see clearly
- Empty areas in the vision:
- empty spots in your field of vision
| Buy:
| Read: |
Causes of Diabetic Retinopathy
Diabetic retinopathy can be caused by an excessive level of blood sugar level in the body.
The high levels of sugar in the blood vessels of the retina can lead to blockage which leads to leakage of fluid or blood causing problems in the vision.
This induces the formation of new blood vessels that are abnormal and fragile.
Which Individuals are at the Greatest Risk of Diabetic Retinopathy?
Multiple risk factors increase the risks of individuals developing retinopathy, they are given here
- History of diabetes
- Uncontrolled or poorly controlled diabetes
- Elevated cholesterol levels
- Elevated blood pressure
- Pregnancy with diabetes
- Smoking or tobacco use
In addition, rapid changes in blood glucose can also increase the chances of progression of the disease.
Certain medications especially Insulin and the novel GLP-1 analog, Semaglutide, have been especially associated with the development and progression of diabetic retinopathy.
| Buy: | Read: |
Types of Diabetic Retinopathy
There are two types of DR:
Early Diabetic Retinopathy
Also called non-proliferative retinopathy in which there is no development of new blood vessels.
In this case, the blood vessels start to weaken and small protruding areas develop on the blood vessels which causes leakage of fluid.
With the passage of time, blood vessels become blocked and the condition worsens. Larger blood vessels become deformed. This damage can also cause edema in the macular region.
Advanced Diabetic Retinopathy
The early DR can progress into a severe condition that involves the development of new blood vessels as the old ones are damaged.
These new ones are fragile and can leak fluid in the vitreous area of the eye and if they interfere with the flow of fluid out of the eye then the pressure will build up in the eyeball leading to glaucoma by damaging the nerve.
| Buy: | Read: |
Associated Complications of Diabetic Retinopathy:
Diabetic retinopathy brings with it a series of complications.
Glaucoma
As described above, glaucoma occurs when new blood vessels interfere with the normal flow of fluid out of the eye causing a buildup of pressure.
This pressure damages the optic nerve which serves the function of carrying images from the eye to the brain.
Retinal detachment
The blood vessels can cause the formation of scar tissue which induces the separation of the retina from the eye leading to vision problems like empty spots in the field of vision or flashes of light.
Vitreous hemorrhage
The leakage of blood from the newly formed blood vessels in the jelly-like material called the vitreous area can cause you to see a few dark spots but if the bleeding is excessive then it can block the entire vision.
Blindness
All of the conditions stated above can eventually lead to complete vision loss.
| Buy: | Read: |
How to Prevent Diabetic Retinopathy
Managing your blood sugar level is the key step to preventing any other complication.
It is recommended to perform physical activity like exercising for at least 150 minutes per week and choose a healthy meal every day that includes fruits, vegetables, and low-fat milk.
Also, monitor your blood sugar level daily to control hyperglycemia. Choose a healthy lifestyle and quit smoking.
Keep a check on your vision and instantly report to your doctor if you see or experience any changes.
Get a dilated eye exam every year since diabetic retinopathy is asymptomatic at the start and can be detected through this exam.
| Buy: | Read: |