Traditionally, there are four Diabetes Types: Type 1 Diabetes, Type 2 Diabetes, Gestational Diabetes, and LADA (latent autoimmune diabetes of adults).
Gestational diabetes develops during pregnancy and is otherwise similar to Type 2 Diabetes.
Type 1 Diabetes, Type 2 Diabetes, and LADA can be differentiated based on the degree of insulin production, insulin resistance, and the presence of autoantibodies against the beta islet cells.
Lately, scientists grouped patients with Type 2 Diabetes into 5 different clusters. These clusters have different glycemic profiles.
In addition, diabetes-associated complications especially kidney disease and diabetic retinopathy are more common in certain clusters than others.
Differentiating Between the Different Diabetes Types:
Historically, diabetes has been classified as either Type 1 diabetes which manifests at a younger age, and patients have positive autoantibodies against the pancreatic islet Beta cells.
Type 2 diabetes is usually diagnosed when autoantibodies are absent and the patients are usually older.
LADA (latent autoimmune diabetes of adults) is similar to type 2 diabetes at diagnosis but is indistinguishable from type 1 diabetes later on. Patients with LADA also have positive anti-glutamic acid decarboxylase antibodies.
A group of Swedish scientists classified type 2 diabetes into 5 different clusters based on the following 6 variables [Ref]:
- glutamate decarboxylase antibodies,
- age at diagnosis,
- BMI,
- HbA1c,
- homeostatic model assessment 2 estimates
of β-cell function and - Insulin resistance
3 Types of Diabetes were diagnosed:
- Type 1 diabetes was defined when C-peptide levels were less than 0.3 mmol/L and GADA positive (glutamic acid decarboxylase antibodies)
- LADA (latent autoimmune diabetes of adults) was defined as C-peptide levels of 0.3 mmol/L or more and GADA positive.
- Type 2 Diabetes, with C-peptide higher than 0.3 mmol/L and GADA negative were further grouped into 5 clusters.
| Read: |
The 5 clusters of Type 2 Diabetes mellitus:
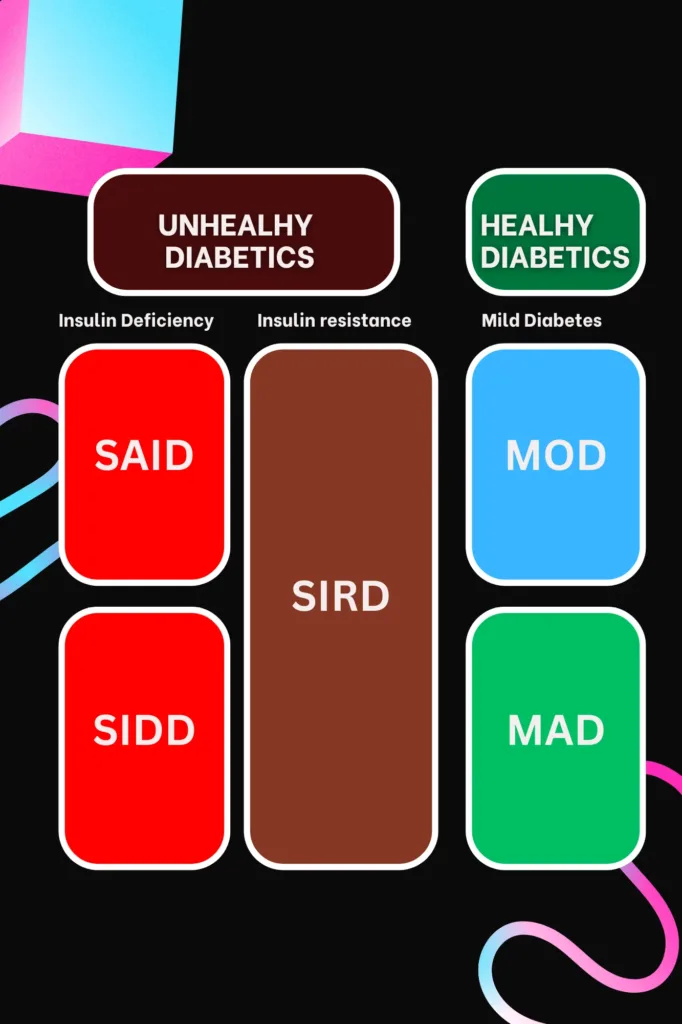
Patients with type 2 diabetes were further grouped into 5 clusters based on their glycemic profiles, insulin production, and insulin sensitivity.
SAID (Severe Autoimmune Diabetes): Cluster 1 characterized by:
- Early-onset disease,
- Relatively low BMI,
- Poor metabolic control,
- Insulin deficiency, and
- the presence of GADA
SIDD (Severe Insulin Deficient Diabetes): Cluster 2 characterized by:
- GADA negative (but otherwise similar to cluster 1)
- Onset at a younger age
- Low BMI
- Insulin Deficiency, and
- Poor metabolic control
SIRD (Severe Insulin Resistant Diabetes): Cluster 3 characterized by:
- Insulin resistance
- High BMI
MOD (mild obesity-related diabetes): Cluster 4 characterized by:
- Obesity
- No insulin resistance
MARD (mild age-related diabetes) or MAD: Cluster 5 characterized by:
- Older patients
- No insulin resistance
- Only modest metabolic derangements
| Read: |
Clinical Implications of the 5 Clusters of Type 2 Diabetes:
The 5 clusters of diabetes had significant variations in their diabetes profiles and associated complications.
The table below shows the clinical differences between the 5 clusters of diabetes:
Clinical Implication | Prevalence in different clusters |
| HbA1c at Diagnosis and Ketoacidosis | Clusters 1 and 2 had higher HbA1c and more ketoacidosis at diagnosis compared to other clusters. |
| Non-Alcoholic Fatty Liver Disease | Cluster 3 had the highest prevalence of non-alcoholic fatty liver disease. |
| Autoantibodies (ZnT8A) | ZnT8A autoantibodies were primarily seen in patients with SAID. |
| Insulin Prescription at Registration | Clusters 1 and 2 had higher proportions of patients prescribed insulin compared to clusters 3-5. |
| Metformin Use and Traditional Classification | Cluster 2 had the highest metformin use, cluster 1 was least likely to use metformin, Cluster 3 had low metformin use despite the most expected benefits in this cluster. |
| Kidney Disease Risk | Cluster 3 had the highest risk of developing chronic kidney disease and diabetic kidney disease. |
| Diabetic Retinopathy | Early signs of diabetic retinopathy were more common in cluster 2 compared to other clusters. |
| Coronary Events and Stroke Risk | No significant difference between clusters in age-adjusted and sex-adjusted risk. |
| Genetic Associations | Different genetic variants were associated with different clusters, indicating genetic heterogeneity. |
Insulin prescription was predominantly observed in patients categorized within clusters 1 and 2, whereas clusters 3, 4, and 5 exhibited a lower likelihood of being prescribed insulin.
Patients belonging to cluster 2 demonstrated the briefest duration to administering a second oral diabetes treatment.
They concurrently exhibited the lengthiest period to achieve the treatment goal defined by an HbA1c level of less than 6.9%.
Clusters 1, 2, and 4 displayed the lowest incidence of coronary events and strokes.
The association of the TM6SF2 gene with SIRD, but not with MOD, implies a propensity for unhealthy obesity (specifically, metabolic syndrome) among individuals characterized by SIRD.
| Read: |
In Summary:
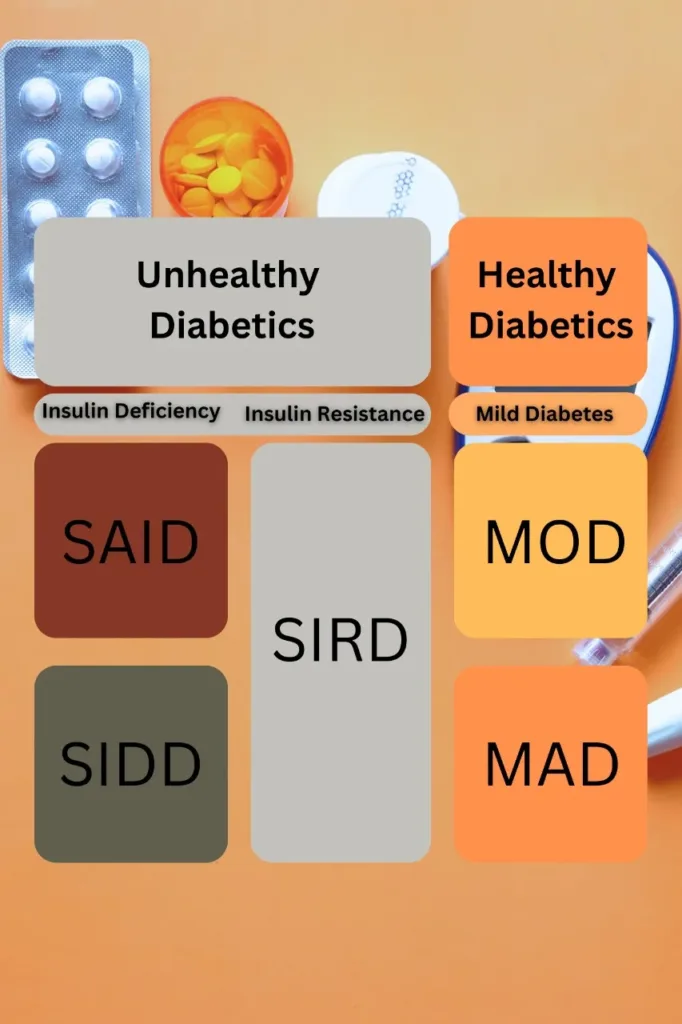
The 5 clusters of diabetes are summarized here in a table format:
Clusters | Clinical Features |
1. SAID |
|
2. SIDD |
|
3. SIRD |
|
4. MOD |
|
5. MARD or MAD |
|
SAID (severe autoimmune diabetes) overlapped with Type 1 diabetes and LADA.
SIDD (severe insulin-deficient diabetes) and SIRD (severe insulin-resistant diabetes) are two severe forms of type 2 diabetes.
Retinopathy was predominantly seen in SIDD (severe insulin-deficient diabetes) while kidney disease was strongly associated with severe insulin-resistant diabetes (SIRD).
Despite optimal glucose control, diabetic kidney disease developed in patients in cluster 3. Insulin resistance was the hallmark of cluster 3 and this association was thought to trigger kidney disease.
| Read: |



