Stone man syndrome is a very rare medical condition. It is also termed ‘Fibrodysplasia Ossificans Progressiva‘.
I am sure you haven’t heard of this disease! Worldwide fewer than 1000 cases have been reported.
Stoneman Syndrome is a rare condition that runs in families in an autosomal dominant pattern. It is characterized by bony formation at atypical sites, especially after trauma.
Treatment is supportive, however, Sohonos (Palovarotene) is a retinoid derivative and has been recently approved by the FDA for this disease. It has been approved just a few weeks back!
We present here the story of a young man who presented to our outpatient clinic with bilateral leg swelling and difficulty walking.
The pictures and case report posted here have been published here after proper written and verbal consent of the patient.

Story of a man later diagnosed with Stone man syndrome:
Mr. Ali Mohammed, a 37-years of age, young man, a cook by profession, came to our outpatient clinic with a complex medical history. He complained of difficulty in walking and leg swelling on both sides.
He noticed swelling in both his feet when he was just 9 years of age. He noted that the swelling started insidiously and has progressively worsened over the years.
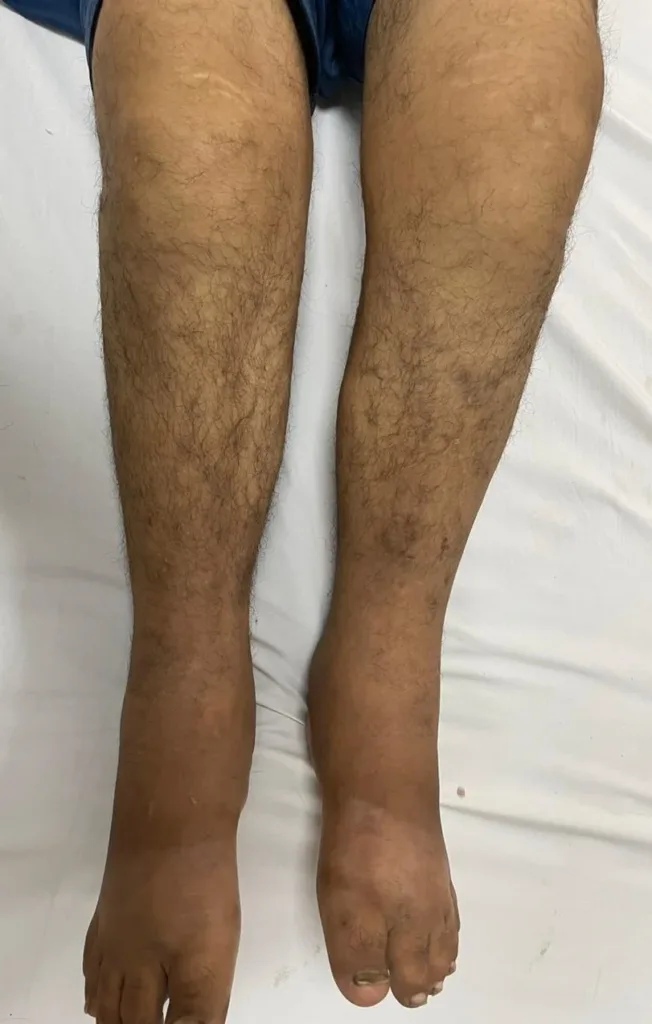
With leg swelling, he found it increasingly difficult to move around and bend his knees. Initially, he attributed it to standing for a longer period of time in the kitchen.
However, he noticed that the swelling in his legs persisted even in the early hours of the day when he would wake up. In addition, he did not have swelling around the eyes.
About a year ago, he fell from stairs while lifting a heavy load after which his limb swelling rapidly progressed and he observed that his feet and lower limbs were getting hard like a bone.
In addition, he also developed a bony swelling around his wrist which became more noticeable with time.
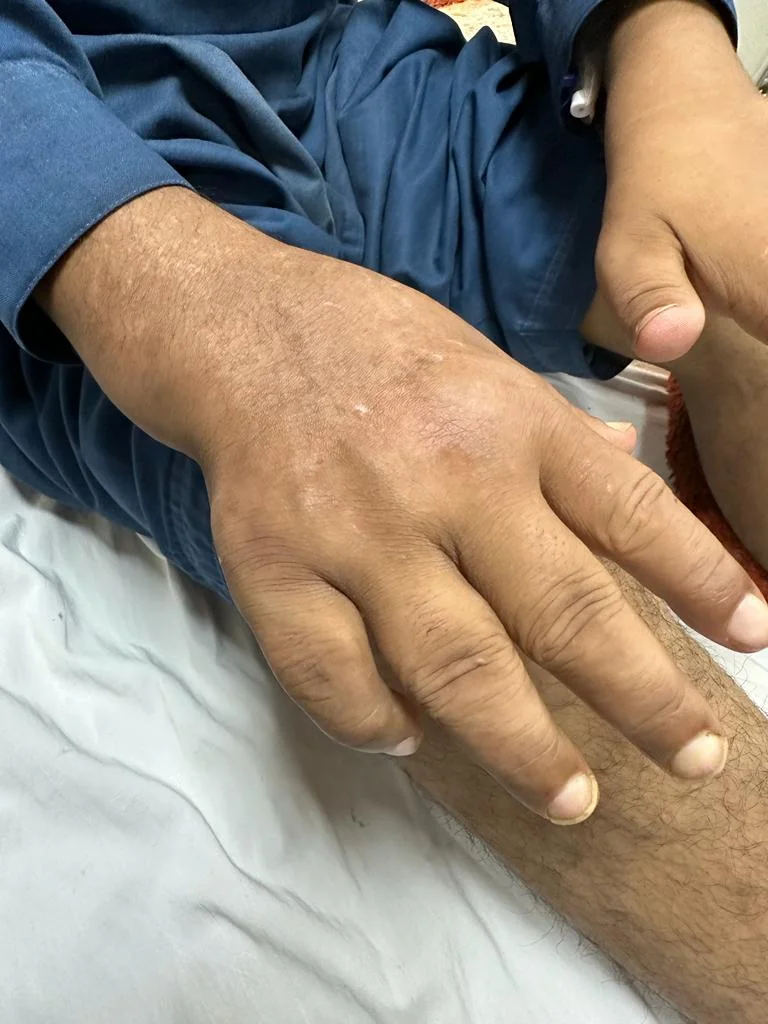
Mr Ali now found it increasingly difficult to move and could barely perform his routine activities. In addition, he started having pain in the legs and body.
He reported a significant unintentional weight loss of approximately 30 kilograms over the past year despite the fact that his appetite remained normal.
He did not give any history of difficulty swallowing, fever, cough, night sweats, swelling of the joints, and early morning stiffness.
He also did not report shortness of breath on lying down or on exertion, heat or cold intolerance, altered bowel habits, or urinary symptoms.
He did not smoke or use any drugs or alcohol and did not have diabetes, hypertension, lung disease, cancers, or any other chronic medical or surgical conditions.
Mr Ali is married with two sons and a daughter who are healthy. His elder sister died of a similar condition but she remained undiagnosed till the last.
There is no family history of cancers, joint diseases, kidney, or heart diseases.
On Examination;
Mr. Ali was lying comfortably in a flexed posture, and upon attempting to extend his knee joints fully, he was unable to do so.
His lower body, particularly his lower limbs, exhibited marked swelling. Notably, the swelling was hard and felt as if pressing a bone.

The skin overlying the swollen areas appeared normal without redness or raised temperature. Pulses in the lower limbs were difficult to feel but they were not cold and the capillary refill time was normal.
He could not extend his legs fully and would bend them partially and with extreme difficulty. He had prominent tibial tuberosities. Movements in his lower limbs were restricted at the ankle, knee, and hip joints.
He could not perform Schoeber’s test as he could not bend his spine. In addition, he would move his neck with difficulty.
In addition, he had a discrete swelling around his right wrist but it was not related to the wrist joint.
He seemed to have a normal height and weight. His body seemed proportionate and examination did not suggest hypothyroidism, hyperthyroidism, kidney or heart disease, joint diseases such as Rheumatoid arthritis or ankylosing spondylitis, acromegaly, or other endocrine disease.
Differential Diagnosis:
Keeping in view the hard swollen legs, bony deformities, limitation in movements with a progressive disease pattern, and possible family history, we thought of the following differential diagnosis:
- Fibrodysplasia Ossificans Progressiva or Stone man disease
- Mucopolysaccharidosis
- Acromegaly
- Pagets disease
- Hypothyroidism
Fibrodysplasia Ossificans Progressiva or Stone Man syndrome was our top differential diagnosis as the swelling in the lower limbs was very different.
It was bony hard and to be very honest we had not seen similar swelling in the past with any of the above-mentioned endocrine conditions or systemic diseases.
In addition, there were other discrete bony swellings and a possible family history too.
Mucopolysaccharidosis was another differential, however, Mr. Ali had a normal height, the axial skeleton and limbs seemed proportionate, and he had no corneal clouding, significant spine disease, hepatosplenomegaly, or heart disease.
Acromegaly was kept in the differential diagnosis but features suggestive of acromegaly such as prominent maxillary bones, wide teeth spaces, enlarged tongue, hoarse voice, large hands and feet, diabetes, and hypertension were not present.
Paget’s disease can present with discrete bony swellings but he had diffuse bony swelling of the limbs without hearing problems or change in skull size.
Hypothyroidism was down in the list of the differential diagnosis but features were not suggestive and it was ruled out as Thyroid function tests were normal.
| Read: |
What is Stone Man Syndrome?
Stone Man Syndrome is a rare condition characterized by calcium deposition and new bone formation at sites other than the bones.
Various case reports of Stone Man Syndrome have emphasized the presence of an abnormal big toe, however, our patient did not have any such finding.
In addition, most case reports are about children and adolescents while our patient is an adult who presented to us at the age of 37 years.
Here are some x-rays of our patient with stone man syndrome:

You can see obvious calcification close to the medial aspect of the radius extending to the thumb.
Below is the x-ray of the legs. There is obvious calcification of the muscles and soft tissues of the legs. These calcifications are very dense and diffuse.
You can also compare the extra-skeletal calcifications with the bones. Despite the diffuse calcifications, the bones do not seem very dense.
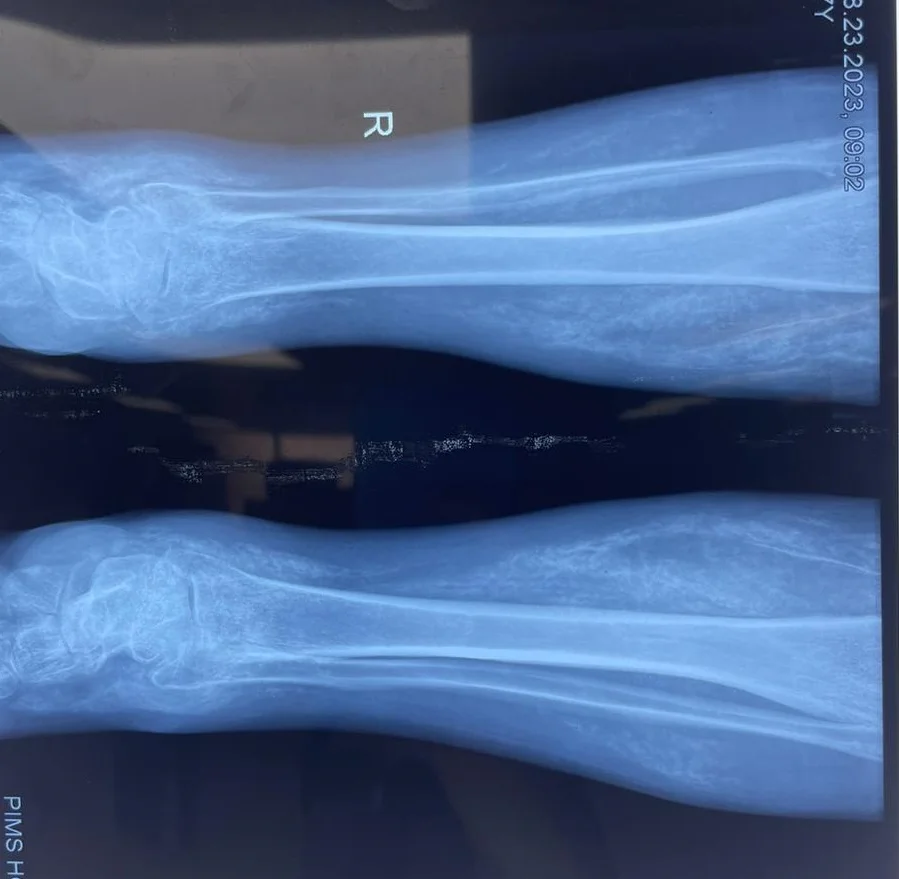
Here is another x-ray showing diffuse ossification of the leg muscles which is almost becoming like a bone. The density is almost comparable to the tibia and fibula.

Calcifications in the pictures below are not very obvious here probably the x-ray position but it is obvious in the palmar aspect of the wrist joint.

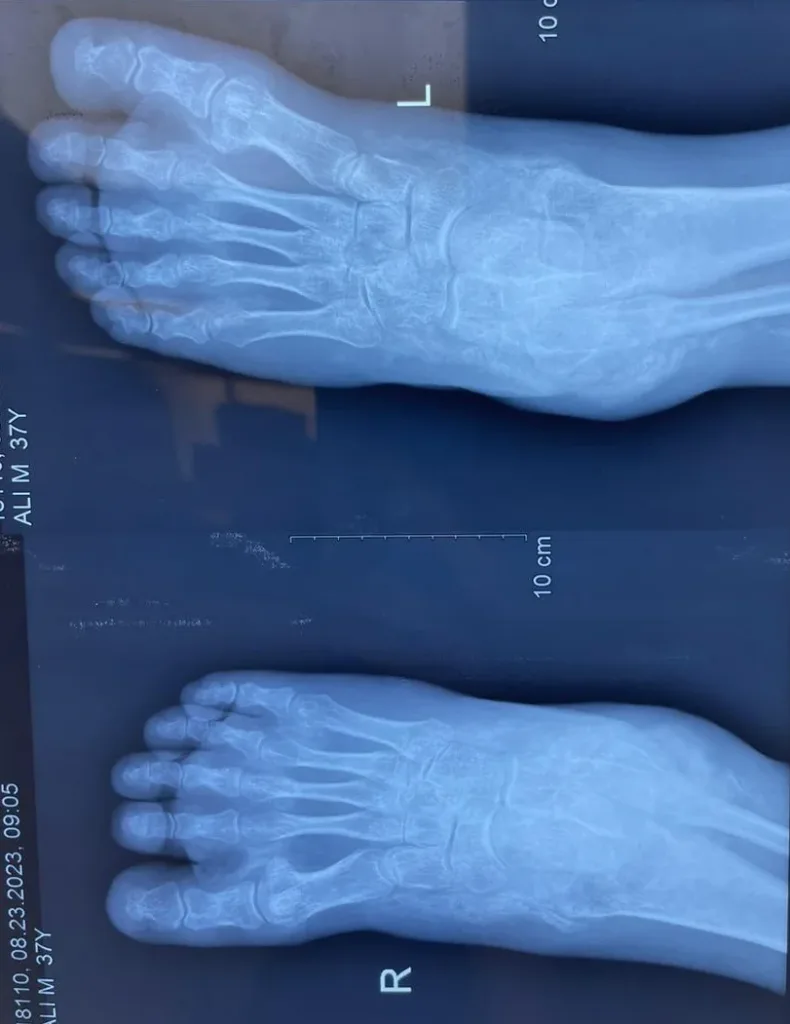
Another x-ray of the feet. The bones are like a heap of calcium, especially the tarsal bones which can not be identified separately.
Bone Scan of Stone Man Syndrome:
Bone scan of our patient was done with 740 MBq of Tc-99m MDP injection. Findings revealed intensely increased tracer uptake in soft tissues of gluteal regions and both lower limbs.
There was also mildly increased tracer uptake in both hands, humorous, spine, and ribs.
Here is the bone scan of the patient with Stone Man Syndrome:

Treatment of Stone man syndrome:
The treatment of stone man disease is supportive. However, retinoids have been tried and may prevent new bone formation.
Last month (August 2023), the FDA approved Sohonos (Palovarotene) for the treatment of Stone Man syndrome.
The drug may prevent new bone formation and is available as oral tablets. It is given in a dose of 5 mg daily.
After trauma, the dose is increased to 20 mg per day for 4 weeks and then 10 mg per day for 8 weeks.
The most important step in the management is avoiding trauma, surgeries, and any invasive procedure. Even physiotherapy should be done very gently. Aggressive physiotherapy should also be avoided.
We have mailed the drug’s manufacturer to help out this patient and hope to get a reply soon.
In summary:
Stoneman syndrome is a rare autosomal dominant condition characterized by new bone formation at sites other than the bones.
Patients should avoid trauma and unnecessary surgeries. Gentle physiotherapy and NSAIDs may help.
Retinoids may help too, hence, all eyes are on the new FDA-approved medicine SOHONOS.
| Read: |




