Neuroendocrine Pancreatic Cancer is a type of cancer that arises from the neuroendocrine cells of the pancreas. Most of these cancers produce active substances and hormones that have distinct clinical manifestations.
Neuroendocrine cells are found in other organs as well. These include the adrenal gland, pituitary, and parathyroid gland.
However, most neuroendocrine tumors arise from the pancreas. There are about 8 neuroendocrine pancreatic tumors identified.
These are summarized in the table below [Ref]:
Neuroendocrine Pancreatic Cancer | Cell Type | Hormone | Symptoms |
| Insulinoma | B | Insulin | Hypoglycemia |
| Gastrinoma | G | Gastrin | ZES (Zollinger Ellison Syndrome) |
| VIPoma | D1 | VIP | Diarrhea, Hypokalemia |
| Glucagonoma | A | Glucagon | Diabetes, Rash, erythema |
| Somatostatinoma | D | Somatostatin | Diabetes, Diarrhea, gallstones |
| GFRoma | PP | GHRH | Acromegaly |
| ACTHoma | NT | ACTH | Cushing’s syndrome |
| Carcinoid | EC | Serotonin | Diarrhea, asthma, flushing |
| You may also like to read: |
What is a Neuroendocrine Pancreatic Cancer?
As the name suggests, Neuroendocrine Pancreatic Cancer or Pancreatic Neuroendocrine Tumors (PNETs) arise from the neuroendocrine cells present in the pancreas.
These cells secrete active substances and therefore have distinct clinical manifestations. Although rare, they account for up to 2% of all pancreatic cancers and often have a good outcome compared to deadly pancreatic cancers other than the PNETs.
From where does Neuroendocrine Pancreatic Cancer arise?
Neuroendocrine cells are a unique type of cells present mostly in the pancreas. Neuroendocrine Pancreatic tumors are cancers that originate from neuroendocrine cells present in the pancreas.
The pancreas contains islets, which are condensed collections of neuroendocrine cells, also known as endocrine cells.
Important chemicals like insulin and glucagon, which help regulate blood sugar levels, are produced by these islets and released into circulation immediately.
Exocrine cells are different types of cells that make up the majority of the pancreas. Pancreatic enzymes are produced by the exocrine glands and secreted into the intestines to aid in food digestion (especially fats).
Adenocarcinoma of the pancreas, the most common form of pancreatic cancer, arse from these exocrine cells.
| You may also like to read: |
Non-functioning Pancreatic Neuroendocrine Cancer:
Non-functioning pancreatic neuroendocrine tumors are the most common kind (60–90%) of pancreatic neuroendocrine tumors.
Hormone production does not increase. On rare occasions, they can produce signs that resemble those of pancreatic ductal adenocarcinoma. These include discomfort, loss of weight, jaundice, and diarrhea.
A non-functioning neuroendocrine pancreatic cancer is difficult to localize and remove. This is due to the lack of recognizable symptoms they produce. They are frequently discovered during examinations for another issue.
| You may also like to read: |
Functioning neuroendocrine pancreatic cancer:
A functioning pancreatic neuroendocrine cancer is one that produces an active substance resulting in particular clinical manifestations.
About 30% of pancreatic neuroendocrine cancers are functional and produce some form of chemicals or hormones [Ref].
The hormones that are produced by around half of the pancreatic NETs are released into circulation and result in symptoms. These are referred to as functioning NETs. Each one bears the name of the hormone that the tumor cells produce.
Gastrinomas:
Pancreas and duodenal gastrinomas are common (first part of the small intestine). They overproduce gastrin, a hormone found in the intestines. The production of too much stomach acid is indicated by high levels of gastrin.
Chest and/or stomach discomfort, acid reflux, heartburn, diarrhea, and fatigue are among the symptoms that may be present.
The Zollinger-Ellison syndrome is the collective name for these symptoms. Additionally, too much gastrin might irritate the stomach or duodenum, which can result in ulcers and bleeding.
| You may also like to read: |
Insulinomas:
Any part of the pancreas can develop an insulinoma. They produce excessive amounts of the hormone insulin, which lowers blood sugar.
Dizziness, lightheadedness, perspiration, hunger, confusion, and irritability are just a few signs of low blood sugar.
Insulinomas produce insulin and so patients develop hypoglycemia and weight gain.
| You may also like to read: |
VIPomas:
VIPomas are more prevalent in the tail of the pancreas. These PNETs produce an excessive amount of the hormone, vasoactive intestinal peptide (VIP).
VIP in physiological amounts help in the digestion, balancing of stomach acid, and regulating how quickly food travels through the bowels.
Numerous bouts of watery diarrhea, dehydration, low potassium levels in the blood (hypokalaemia), abdominal ache, bloating, and a flushed face are among the signs and symptoms.
VIPomas may present with profuse watery diarrhea. Because of the profuse watery diarrhea, it is also referred to as pancreatic cholera.
| You may also like to read: |
Glucagonomas:
The body & tail of the pancreas contains the majority of the glucagonomas. They produce an excessive amount of the gastrointestinal hormone glucagon, which helps regulate blood sugar.
Unusual skin rash (redness and blisters), especially on the face, abdomen, and feet, is one of the symptoms.
Diabetes (high blood sugar levels), diarrhea, weight loss, mood swings, anemia (low amounts of red blood cells), blood clots, and irritated lips and tongue are further symptoms of glucagonomas.
The classic triad of Glucagonomas includes:
- High amounts of glucagon in the blood
- Diabetes, and
- NME (Necrolytic migratory erythema)
| You may also like to read: |
ACTHomas:
ACTHomas that overproduce ACTH (adrenocorticotropic hormone). Weight gain, easy bruising, anemia, depression, an elevated risk of infection, and darker skin are just a few of the Cushings disease symptoms that can result from this.
Ppomas:
Ppomas generate an excessive amount of pancreatic polypeptide. Diarrhea, stomach discomfort, and weight loss are just a few of the symptoms that might result from this.
Somatostatinomas:
Somatostatin-overproducing cancers are called somatostatinomas. This might result in symptoms including gallstones, steatorrhoea (pale, fatty stool), anemia, stomach discomfort, high blood sugar levels, and jaundice.
Carcinoid tumors:
Although they seldom ever begin in the pancreas, these NETs are far more prevalent in other regions of the digestive system. These tumors produce serotonin often.
| You may also like to read: |
Pancreatic Neuroendocrine Cancer Grading:
The tumor grade of pancreatic neuroendocrine tumors (NETs) indicates how quickly the cancer is likely to advance and spread.
Grade 1:
Neuroendocrine tumors, often known as low-grade or well-differentiated tumors, have cells that resemble normal cells more and do not grow rapidly.
Grade 2:
Cancers that fall within the categories of low- and high-grade tumors are referred to be intermediate-grade or moderately differentiated tumors.
Grade 3:
Neuroendocrine tumors, often known as high-grade or poorly differentiated tumors, have cells that look incredibly aberrant and are proliferating more quickly.
Note: Pancreatic neuroendocrine tumors of grade 1 or 2 can expand to other places of the body but typically progress slowly. Pancreatic neuroendocrine carcinomas of grade three spread to other body areas and have a tendency to develop and spread rapidly.
| You may also like to read: |
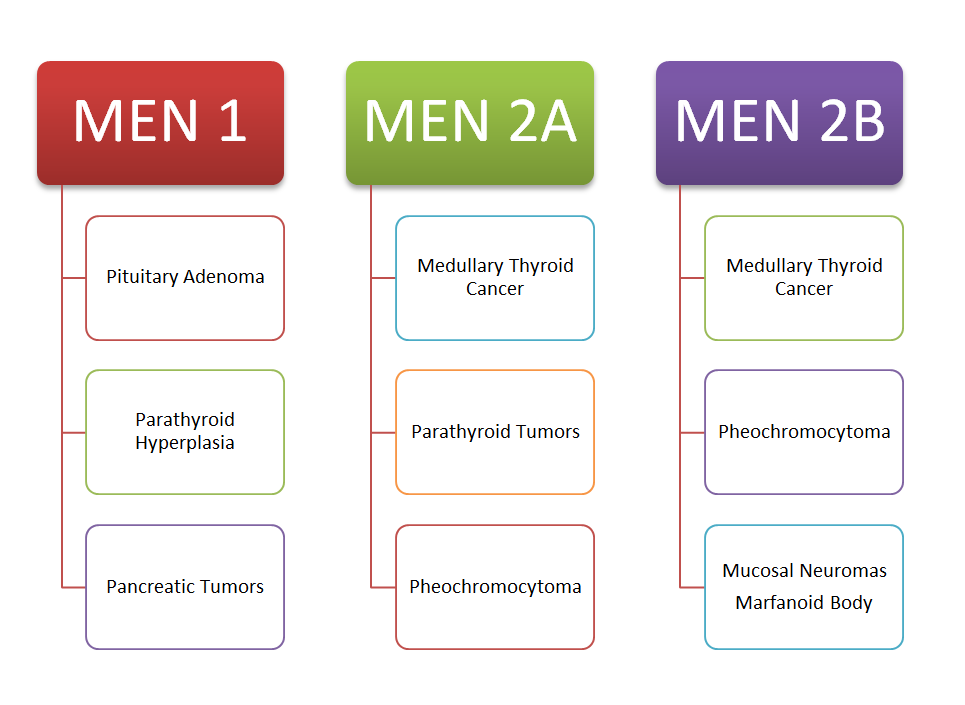
In addition, if a person is diagnosed with pancreatic neuroendocrine cancer, he/ she should also be screened for other neuroendocrine cancers as well. These are classically described in the MEN syndromes.