Diabetes during pregnancy is treated primarily with insulin and metformin. Among oral medications, the only drug that was thought to be relatively safer than others was Glyburide (Glibenclamide or Daonil).
However, a recent study found that sulfonylureas are associated with a relatively increased incidence of congenital malformations compared to other oral or injectable medications for gestational diabetes or type 2 diabetes during pregnancy.
Because drug testing in pregnancy has its specific legal and ethical implications, data is limited to clearly identify the safest medications for gestational diabetes mellitus.
What Researchers Found That Might Be a Turning Point in the Management of Gestational Diabetes?
- Researchers looked into the possibility of major birth abnormalities in pregnant women with type 2 diabetes who were using medications other than insulin.
- Data from the Israeli Maccabi Health Services database, the US MarketScan database, and four Nordic nations were studied between 2009 and 2021.
- The study found that medications other than insulin to treat type 2 diabetes in pregnant women have increased.
- Mothers who took sulfonylureas, DPP-4 inhibitors, GLP-1 receptor agonists, or SGLT2 inhibitors did not report a relatively high risk of birth defects in their newborns when compared to the mothers who used insulin
- Even though a significant risk of higher birth defects was not associated with the use of non-insulin meds still, further research is required.
The number of women being diagnosed with T2DM is increasing day by day. This leads to a higher use of non-insulin antidiabetic medications during pregnancy.
If someone with type 2 diabetes is not effectively managing their blood sugar with metformin, sulphonylureas, or insulin, or if the treatment goal involves weight loss, preventing hypoglycemia, or reducing cardiovascular risk, a doctor may recommend prescribing a GLP-1 agonist or SGLT2 inhibitor.
Although GLP-1 agonists and SGLT2 inhibitors are widely used for managing glucose levels in clinical practice, there is a significant lack of information regarding their safety during pregnancy and lactation.
In pregnancy, inadequate control of blood sugar is a recognized risk for major birth defects.
While some guidelines suggest considering metformin during pregnancy, there is a lack of information on the safety of other non-insulin antidiabetic medications in this context.
A recent study aimed to assess if using certain non-insulin medications for type 2 diabetes during pregnancy increased the risk of major birth defects.
Their conclusion suggests that while there’s a rising use of non-insulin medications, the risk of birth defects does not seem significantly higher compared to insulin, providing some reassurance. [ref]
However, further studies are needed for confirmation, and ongoing monitoring will provide more precise information as more data accumulate.
| Read: |
Study Methodology:
As a part of the International Pregnancy Safety Study Consortium, this study analyzed data from Nordic countries, the US, and Israel on pregnant women with type 2 diabetes and their live-born infants (2009-2021).
Using log-binomial regression, they compared the risks of significant birth abnormalities with insulin and non-insulin drugs during the periconceptional period. Cohorts were from population registers and health databases.
Exclusions included fetal chromosomal abnormalities and teratogenic exposure. Ethical approvals were obtained.
Pregestational type 2 diabetes in women was identified, and periconceptional exposure to specific drugs was defined.
Major congenital malformations (MCM) were assessed, and covariates like maternal age were considered. Meta-analysis combined results across cohorts.
| Read: |
Study Analysis:
In this study, they looked at more than 3.5 million pregnancies. Out of these, 51,826 women had type 2 diabetes before pregnancy.
About 29% of these women used certain non-insulin medications during pregnancy, and this varied in different countries.
The study also checked if different diabetes medications (like metformin, insulin, sulfonylureas, DPP-4 inhibitors, GLP-1 receptor agonists, and SGLT2 inhibitors) were linked to a higher chance of serious birth defects in babies.
Scientists found that the likelihood of serious birth defects differed depending on the type of medication used.
The risk was lowest in babies not exposed to specific diabetes medications or only exposed to metformin.
The study also concluded that when comparing certain medications like sulfonylureas or GLP-1 receptor agonists to insulin, there was no notable increase in the risk of birth defects.
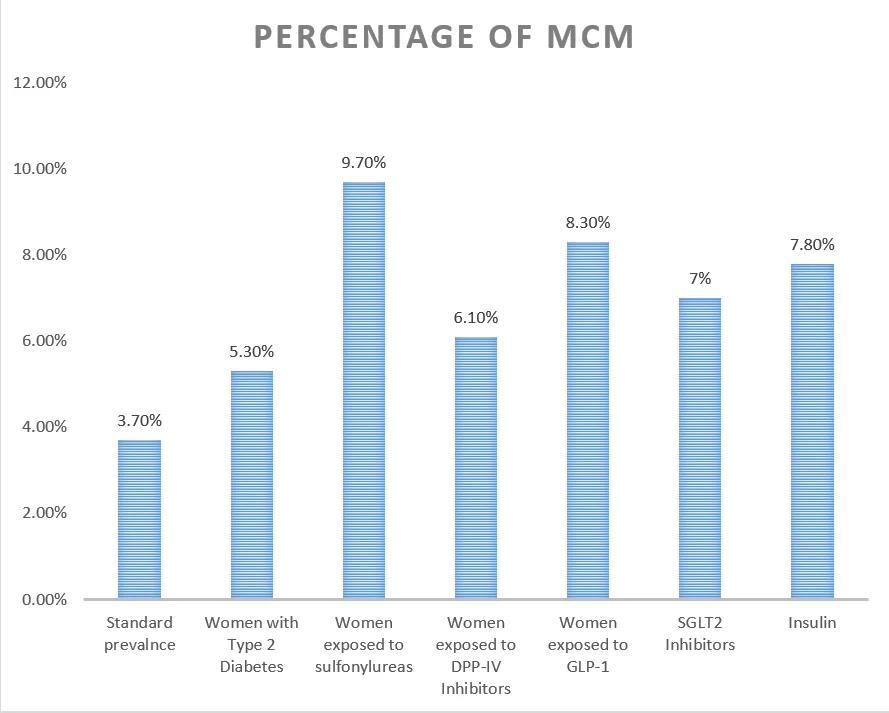
| Population | Percentage of infants with MCM (major congenital malformations) [Ref] |
| Standard prevalence | 3.7% |
| Women with Type 2 Diabetes | 5.3% |
| Women exposed to sulfonylureas | 9.7% |
| Women exposed to DPP-IV Inhibitors | 6.1% |
| Women exposed to GLP-1 | 8.3% |
| Women exposed to SGLT2 Inhibitors | 7% |
| Women on Insulin | 7.8% |
The study’s reassurance about using these medications during pregnancy remained consistent even when looking at prescriptions in the first trimester. However, it highlights the need for continuous monitoring and more research.
The relative risk of developing MCMs (major congenital malformations) was highest with sulfonylureas and lowest in women exposed to DPP-IV inhibitors [Ref].
Insulin Vs other antidiabetic medications | Adjusted RR (relative risk of MCM) |
| Women exposed to sulfonylureas | 1.18 |
| Women exposed to DPP-IV Inhibitors | 0.83 |
| Women exposed to GLP-1 | 0.95 |
| SGLT2 Inhibitors | 0.98 |
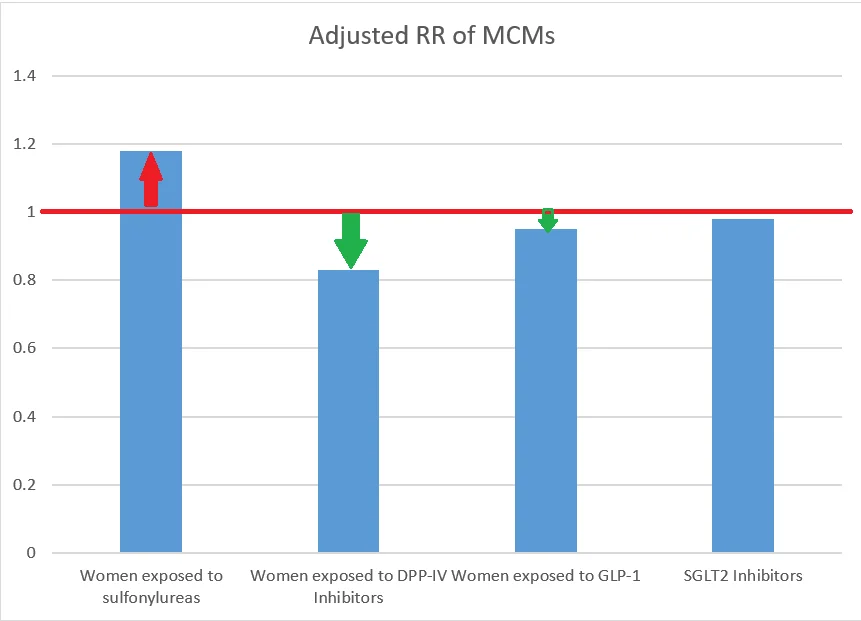
It is obvious that except for sulfonylureas, other medications for gestational diabetes mellitus are not associated with an increased risk of fetal malformations.
In addition, although SGLT2 inhibitors are not associated with major congenital malformations, they may cause urinary tract infections in pregnant women which can cause small for gestational age and other fetal complications.
| Read: |
The bottom line:
To improve the study’s dependability, the researchers tried replicating an actual clinical experiment. The study also provided important information regarding the safety of some non-insulin antidiabetic medications during pregnancy.
However, there are certain restrictions, and the estimations are not precise because there aren’t enough infants exposed to particular medications.
Due to potential bias, the study was unable to include pregnancies that ended in miscarriage, stillbirth, or termination.
It will take more investigation to validate these results. Nevertheless, the study’s antidiabetic medications are thought to be safe to take while pregnant.
| Read: |