Breast cancer survival rate is determined by multiple good and bad prognostic factors. The survival or mortality rate is usually described in terms of the percentage of surviving patients after 5 or 10 years and the recurrence rates.
Breast cancer survival rate has improved over the years by about 39% over the last 3 decades. This is because of increased awareness, early diagnosis, and better treatment modalities.
Here are Some Factors that Influence Breast Cancer Survival Rate:
The overall 5-year survival rate of breast cancer as per the 2023 statistics is 90.8%.
This means that out of 100 women diagnosed with breast cancer, 91 women are likely to live for up to 5 years and beyond regardless of their ages, tumor size, stage of breast cancer, or other factors.
Many factors influence breast cancer survival rate. Here are some of the good and bad prognostic indicators of breast cancer survival rate:
Age of the patient:
Breast cancer in women affects mostly middle-aged females. More than half of the women diagnosed with breast cancer are between 55 to 74 years of age.
Here is a table showing the incidence of breast cancer in women by age:
Age | % of new cases by age |
| <20 | – |
| 20 -34 | 2% |
| 35 – 44 | 8.3% |
| 45 – 54 | 18.5% |
| 55 – 64 | 25.4% |
| 65 – 74 | 26.8% |
| 75 – 84 | 13.9% |
| >84 | 5.1% |
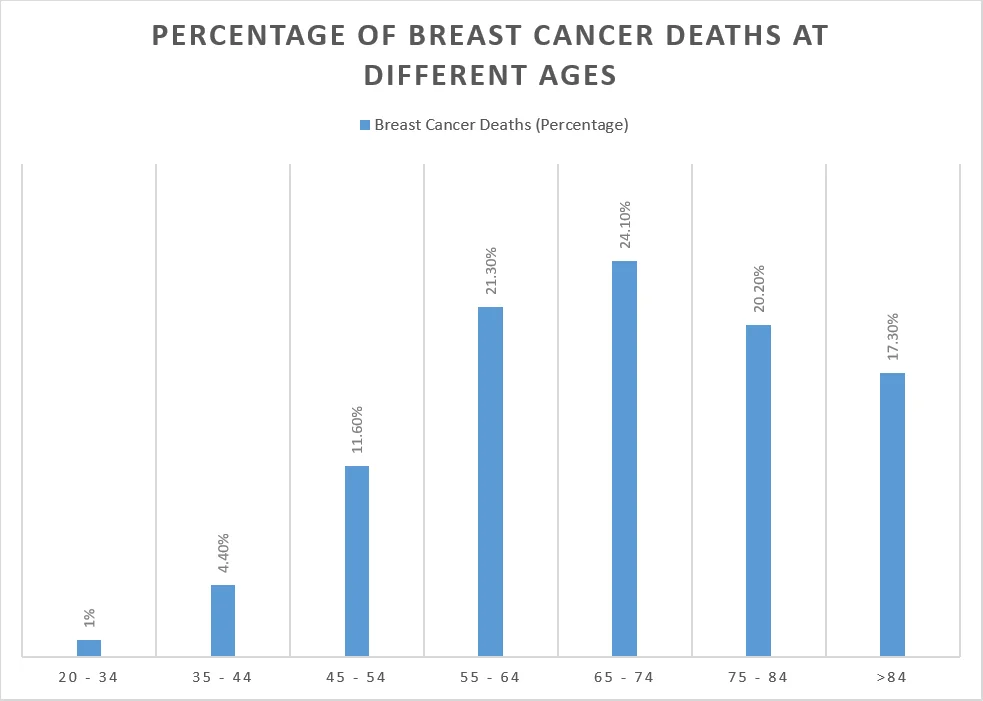
The death rates in women with breast cancer increase with increasing age. Younger age is associated with a better prognosis.
However, the prognosis depends on multiple factors other than the age.
Age (Years) | Breast Cancer Deaths (Percentage) |
| 20 – 34 | 1% |
| 35 – 44 | 4.4% |
| 45 – 54 | 11.6% |
| 55 – 64 | 21.3% |
| 65 – 74 | 24.1% |
| 75 – 84 | 20.2% |
| >84 | 17.3% |
The median age of at death is 70 years.
| Read: |
Stage of Breast Cancer:
The stage of breast cancer is one of the most important factors influencing survival rate. Stage 1 cancer, also called localized tumor which has not spread to distant parts of the body or lymph nodes has the best prognosis.
The 5-year survival rate of a localized breast cancer is 99.3%. In simple words, almost all women who are diagnosed with breast cancer in the early localized stage (Stage 1) are going to survive for 5 years or more.
In contrast to women with regional or distant spread of the tumor, the survival rates decline tremendously.
The 5-year survival rate of women with regional spread of breast cancer is 86.3%, and those with distant spread is 31%.
Age | Breast Cancer % 5-year Survival Rate |
| Localized Cancer | 99.3% |
| Regional Spread of Cancer | 86.3% |
| Distant Spread of Cancer | 31% |
| Unknown | 70.2% |
| Read: |
Size of the tumor:
The size of breast cancer affects the survival rates. Breast cancer that is smaller than 1 cm and has not spread has a very favorable prognosis compared to breast cancer of 5 cm or larger.
In the TNM staging of breast cancer, “T” refers to tumor size. This signifies the importance of tumor size at diagnosis [Ref].
- TX: Can not assess the primary tumor.
- T0: Primary tumor not detected.
- T1: The tumor is less than 2 cm in size.
- T2: The tumor is 2 to 5 cm in size.
- T3: The tumor is larger than 5 cm in size.
- T4: The tumor has extended to the chest wall or skin. Can be of any size.
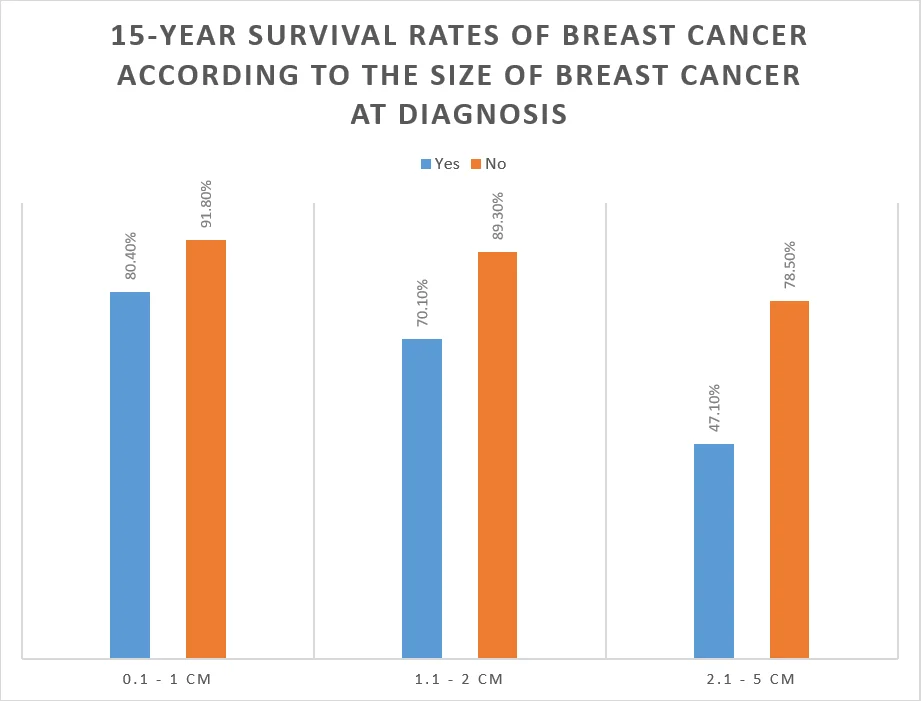
In one study, the 15-year survival was observed to be greatly reduced when the tumor size at diagnosis was more than 2 cm, especially in women with lymph node involvement [Ref]:
| Tumor Size at Diagnosis | Node Involvement | 15 years survival |
| 0.1 – 1 cm | Yes | 80.4% |
| No | 91.8% | |
| 1.1 – 2 cm | Yes | 70.1% |
| No | 89.3% | |
| 2.1 – 5 cm | Yes | 47.1% |
| No | 78.5% |
| Read: |
Spread of the tumor:
The Spread of the tumor is commonly described in medical terms as “metastasis”. Metastasis is probably the most significant factor in predicting a 5-year survival rate in women with breast cancer.
Although other factors play a significant role, generally, the 5-year survival is estimated to be around 30% in women with metastatic breast cancer.
In the TNM staging, M0 is when there is no evidence of the spread of the breast cancer while M1 is when the breast cancer has spread to any part of the body such as the liver, lungs, or brain.
The 5-year survival rate in women with regional spread of breast cancer is about 86% while that of distant spread is 29 – 30%.
However, the survival rates differ depending on the site and organ where the cancer has spread.
The table below shows the breast cancer survival rates after it spreads to distant organs:
Spread of Cancer | Breast Cancer Survival Rates |
| Sternum | 10-year survival after Sternectomy: 41.8% Median survival: 9 months after recurrence [Ref] |
| Eye (Orbit) | Mean survival after diagnosis is 22 months [Ref] |
| Neck | The median survival after diagnosis of neck metastasis is 21 months |
| Pancreas | 1 – 50 months [Ref] |
| Stomach | 24 – 36 months [Ref] |
| Brain | 2 – 27 months |
| Bone | 1-year survival rate: 51% Median survival:
Stage 4 breast cancer spread to bones survival rate at 1, 3, and 5 years
|
| Liver | 5-year survival: 37% [Ref] |
In one study, breast cancer spread to the liver had a very poor prognosis [Ref]
Breast cancer with liver metastasis | Median survival (months) |
| Liver Metastasis | Single: 10.34 months Multiple: 4.6 months |
| Liver and Bone | 3.87 months |
| Liver and lung | 5.75 months |
| Liver and pleura | 4.27 months |
| Read: |
Lymph node involvement:
Lymph node involvement is another major prognostic indicator of survival in women with breast cancer.
Because of its association with survival, nodal positivity has been added to the TNM staging of breast cancer.
The “N” in the “TNM” staging of breast cancer denotes “Node involvement”.
Nodal involvement can be:
- Nx: Nodes can not be assessed
- N0: Nodes are free of the disease
- N1, 2, or 3: Nodes are positive
- N1: 1 – 3 nodes involved
- N2: 4 – 9 nodes involved
- N3: 10 or more nodes involved
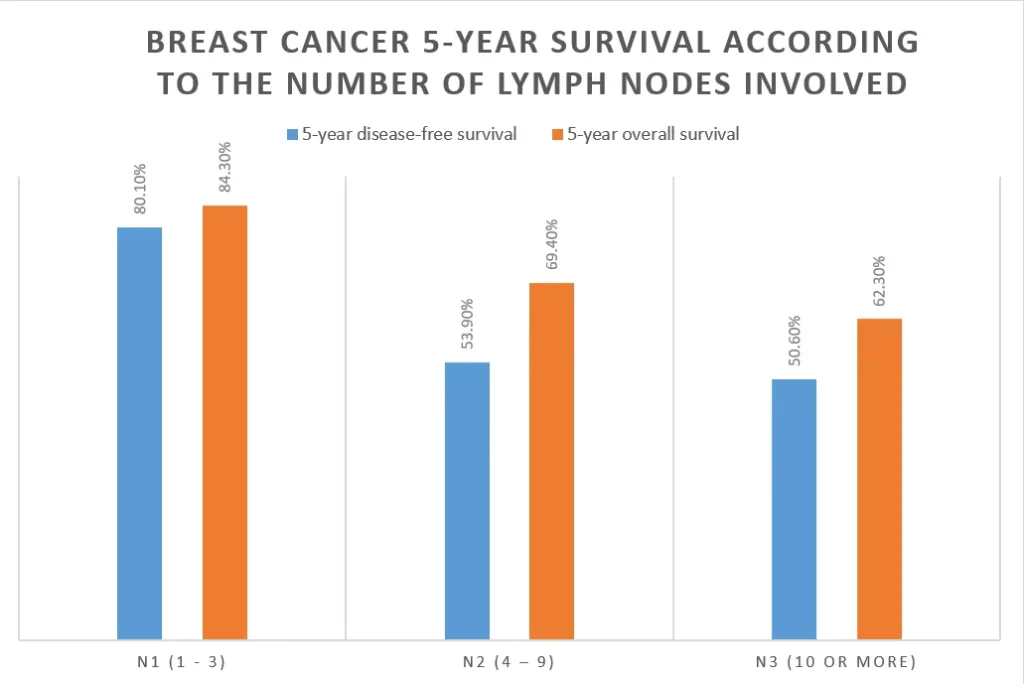
In one study, the 5-year breast cancer survival rate was determined in a cohort of 628 women with node-positive breast cancer.
The results are given in the table below:
Lymph node Involvement | 5-year disease-free survival | 5-year overall survival |
| N1 (1 – 3) | 80.1% | 84.3% |
| N2 (4 – 9) | 53.9% | 69.4% |
| N3 (10 or more) | 50.6% | 62.3% |
In another study, LNR (Ratio of lymph nodes positive to total lymph nodes examined) was used to assess the 10-year breast cancer survival rate.
Patients were divided into low, intermediate, and high-risk groups. The 10-year survival in the three groups is given below:
Lymph node Ratio (LNR) | 10-year disease-free survival |
| Low (0.2 or Less) | 80.1% |
| Intermediate (>0.2 – <0.65) | 53.9% |
| High (>0.65) | 50.6% |
The 10-year disease-free survival is greatly reduced in the high-risk groups.
| Read: |
The type of breast cancer:
The WHO has classified breast cancer into 21 different histologic subtypes. Of these, invasive ductal breast carcinoma of no special type (NST) is the most common [Ref]
Breast cancer with favorable histologic types include [Ref]:
Breast Cancer Type | 5-Year Survival Rate | 10-Year Survival Rate |
| Pure Mucinous Carcinoma | 94% | 89% |
| Tubular Carcinoma | 94% | – |
| Invasive Cribriform Carcinomas | Excellent | – |
| Neuroendocrine Carcinoma | Up to 0.5% | Favorable |
| Medullary Carcinoma | Generally good | 95% |
| Adenoid Cystic Carcinoma | 90% | – |
| Secretory Breast Carcinoma | Extremely rare | Favorable |
Apocrine carcinoma has an intermediate prognosis. Breast cancer with the worst prognosis according to histologic subtypes include [Ref]:
- Pleomorphic Lobular Carcinoma
- Invasive Micropapillary Carcinoma
- Metaplastic Carcinoma
- High-Grade Small Cell Neuroendocrine Carcinoma
| Read: |
Histologic grade of the tumor:
Histologic grade has a lot of inter-observer variability. There are three different histologic grades of breast cancer.
Grade 1 breast cancer is well differentiated with few mitotic processes while grade 3 is the least differentiated and abundant of mitotic processes.
The higher the grade of the tumor, the poorer the prognosis [Ref]:
- Grade 1 breast cancer: Good prognosis and better survival rates
- Grade 2 breast cancer: Intermediate prognosis and survival rates
- Grade 3 breast cancer: Poor prognosis and survival rates
| Read: |
The response to treatment:
A patient’s response to treatment significantly relates to overall survival rates. Patients who have a good response to chemotherapy or neoadjuvant therapy have better survival compared to patients who have a progression of the disease.
Women who have disease progression in terms of an increase in tumor size, spread to local or distant organs of the body, or develop intolerance to medications do less well and have poor overall survival compared to women who tolerate the medicines and whose tumors shrink with treatment.
Estrogen and Progesterone receptor status (ER/PR positive or negative):
Estrogen and progesterone receptor status have been strongly linked with survival rates. Generally speaking, women with ER and PR-positive breast cancers have a better prognosis.
In addition, ER and PR status are usually seen with HER-2 expression. Hence women with breast cancer can have any of the combinations:
ER/PR/HER-2 status | ER | PR | HER-2 |
| ER+/PR+/HER-2 + (Triple positive) | +ve | +ve | +ve |
| ER+/PR+/HER-2 – | +ve | +ve | -ve |
| ER+/PR-/HER-2 – | +ve | -ve | -ve |
| ER-/PR+/HER-2 + | -ve | +ve | +ve |
| ER-/PR-/HER-2 + | -ve | -ve | +ve |
| ER-/PR-/HER-2 – (Triple negative) | -ve | -ve | -ve |
| ER-/PR+/HER-2 – | -ve | +ve | -ve |
However, for practical purposes, the following four categories of breast cancer are commonly used to decide the treatment [Ref]:
| Molecular Subtype | Description | 4-year survival rates |
| Luminal A | HR+/HER2- | 92.5% |
| Luminal B | HR+/HER2+ | 90.3% |
| HER2-enriched | HR-/HER2+ | 82.7% |
| Triple Negative | HR-/HER2- | 77% |
HR + means ER and PR positive
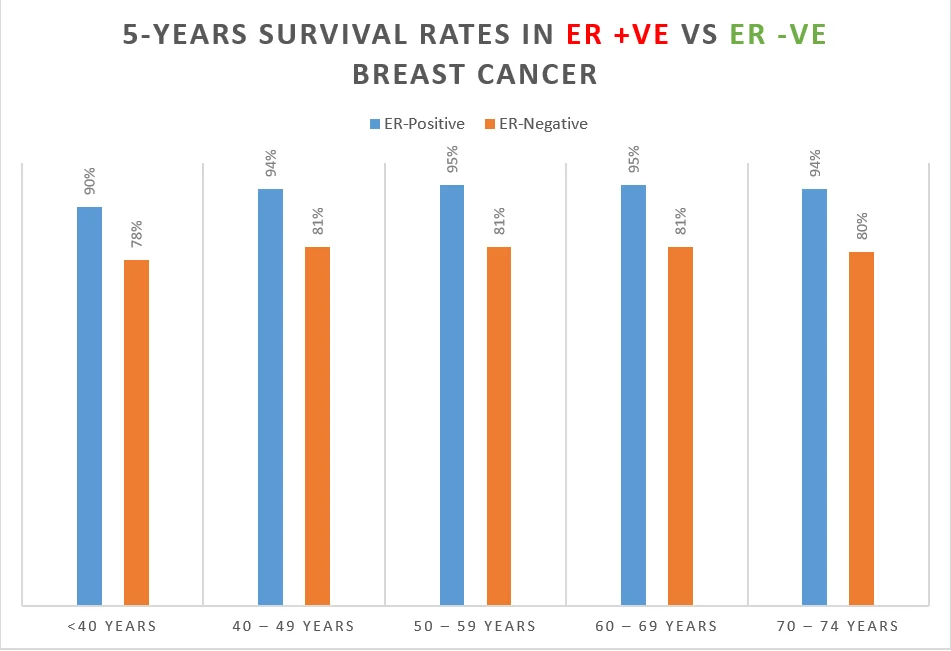
Estrogen receptor (ER) positive breast cancer has a better prognosis compared to women with estrogen-negative breast cancer as shown in the table below [Ref]:
Age of the patient | 5 Year Survival Rates in ER-Positive Breast Cancer | 5 Year Survival Rates in ER-Negative |
| <40 years | 90% | 78% |
| 40 – 49 years | 94% | 81% |
| 50 – 59 years | 95% | 81% |
| 60 – 69 years | 95% | 81% |
| 70 – 74 years | 94% | 80% |
Overall, breast cancer survival at 15 years for ER-positive breast cancer was 77%, and for ER-negative breast cancer was 70%.
The breast cancer survival rates for combined ER+ and PR+ were estimated to be better than hormone-receptor-negative breast cancer [Ref]:
Tumor Type | 5-Year DFS | 10-Year DFS | 5-Year OS | 10-Year OS |
| ER + PR – Tumors | 91.4% | 79.6% | 95.9% | 93.9% |
| ER – PR + Tumors | 81.0% | 73.1% | 95.3% | 88.7% |
DFS: Disease-free survival
OS: Overall survival
The prognosis is best when the breast cancer is Estrogen and Progesterone receptors positive and HER-2 negative.
The overall 5-years survival rates of ER +, PR +, and HER-2 – breast cancer is estimated as 96.7% compared to 82.7% for breast cancers which are ER -, PR -, and HER-2 + [Ref]
| Subtype | 5-Year Survival Rate | 5-years Disease-free survival |
| ER+ PR+ HER-2- | 96.7% | 90% |
| ER- PR- HER-2+ | 82.7% | 73.3% |
| Read: |
HER2 gene expression:
HER-2 expression means the breast cancer cells have “human epidermal growth factor receptor 2” on their surface.
Women who have an extra copy of a gene that encodes for cell surface proteins called HER-2 express these proteins on their surface.
These protein receptors promote the growth and help the spread of breast cancer cells. These proteins are detected by molecular techniques such as FISH (Fluorescence in situ hybridization) and immunohistochemistry.
Hence, women who are positive for HER-2 receptors have a poor prognosis and a shorter survival.
It is estimated that 15 – 20% of all invasive breast cancers (invasive ductal carcinoma and lobular carcinoma are HER-2 positive) [Ref].
HER-2 positivity is an indicator of poor prognosis, however, breast cancer survival rates are best estimated along with ER (estrogen receptors) and PR (progesterone receptors).
HER-2-positive breast cancers have a 5-year survival rate of more than 90% if picked up in the early stages. However, once the disease spreads to distant organs, the survival rates are greatly reduced.
| Read: |
In Conclusion:
Women with breast cancer who are younger, have a small tumor at diagnosis, that has not spread to the lymph nodes, locally, or to distant organs and have a better prognosis and excellent chances of surviving for 5 years or more.
In addition to these traditional prognostic factors, novel markers of survival are being increasingly used. These include Hormone Receptors (HR) and Human Epidermal Growth Factor Receptor- 2 (HER-2).
Women with breast cancer positive for Estrogen and Progesterone (Hormone positive – HR +) have a better prognosis while HER-2 positive breast cancer has a poor prognosis.
Prognostic Factor | Good Prognostic Factors | Bad Prognostic Factors |
| Axillary Lymph Node Status | Node-negative disease | Positive nodes (Number of nodes correlates with recurrence) |
| Tumor Size | Smaller tumor size | Larger tumor size |
| Lymphatic/Vascular Invasion | Absence of invasion | Presence of invasion |
| Patient Age | Younger age | Older age |
| Histologic Grade | Lower grade | Higher grade |
| Histologic Subtypes | Tubular, Mucinous, or Papillary subtypes | Comedo subtype for DCIS |
| Response to Neoadjuvant Therapy | Favorable response | Poor response |
| Hormone Receptor (ER/PR) Status | Positive (responsive to hormone therapy) | Negative |
| HER2 Gene Amplification/Overexpression | Improved prognosis with targeted therapies | Worse prognosis (historically) with no targeted therapies |
| Read: |




