A special type of Thyroid Cancer called Medullary Thyroid Cancer (MTC) has been associated with Ozempic (semaglutide), Rybelsus, and Wegovy.
All GLP-1 analogs, including Liraglutide (Victoza and Saxenda) and Dulaglutide (Trulicity), are associated with an increased risk of MTC.
GLP-1 analogs, including Ozempic (semaglutide), are thought to stimulate the C-cells of the thyroid gland to release calcitonin.
GLP-1 also causes C-cell proliferation and hyperplasia by upregulating the calcitonin gene expression.
Which cancers can occur in the thyroid gland?
The thyroid gland has two important cell types:
- The Follicular cells, and
- The C-Cells
The follicular cells are the most abundant and primarily responsible for the production of thyroxine (the iodination and de-iodination processes).
The C-Cells of the thyroid gland produce Calcitonin which is responsible for calcium regulation in our body. It lowers blood calcium levels by causing its deposition in the bones.
These two types of cells can rapidly proliferate and develop into cancer. There are five main types of thyroid cancers. These include:
- Papillary Thyroid Cancer
- Follicular Thyroid Cancer
- Hurthle Cell Thyroid Cancer
- Medullary Thyroid Cancer
- Anaplastic Thyroid Cancer
Papillary thyroid cancer is the most common cancer of the thyroid gland. Follicular thyroid cancer is the second most common thyroid cancer. Both papillary and follicular thyroid cancers account for more than 95% of the cases of thyroid cancers.
Medullary thyroid cancer accounts for 3% of all thyroid cancers. Hurthle cells and Anaplastic thyroid cancers are very rare.
Other cancers that can occur in the thyroid gland include non-Hodgkin’s lymphoma and sarcomas. Parathyroid adenomas and carcinomas occur outside but in close proximity to the thyroid gland.
Among the cancers mentioned above, medullary thyroid cancer is associated with genetic mutations of the RET proto-oncogenes and has a familial predisposition.
It is the medullary thyroid cancer that has been found in animals treated with GLP-1 analogs including Semaglutide (Ozempic, Rybelsus, and Wegovy).
What is Medullary Thyroid Cancer?
Medullary thyroid cancer accounts for up to 3% of thyroid cancers. It is derived from the C-cells of the thyroid gland that produces calcitonin.
75% of the cases of medullary thyroid cancers are sporadic, while 25% occur in patients who have a genetic mutation in the RET proto-oncogene and can be familial.
Mutations in the RET genes cause a syndrome called MEN (multiple endocrine neoplasia). MEN-1 and MEN-II are the most common, followed by mixed types.
MEN-1 syndrome is characterized by:
- Tumors of the anterior pituitary
- Pancreatic islet-cell tumors
- Parathyroid tumors
MEN-2 is further divided into two subtypes:
- MEN-2A is characterized by:
- Medullary thyroid cancer
- Pheochromocytoma
- Parathyroid tumors
MEN-2A can also occur with Hirschsprung disease and lichen amyloidosis.
- MEN-2B is characterized by:
- Medullary thyroid carcinoma
- Pheochromocytoma, and
- Mucosal neuromas
MEN-2 B patients may have a Marfanoid habitus.
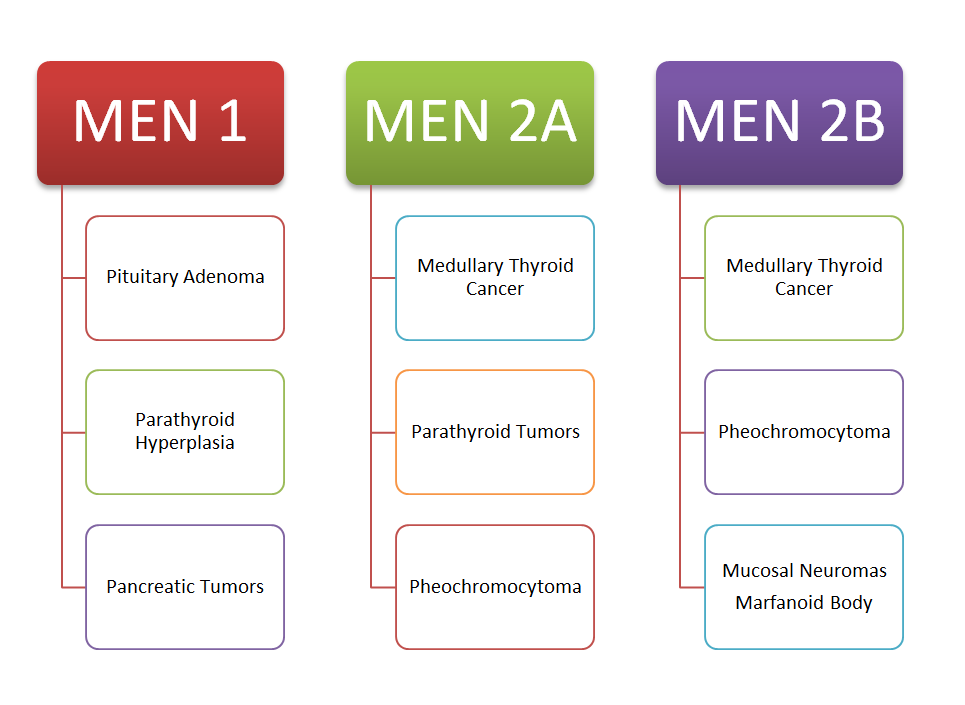
It can be seen here that MEN-II syndromes (Both MEN-II A and MEN-II B) predispose patients to medullary thyroid cancers.
Thus, patients who have MEN-II syndromes are at risk of developing medullary thyroid cancer if they are given Ozmepic (or any other GLP-1 analog).
It is also likely that medullary thyroid cancer may be the first presentation of a person who has MEN-2 syndrome. It is this subgroup of patients who are at high risk of developing MTC when started on Ozempic (Semaglutide).
Genetic testing for RET gene before Ozempic treatment initiation is not recommended because of the very low prevalence of the disease.
However, patients started on Ozempic must be advised to report to the doctor and stop Ozempic immediately if they develop any of the following symptoms:
- Lump or lumps in the neck
- hoarseness of voice
- Bone pains
- Weight Loss
- Lethargy and Fatigue
- Persistent Diarrhea or new-onset cushingoid features (Buffalo hump, moon facies, abdominal striae, Hypertension, and Diabetes).
Patients who have a multinodular thyroid gland, and those with a history of papillary or follicular thyroid cancers are not at risk of developing medullary thyroid cancer when started on Ozempic treatment.
Patients who develop a neck lump while on Ozempic treatment may be advised of the following tests:
- Calcitonin levels
- Ultrasound of the thyroid gland
- FNAC of the thyroid gland.
Who is at risk of developing Medullary Thyroid Cancer?
Medullary thyroid cancer can occur in patients who have multiple endocrine neoplasias (MEN) type II syndrome. These syndromes can be inherited in an autosomal dominant pattern.
All patients with MEN-2A, also called Sipple Syndrome, have Medullary thyroid cancer. 50% of these patients may develop pheochromocytoma, and 10 – 20% of these patients can also develop parathyroid adenomas.
All patients with MEN-2B have medullary thyroid cancer, which occurs at around 10 years of age. 50% of these patients have pheochromocytoma, and 50% of patients have marfanoid body habitus (tall stature, high-arch palate, and lax skin).
MEN-2B has an aggressive course. Patients develop MTC at the age of 10 years, while MTC develops in patients with MEN-2A at the age of 10 to 20 years.
How frequently is Ozempic associated with Thyroid Cancer?
Ozempic (and other formulations of Semaglutide, like Rybelsus and Wegovy) have been associated with an increased risk of medullary thyroid cancer.
Although no cases of Medullary thyroid cancer have been reported in humans using Ozempic, in animal studies, the risk of developing MTC was high in mice treated with Ozempic.
The risk of developing Medullary Thyroid Cancer was dependent on the dose and duration of Ozempic use.
Post-marketing cases of MTC have been reported in patients using Liraglutide, another drug from the same class as Ozempic.
Because of the association of MTC in animal studies and post-marketing cases of MTC in patients using Liraglutide, Ozempic (Semaglutide) is contraindicated in the following high-risk patients:
- Patients with a personal or family history of MTC (medullary thyroid cancer)
- Patients with MEN-2 syndrome
In addition, all patients must be asked to discontinue treatment and report if any of these symptoms develop while using Ozempic:
- Neck swellings or lumps in the neck
- Difficulty in swallowing (Dysphagia)
- Hoarseness of voice, especially if persistent and not relieved with symptomatic treatment
- Fatigue, skeletal pains, diarrhea, and cushingoid appearance.
Pretreatment monitoring of Calcitonin, Procalcitonin, or CEA (carcinoembryonic antigen) levels is not routinely recommended because of very low specificity.
However, the presence of a new-onset neck lump and high levels of calcitonin and CEA should warrant further investigations. These include FNAC of the lump and imaging such as ultrasound or CT of the neck.
Calcitonin levels exceeding 50 ng/L should never be disregarded. High-risk patients such as those with MEN-2 and patients with a neck lump and raised calcitonin levels, if missed, may file a lawsuit if they are on Ozempic or other GLP-1 analogs, or any other formulation of Semaglutide (Ryeblsus and Wegovy).
Which GLP-1 use is more strongly associated with MTC?
The association of thyroid cancers in patients using GLP-1 analogs was evaluated using the Eudravigilance database until 2020 [Ref].
The following GLP-1 analogs were analyzed:
- Liraglutide
- Exenatide
- Dulaglutide
- Albiglutide
- Semaglutide
The following thyroid cancers were diagnosed while patients were on GLP-1 analogs:
| Preferred Term used in the study | Total number of cases (236) | Percentage |
| Medullary thyroid cancer | 64 | 27.12 |
| Thyroid adenoma | 9 | 3.81 |
| Thyroid cancer metastatic | 6 | 2.54 |
| Thyroid cancer | 111 | 47.03 |
| Thyroid neoplasm | 46 | 19.49 |
The table above is not showing the specific type of thyroid cancer. These terms were used in clinical trials and the patient’s records. For example, “thyroid cancer” may mean papillary, follicular, or anaplastic thyroid cancer.
With regard to the number of cases of thyroid cancer in patients on the five different GLP-1 analogs, most cases were associated with Liraglutide.
The table here shows the number and percentage of thyroid malignancies (mentioned in the table above) in association with the various GLP-1 analogs:
| GLP-1 analog | Cases of Thyroid Cancers | Percentage of Cases |
| Albiglutide | 3 | 1.27 |
| Dulaglutide | 35 | 14.83 |
| Exenatide | 76 | 32.2 |
| Liraglutide | 113 | 47.88 |
| Semaglutide | 9 | 3.81 |
| Total Cases | 236 | 100 |
The number of cases of thyroid cancer in patients using Ozempic may increase since the drug is being used commonly compared to other GLP-1 analogs.
Medullary Thyroid Cancer (MTC) association with Ozempic or other GLP-1 analogs has not been mentioned here.
How to Detect Thyroid Cancer at an early stage?
Thyroid cancer can be detected earlier if the patient knows the symptoms and the healthcare provider keeps a low threshold of investigating any lump reported by the patient.
Symptoms of Medullary Thyroid Cancer can be very subtle. Patients should be asked to report symptoms of persistent hoarseness, change in voice, neck lump, difficulty swallowing, and systemic symptoms like weight loss, fatigue, and skeletal pains.
Thyroid ultrasound, Calcitonin levels, CEA (Carcinoembryonic antigen) levels, Procalcitonin levels, and FNAC may help in the early diagnosis of patients with MTC.
Patients with pheochromocytoma or parathyroid tumors and those with a family history of Medullary thyroid cancer or MEN-2 syndrome should also undergo genetic testing for RET gene mutations.
Patients with MEN-2 syndrome may develop MTC at the age of 10 to 20 years. Prophylactic thyroidectomy is recommended by most experts for high-risk patients.
In Conclusion:
Ozempic association with Medullary thyroid cancer should be kept in mind when prescribing Ozempic to any patient who has MEN-2 syndrome, has a family history of MTC or MEN-2, and who develops symptoms of MTC.
A neck lump in a patient should be investigated by measuring blood levels of calcitonin, performing an ultrasound of the neck, and an FNAC of the thyroid gland.
- Premium Ingredients: Our tea blend features high-quality Berberine, aromatic Oolong, and refreshing Mint, all organicall…
- Mint Flavored: Enjoy the cool, crisp taste of mint that perfectly complements the robust flavors of Berberine and Oolong…
- Unsweetened with Zero Calories: Crafted for those who appreciate the natural flavors of tea, our blend is completely uns…
- Supports Healthy Thyroid Functions—We use a proprietary blend of vitamins and minerals combined with natural herb extrac…
- Promotes Mental Clarity and Focus—Our supplement contains nutrients that not only support healthy thyroid functions but …
- Supports a Healthy Metabolism – With a healthy diet, rest, and exercise, 1 Body Thyroid Support helps support thyroid he…

- High-Quality Ingredients: Freeze-dried raw, grass-fed bovine thyroid glandular from New Zealand.
- Holistic Support: Aims to support energy levels, metabolism, mental function, mood balance, and sleep quality
- Sustainable Processing: Crafted in a GMP certified facility, our product harnesses low-temperature lyophilization and ca…

- Thyroid Health Nourishment: Our Thyroid Support Complex is a blend of vitamins, minerals, and herbal extracts for optima…
- Optimized Hormone Function: Supports thyroid hormone synthesis and metabolism with iodine, l-tyrosine, and ashwagandha*
- Antioxidant Infusion: Thyroid Support Complex contains vitamin A, C, selenium, and turmeric to support the functioning o…









